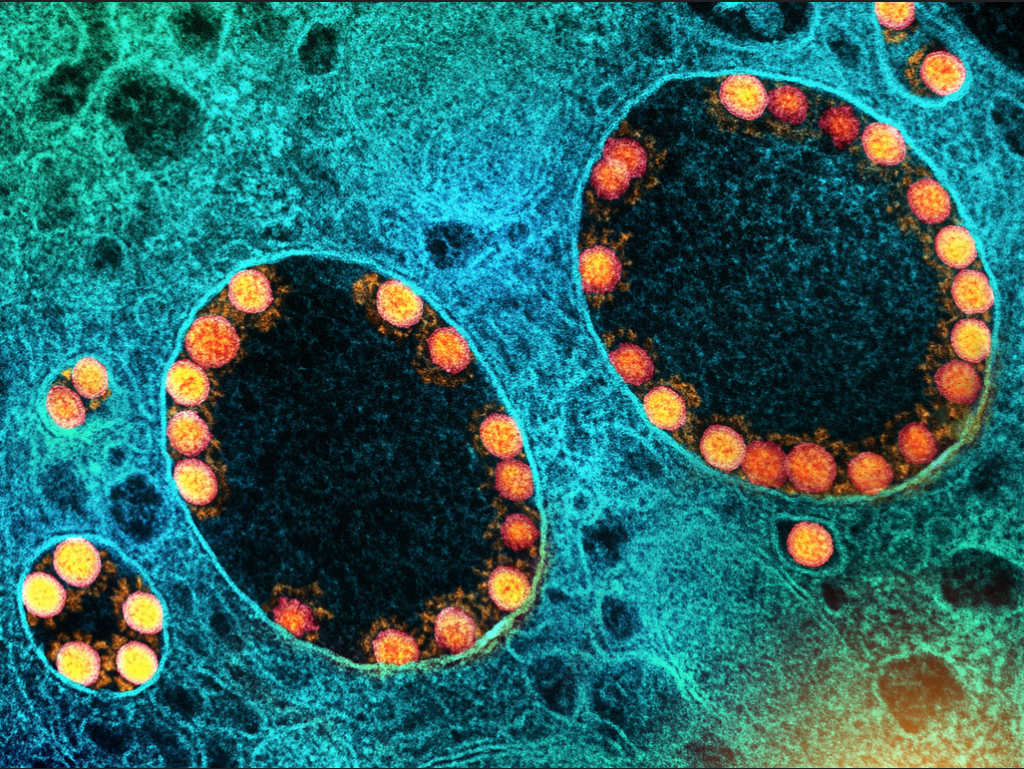
We are nearly two years into the COVID-19 pandemic. Now, more than ever, it’s worth looking into what goes on in the body and how the immune system works in critical situations like COVID-19.
The pandemic has certainly put the functioning of the immune system to test, but it has also brought to light the intricate pathways involved in protecting ourselves from viral pathogens.
Various organs and cell types—the spleen, lymph nodes, immune cells—play a role in protecting the body against pathogens and toxins, an in repairing damaged tissue. In the context of a viral infection like COVID, the key players are the white blood cells. They travel throughout the body, searching for microbes and foreign particles.
The T Cell Response
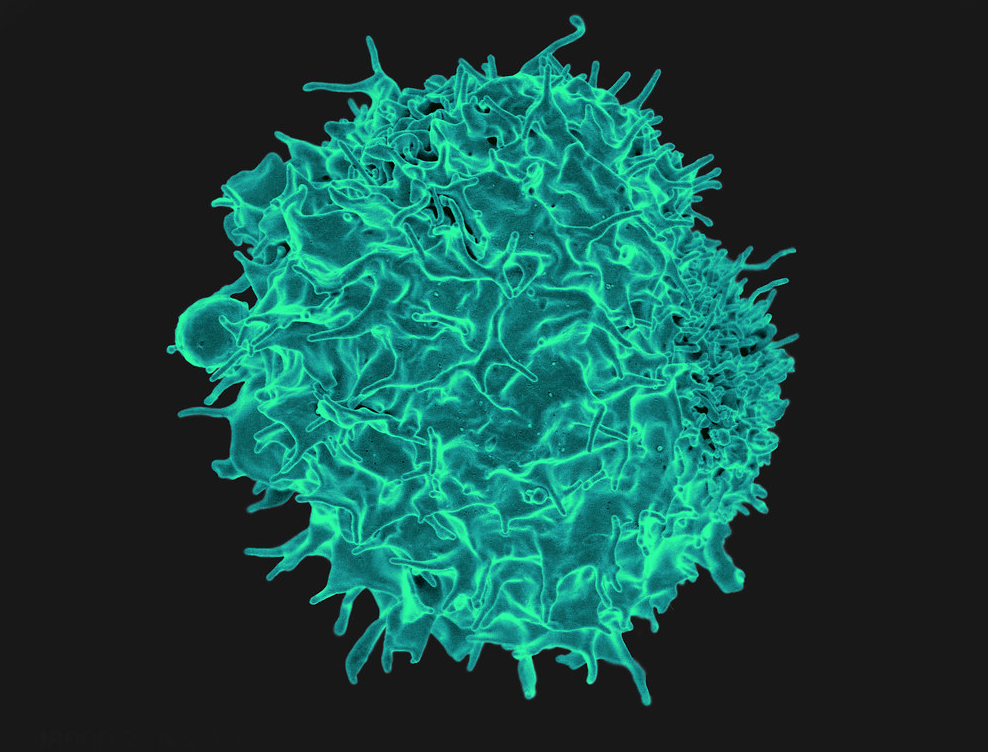
T and B lymphocytes are the major cellular components of the adaptive immune response.
T cellsare made predominantly in the thymus gland (hence the “T”) and are involved in cell-mediated immunity. T cells, including the CD4 helper and CD8 helper cells, are responsible for memory-based natural immunity.
A healthy T cell response in response to a pathogen like SARS COV2 (a positive T cell test can confirm this) should lead to a natural, protective, and relatively long-lasting immunity.
Over 160 million people worldwide have now recovered from COVID-19. Many of them have a strong protective immunity, which can shield them from repeat infection, disease, hospitalization, and even death.
Back in May, the World Health Organization released a report stating that within four weeks of infection, 90% to 99% of people who recover from COVID-19 develop detectable neutralizing antibodies, and that this protective response remains strong for at least 8 months after infection.
The problem, of course, is that many people do not survive the initial infection. The current estimate is that 4.8 million people worldwide, and nearly 725,000 in the US, have died from COVID-19.
But that does not mean we should ignore the role of natural immunity. As healthcare professionals, we should do all that we can to support our patients’ innate and adaptive immune systems, so they can respond maximally when faced with the virus.
Delta Variant: Outpacing Immune Cells
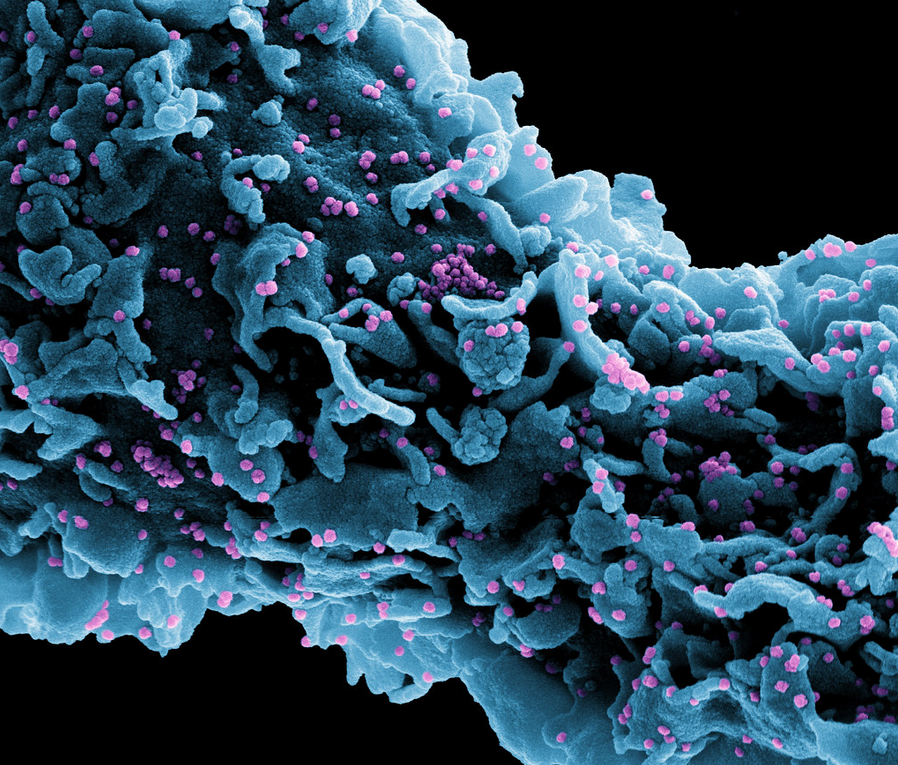
Many people are concerned about the risk posed by the new variants, especially the Delta variant. The big problem with Delta is that it can replicate 2-3 days faster than B and T cells can. In essence, it can outpace the key immune cells, making it much harder for these cells to stop the virus and prevent symptoms or interpersonal transmission. The Delta variant also puts a greater burden on the neutralizing antibodies.
The cautious good news is that while this new variant appears to spread faster, it may not necessarily be more aggressive.
Viruses are promiscuous by nature; they constantly mutate and evolve. It will not be surprising if we see additional variants emerge in the future. This is all the more reason to focus on bolstering immune system capacity.
Natural vs Induced Immunity
The protection conferred by natural immunity is equivalent to, or perhaps better than, that of vaccine-induced immunity. But the two are not mutually exclusive. Both vaccine-induced immunity and naturally-occurring post-COVID immunity will play a role in stemming the spread of COVID and reducing its morbidity and mortality.
As Klausner and Kojima state in their well-reasoned Op-Ed on MedPageToday, “Numerous scientists have found that there is a decreased risk of re-infection and extremely low rates of hospitalization and death due to repeat infection” in unvaccinated people who developed natural immunity following COVID infection.
Some people assume that documentation of a prior SARS-CoV-2 infection is synonymous with natural immunity, but really, immune status is best determined by an accurate and reliable antibody test. While antibody titers can decrease over time, T cell protective immunity–as detected by a T cell test—potentially confers lifelong protection, a phenomenon acknowledged by NIH Director, Francis Collins back in July 2020.
The COVID-19 vaccines induce neutralizing antibodies that circulate in the body, recognize, and bind to the virus, preventing it from entering cells and replicating. This is important, because once the virus enters cells, it is no longer accessible to the antibodies circulating outside the cells, and it’s free to replicate and cause damage.
An individual’s response to the vaccine can be robust or weak, or anywhere in between.
Though the scientific consensus and the public health community are almost unanimously supportive of vaccination, the reality is that many people remain resistant to getting the shots. Chastisement is unlikely to change their positions on the issue.
Bolstering Protective Mechanisms
It isvital that we do all we can to help patients nurture their intrinsic protection mechanisms, regardless of whether or not they are vaccinated.
Healthy people have a well-integrated array of robust protective mechanisms, from strong and intact skin and mucosal surfaces, to balanced Th1 and Th2 immune responses.
But too many people are in survival mode. They’re not thriving, and they’re not able to effectively protect themselves. They have co-morbidities affecting their lungs, heart, nervous system, blood vessels and other organs. They lack the essential nutrients needed for the body to function well.
Co-morbidities often indicate overexposure to “anti-nutrients”—chemical compounds that reduce the body’s ability to absorb and assimilate essential nutrients—and other stressors that deplete the body’s nutrient stores and its metabolic capacities.
Let’s face it: the immune system protects those who are able to protect themselves. People can minimize their risk of serious illness from SARS-CoV-2 or any virus by ensuring they’re getting enough essential nutrients, healthy activity, and sleep.
We recommend that people following the Alkaline Way program to fully support and nourish the immune system. This includes:
- Using buffered l-ascorbate. Acute depletion of antioxidants, especially ascorbate, is a hallmark of COVID-19 infection.
- Taking vitamin D3 regularly– especially liquid drops that are assimilated and absorbed easily. This essential neurohormone helps regulate cell division and is important in many systems, especially when combined with vitamin K2. Maintaining a Vitamin D3 level of 50-80 ng/ml is a good goal. Though there are not yet any large intervention trials proving that vitamin D3 is protective against SARS-CoV-2, deficiency is a well-documented epidemiologic risk factor for infection, severe illness, and death.
- Zinc and Magnesium: From taste and smell to immune and neurohormone balance, zinc and magnesium are essential, yet often deficient nutrients. People at high risk show signs of metabolic acidosis. Urine pH after rest is a good indicator of whether or not someone has enough buffering minerals present to neutralize the day’s excess acids from metabolism.
- Flavonoids like quercetin dihydrate, which function as zinc ionophores. Flavonoids are nature’s way to facilitate necessary cellular uptake of zinc and other helpful minerals.
Read our complete virus reduction protocol here .

Lack of essential nutrients to rebuild damaged tissue, increased exposure to anti-nutrients, lack of deep abdominal breathing, inadequate stretching/walking, and poor sleep are also predisposing factors for myriad illnesses.
At its core, sustained health is determined by what people EAT, DRINK, THINK and DO. Let’s all consider COVID-19 a wake-up call to invest in personal and social health.
Now is the time for people to invest in self-care, personal care and cultivation of healthier habits. Small steps often bring big rewards. Multiple small steps multiply the benefits.
END







