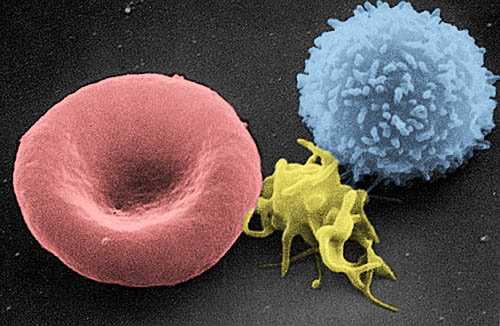
Platelets may be tiny—on average they’re about 20% of the diameter of red blood cells—but they have huge impact on our health and wellbeing. Beyond their obvious role in blood clotting and wound healing, they are also important players in the immune system.
More than we realize, optimal health depends on the platelets doing their jobs appropriately, but not over-doing them.
There are as many as 150,000-350,000 platelets per microliter of blood, but since platelets are so small, they make up just a tiny fraction of the blood volume.
These splendid multi-functional cell fragments are produced by the megakaryocytes in the bone marrow, via a process comprised of an intricate series of remodeling events. A single megakaryocyte can release of thousands of platelets. Like red blood cells, platelets (aka thrombocytes) lack nucleii, and hence they have no nuclear DNA; but they do contain some RNA machinery.
The “Goldilocks” Zone
As with most physiological functions, we want thrombocyte production and function to in the “Goldilocks” zone: not too much and not too little.
Blood clotting is indeed essential. If it weren’t for high-functioning platelets, even relatively minor injuries would be debilitating or life-threatening.
But as we see all too often in our practices, clotting in the wrong places at the wrong times—in the coronary arteries, the carotids, or the brain—can be deadly. Clots are not always stable and they don’t always stay put. A clot formed in a leg vein can travel through the bloodstream to the lungs, causing an embolism. A thrombus arising in the heart can end up in the brain. These silent migrations can have lethal consequences.
In the context of atherosclerosis, we can really see how a physiological healing response can end up causing damage. When there’s an endothelial injury, white blood cells and particles of cholesterol-carrying low-density lipoprotein (LDL), and form a gooey pool rich in inflammatory signaling molecules.
Eventually, a thin cap forms over the mess. If that cap splits open, the body responds as it would to a cut in the skin: platelets rush to the scene and clotting begins. If the break is small and heals quickly, the episode passes with no harm. But if the rupture is extensive, the resulting clot occludes the artery. If that happens in one or more of the coronary arteries, the patient ends up in the emergency room with a myocardial infarction. When a clot occludes an artery feeding the brain, it causes a stroke.
We’re taught to prescribe anticoagulant drugs to decrease platelet aggregation, and to interrupt the clotting cascade at one or several of its stages. These can mitigate risk of MI and stroke, but it is equally true that any one of these anticlotting drugs can cause excessive bleeding. We need to be careful and constantly watch for signs of abnormal bleeding, such as bruising and swelling (without physical injury), or blood in the stool.
We also need to consider that thrombocytes play other important roles beyond clotting. These include:
Tissue & Wound Repair: Adequate and timely repair depends upon healthy, functioning platelets. Different growth factors and other biomolecules necessary for wound healing are provided by platelets (hence the surging interest in platelet-rich plasma (PRP) to treat sports injuries and the like). When there is a deficit in repair, inflammation results. In some cases, this is due to platelet inhibition. It may also be due to deficiencies in magnesium or vitamin C, or to use NSAIDs, steroids, aspirin or other drugs that inhibit platelets.
Cell Proliferation: Platelets release specific signals that promote mitosis in various tissues of the body. This property of platelets has been harnessed to create therapies for healing from bone-related injuries
Immune System Function: Platelets are crucial to the optimum functioning of the immune system, modulating both the innate and adaptive immune defense/repair responses.
- Innate – Thrombocytes regulate the maturation and activation of macrophages, neutrophils, and dendritic cells. They also act as first responders when a virus, bacteria or allergen enters the body.
- Adaptive- They also modulate the adaptive immune system by aiding in CD4 maturation. These are helper lymphocytes that amplify immune system reactions to pathogens. CD4 cell activation is required for proper T- and B-cell mediated immunity.
Physiology Before Pharmacology
How can we help our patients optimize their platelet function? I tend to advocate for a “physiology before pharmacology” approach. The key is to protect the endothelial lining, and to promote appropriate but not excessive clot formation. Here are five key factors that support healthy platelet function:
- Ascorbate (Vitamin C): Vitamin C is an antioxidant and antihistamine that mitigates radical oxidative damage. It also down-regulates platelet aggregation by increasing anti-aggregatory nitric oxide (NO) from polymorphonuclear leukocytes (Raghavan SAV, et al. Thrombosis Research 2003). I recommend using buffered l-ascorbate based on the C cleanse protocol to maximize this benefit.
- Polyphenols: Plant-derived polyphenols like quercetin dihydrate and oligomeric proanthocyanidins (OPC) are synergistic antioxidants that promote tissue repair, especially in conjunction with buffered l-ascorbate. They also act as zinc ionophores, meaning that they transport zinc where needed. This is an added plus, because zinc is important for endothelial cell integrity.
- Magnesium: Adequate magnesium intake can prevent thrombocytopenia while also reducing unnecessary platelet aggregation. Magnesium also raises ATP production in the mitochondria. It protects essential fats during transport, activates enzyme catalysts, decreases metabolic acidosis, and protects the kidneys. I suggest using magnesium with choline citrate for optimum absorption. Checking the 1st morning urine pH is a great way to know if you are getting adequate magnesium.
- Vitamins D3 and K2: Vitamin D deficiency can increase platelet aggregation and consequently, raise the risk for cardiovascular disease. Vitamin D3 also regulates platelet volume. I suggest taking enough Vitamin D3 to maintain blood levels of between 50-80 ng/ml. Using Vitamin K2 with Vitamin D3 is recommended.
- Omega 3 Fatty Acids: Omega-3s, especially EPA and DHAhave a positive influence on platelets, in that they reduce unwanted platelet aggregation. For best results, use pure, active EPA/DHA distilled under nitrogen and micellized in softgels. The Omega-3 Index is a simple test that gives a clear picture of someone’s Omega-3 status.
END







