
Data from the massive Vitamin D and Omega-3 Trial (VITAL) show clearly that daily supplementation with 2,000 IU of vitamin D can reduce the incidence of rheumatoid arthritis, polymyalgia rheumatica, and other autoimmune conditions.
Omega-3 fatty acids, at a dose of 1,000 mg per day also mitigated risk, but to a lesser degree.
“Vitamin D supplementation for five years, with or without omega 3 fatty acids, reduced autoimmune disease by 22%, while omega 3 fatty acid supplementation with or without vitamin D reduced the autoimmune disease rate by 15% (which was) not statistically significant,” reports lead investigator Karen Costenbader, Professor of Medicine at Harvard Medical School, and director of the lupus program at Brigham and Women’s Hospital in Boston.
“Both treatment arms showed larger effects than the reference arm (vitamin D placebo and omega 3 fatty acid placebo).”
“The clinical importance of these findings is high because these are well tolerated, non-toxic supplements, and other effective treatments to reduce the incidence of autoimmune diseases are lacking.”
This is the first direct evidence from a large-scale prospective trial looking at supplementation for prevention of autoimmune conditions. The findings were published in mid-January, in the British Medical Journal.

The new paper is the second major report from the ongoing VITAL study. A 2019 paper looking at the effect of Vitamin D on the incidence of cancer and cardiovascular disease showed little effect. Compared with placebo, the supplement did not appear to prevent cardiovascular events, nor did it have any significant impact on overall cancer deaths, or incidence of breast, prostate, or colorectal cancer (Manson JE, et al. NEJM, 2019).
This time around, the VITAL team is delivering good news.
Large, Diverse Cohort
VITAL is nationwide, randomized, double blind, placebo-controlled study involving 25,871 older adults randomized to: daily supplementation with 2,000 IU of vitamin D as cholecalciferol (Pharmavite) plus 1,000 mg of a prescription omega-3 fatty acid formula (Omacor/Lovaza) containing 460 mg of EPA and 380 mg of DHA; vitamin D plus an omega-3 placebo; omega-3s plus a vitamin D placebo; or double placebos.
All VITAL participants were at least 50 years old on entry, with a median age of 67. Across the 4 treatment arms, the gender distribution was nearly 50/50, with equal representation from the Northeast, Midwest, West, and South East.
The cohort was racially diverse, with 20% of participants identifying as Black, and 8% identifying as other non-White ethnicities. They represent a broad range of education and income levels, health status, and lifestyles. The patients were followed for a median of 5.3 years.
The protocol excluded people with a history of renal failure or dialysis, cirrhosis, hypercalcemia, cancer (except non-melanoma skin cancer), cardiovascular disease, or other serious illness. However, roughly one-third of all subjects had family histories of autoimmune diseases, and 18% (n = 4,555) had at least one prior autoimmune diagnosis prior to randomization. The average baseline body mass index was 28.
At the outset, the investigators took blood from all willing participants (n=16 956), and assayed it for 25-hydroxyvitamin D (25-OHD) and plasma omega-3 levels (EPA plus DHA as percentage of total fatty acids).
The authors stress that VITAL is intended to evaluate the impact of vitamin D and omega-3s in a broad sample of American adults, not just those who are deficient in these particular nutrients.
At baseline, roughly 54% had serum 25-OHD levels of 30 ng/ml or greater, while 13% had frank deficiencies with levels below 20 ng/ml. Baseline mean omega-3 Index was 28. Roughly 42% of subjects were taking vitamin D (less than or equal to 800 IU/day) prior to enrolling.
The study’s large and diverse sample size, its clearly defined endpoints, and high adherence rate all give the evidence notable strength.
All participants completed thorough health evaluation questionnaires at six months and then again one year after randomization, with annual evaluations thereafter. Those who reported new incidents of autoimmune disease were asked to authorize release of their medical records, which were thoroughly reviewed by independent physicians, including a board-certified rheumatologist, endocrinologist, and gastroenterologist, to confirm or refute the diagnoses.
Big Impact from Vitamin D

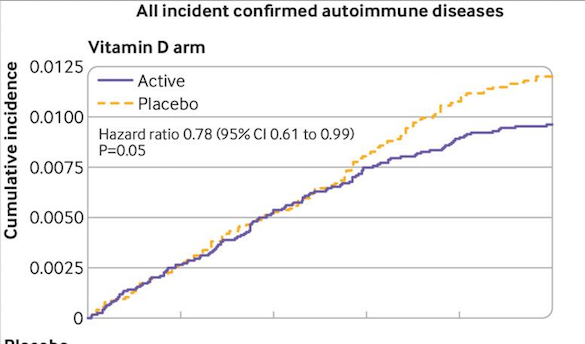
Looking specifically at vitamin D compared with placebo, there were confirmed diagnoses of new autoimmune diseases in 123 participants in the treatment group (0.95%) and 155 in the placebo group (1.19%), indicating an overall 22% lower risk of new onset autoimmune diseases for those who took the vitamin (adjusted hazard ratio 0.78, 95% confidence interval 0.61 to 0.99, P=0.05). The preventive benefit seemed to increase over time. Among people who took vitamin D for more than two years, the risk reduction rose to 39%.
When the researchers made calculations excluding participants with preexisting autoimmune conditions, they still found a 21% relative risk reduction associated with vitamin D (Hahn J, et al. BMJ, 2022).
Modest Benefit from Omega-3s
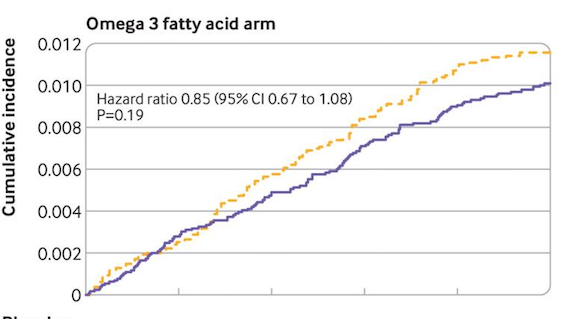
The effect of omega-3s was less robust: the data suggest a trend toward risk reduction, but it was not statistically significant. In the group assigned to omega-3s alone, there were 130 confirmed cases of new-onset autoimmune disease (1.0%) versus 148 (1.14%) in the placebo group. The numbers suggest a 15% decrease in relative risk, but the p-value of 0.19 did not reach statistical significance.
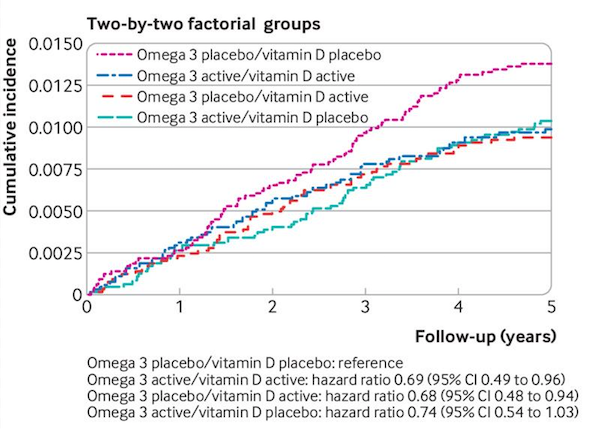
When it comes to blunting autoimmunity, vitamin D seems to do most of the heavy lifting. The sub-cohort taking both vitamin D and omega-3s did show a cumulative 31% drop in autoimmune diagnoses over the 5-year period. But this was not significantly different from the 32% drop seen in the sub-group taking vitamin D plus an omega placebo.
Since the absolute number of people who developed new autoimmune conditions was small (N=278), the investigators were not able to draw firm conclusions about the impact of supplementation on specific diseases.
They did observe an aggregate 40% drop in incidence of rheumatoid arthritis in subjects taking vitamin D, omega-3s, or both, compared with those taking placebos. But there were only 39 total confirmed new cases of RA, so it is important not to overstate the meaning of this finding.
“In preplanned secondary analyses of individual autoimmune diseases, for both vitamin D and omega-3 supplementation, hazard ratios were less than 1 (favoring supplementation) for almost all diseases; however, none of the differences was statistically significant for the individual disorders.”
Psoriasis and autoimmune thyroid disease were the exceptions to the general trend. Neither vitamin D nor omega-3s appeard to reduce the incidence of these two conditions.
BMI Affects Outcomes
Which patients benefitted most from supplementation with vitamin D and/or omega-3s?
Omega-3s had the most preventive impact in people with strong family histories of autoimmune conditions.
For vitamin D, BMI appeared to be a decisive factor, and the relationship was inverse: the vitamin had its biggest effect in people with lowest BMI, and the least effect in those with high BMI.
“When we modeled body mass index as a continuous linear term….for vitamin D treatment versus placebo, the hazard ratio was 0.47 for those with a BMI of 18, 0.69 for those with a BMI of 25, and 0.90 for those with a BMI of 30.”
This inverse relationship is consistent with a 2020 diabetes prevention metanalysis showing that vitamin D supplementation reduces the risk of type 2 diabetes but only in non-obese individuals (Zhang Y, et al. Diabetes Care. 2020). The reasons for this apparent difference in response based on BMI are not yet clear, but it does not appear to be strictly related to the fact that vitamin D sequesters in fat cells.
No other personal variables showed statistically significant relationships with the impact of supplementation.
Strong Adherence
The authors acknowledge that the vitamin D dosage in the VITAL study is two to three times the recommended Daily Values established by the Institute of Medicine: 600 IU for people up to 69 years old and 800 IU for those age 70 and up. But supplementation with 2,000 IU daily is in line with what holistic and functional medicine practitioners routinely recommend.
Hahn, Costenbader, and colleagues did not report any adverse event data but they point out that adherence to the trial regimen, defined as the percentage of participants who took at least two thirds of the given trial capsules, averaged 81%.
Blood samples at one year showed a mean increase in 25-OHD of 40% (from 29.8 ng/ml at baseline to 41.8 ng/ml at one year) in a subset of vitamin D patients, but minimal change in those on placebo, The mean omega-3 index increased by 54.7% in the omega-3 cohort, but changed by less than 2% in the placebo group.
The data showed an aggregate 40% drop in incidence of rheumatoid arthritis in subjects taking vitamin D, omega-3s, or both, compared with those taking placebos.
VITAL is not the first study to look at the potential of vitamin D or omega-3s to reduce autoimmune disease. But it is by far the largest and most definitive to date, giving the new findings considerable weight.
Prior observational studies of vitamin D have given conflicting results in terms of preventive impact (Altieri B et al, Rev Endocr Metab Disord, 2017. Murdaca G, et al. Autoimmun Rev. 2019). Small treatment trials of vitamin D in people with established autoimmune conditions have been disappointing (Giustina A, et al. Rev Endocr Metab Disord. 2020).
There are a number of randomized controlled trials suggesting that omega-3s have therapeutic benefits for people with rheumatoid arthritis, systemic lupus erythematosus, and psoriasis (Akbar U, et al. J Clin Rheumatol. 2017). But there are no intervention trials showing that omega-3 supplements can prevent autoimmune disease.
Danish researchers showed a 49% reduction in rheumatoid arthritis risk for each 30 g increase in daily fatty fish intake (Pedersen M, et al. J Rheumatol. 2005). But it is not possible to draw conclusions about supplementation from data about fish consumption.
Major Clinical Significance
The VITAL authors hold that their autoimmune findings have clinical as well as statistical significance, especially given the limitations of conventional pharmaceutical treatments for most, if not all of the major autoimmune diseases.
“The clinical importance of these findings is high because these are well tolerated, non-toxic supplements, and other effective treatments to reduce the incidence of autoimmune diseases are lacking. Additionally, we saw consistent results across autoimmune diseases and increasing effects with time.”
The study’s large and diverse sample size, its clearly defined endpoints, and high adherence rate all give the evidence notable strength. But it does have an important limitation: because participants were all over age 50, the observations of benefit may not be wholly applicable to autoimmune diseases that tend to arise in younger people.
The VITAL team is continuing to follow many of the patients as part of an extension study looking at the longer term process of autoimmune disease development, and its possible prevention. Future reports will likely shed more light on the potential role for vitamin D and omega-3s in the prevention of autoimmune conditions.
END







