As we head into the peak months for the flu, we as health care providers need to be especially vigilant about the integrity of our patients’ immune systems. Paired with COVID-19, this year’s flu season carries the serious risk of compromising their future immune response.
A key step in preventing these complications lies in helping our patients understand the strengths and weaknesses of their immune systems. Being more aware of their individual vulnerabilities will equip them with an additional line of defense during the dangerous winter months.
With advanced tools like immunophenotyping, we will be better able to advise patients about ways to protect themselves against the threat of serious illness.
Because widespread social distancing and mask measures brought about an historic decrease in influenza transmission last year, population immunity is also likely to be lower than it has been.
A Brutal Flu Season
This year’s flu season is anticipated to be particularly severe, and with COVID-19 still spreading in communities across the country, the stage is set for an impending “twindemic.”
Because widespread social distancing and mask measures brought about an historic decrease in influenza transmission last year, population immunity is also likely to be lower than it has been, according to the Centers for Disease Control and Prevention (CDC) and National Foundation for Infectious Diseases (NFID). As such, everyone is at increased risk of contracting the flu during the 2021-22 season.
Even in milder years, the flu has a significant impact on hospitalization and mortality rates. According to the CDC’s estimates based on preliminary data from the 2019-20 season ending just prior to broad adoption of COVID-19 precautions, there were approximately 35 million people with symptomatic illness, 380,000 hospitalizations and 20,000 flu-related deaths in the US.
With the flu and COVID-19 both circulating and potentially peaking simultaneously in early winter, a large population of the country is under high risk of co-infection. This can not only aggravate the symptoms and complications of disease, but also create treatment conflicts for individuals who are hospitalized.
For example, corticosteroids, administered to prevent or mitigate severe COVID-19-related inflammatory responses, are associated with poor outcomes and increased mortality in severe influenza patients.
Assessing the Immune System
With both viruses triggering immune responses that affect vital organs, including the lungs, brain, heart, and muscle, we are concerned about the long-term risks that co-infection brings to the immune system.
We know that people with weakened immune systems due to preexisting disease or exposure to certain medications are at a higher risk for complications from both the flu and COVID-19.
Recent research has also shown the ability of SARS-CoV-2 to hyperstimulate the immune system and trigger flares of pre-existing autoimmune reactions, even among those who previously showed no overt symptoms of autoimmune disease. Many of our patients could unknowingly be immunocompromised and at risk of severe illness in the event of co-infection this flu season.
With the flu and COVID-19 both circulating and potentially peaking simultaneously in early winter, a large population of the country is under high risk of co-infection.
A complete blood count (CBC) done as part of routine blood work, is frequently the initial diagnostic tool for identifying immunological disorders. But it is only a small part of a complex map that helps our patients understand their immune systems and potential weaknesses.
CBCs alone are insufficient and incomplete for helping us determine how vulnerable our patients are to opportunistic viruses. Looking at a patient with an inflammatory disorder, for example, white blood cell (WBC) and total lymphocyte counts could both come back as “normal” on a routine CBC, indicating nothing out of the ordinary, despite the fact that the patient is actually suffering from dysregulation of the immune system.
In fact, most immunologists agree that even in patients who have been diagnosed with immune-mediated conditions like allergies, rheumatoid arthritis, and neuropathies, the CBC is normal about 70 percent of the time.
Immunophenotyping for Flu Protection
Being able to detect early immunological warning signs and risk goes a long way in helping patients understand the functions and responses of their immune systems. We can offer this support by looking at immunophenotype patterns, or immune system “fingerprints,” which paint a much clearer picture of immunological makeup.
Immunophenotyping provides critical information about immune cells and how well they work together. The techniques are based largely on flow cytometry, which isolates and quantifies different types of cells based on antigens and markers present on the cell surface. Advanced flow cytometry can precisely measure the properties of living cells such as size, shape, density, and granularity, with a high degree of precision.
Lymphocytes represent 20% to 40% of a patient’s total WBCs. By quantifying these subpopulations and the ratios between them, we are better able to predict how an individual might react to environmental antigens like influenza viruses.
Immunophenotyping by flow cytometry is useful in the identification and quantification of lymphocyte subsets. This is especially valuable when working with patients whose CBCs are normal. Immunologists have found that about half of those with normal CBC values will show immune abnormalities when flow cytometry is used to quantify T-cell, B-cell, NK cell, CD4, and CD8 lymphocyte populations.
Flow cytometry is widely used in cancer research. The accuracy and detail provided by these tests have demonstrated significant value well beyond oncology.
Lymphocytes represent 20% to 40% of a patient’s total WBCs. By quantifying these subpopulations and the ratios between them, we are better able to predict how an individual might react to environmental antigens like influenza viruses.
Comprehensive Immunophenotyping
Knowledge gained through immunophenotype patterns is essential for physicians wishing to offer better immune system support, including helping immunocompromised patients make informed decisions during critical periods like flu season.
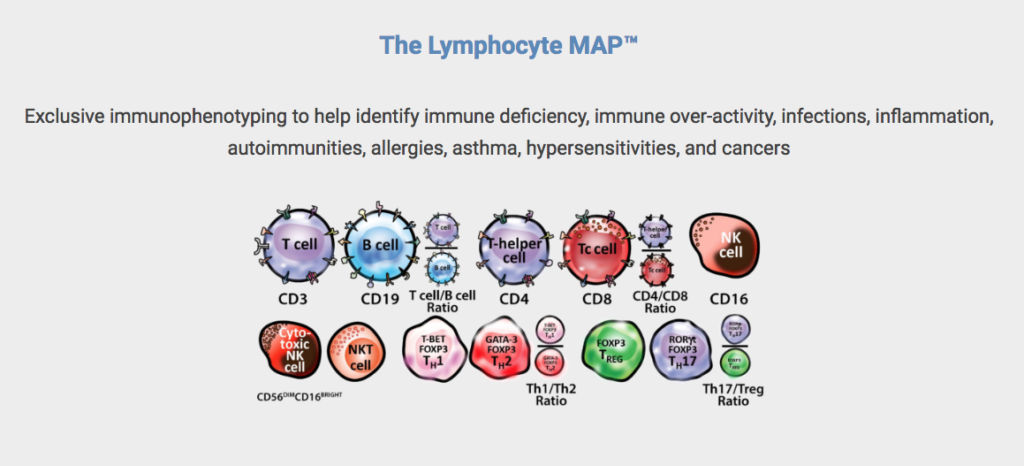
Cyrex Laboratories, a clinical laboratory specializing in functional immunology and autoimmunity, has recently developed a proprietary test panel called The Lymphocyte Map – Comprehensive Immunophenotyping of Lymphocytes. This tool provides a much more comprehensive evaluation of the immune system than a CBC, providing greater clinical insight about a patient’s immune susceptibility.
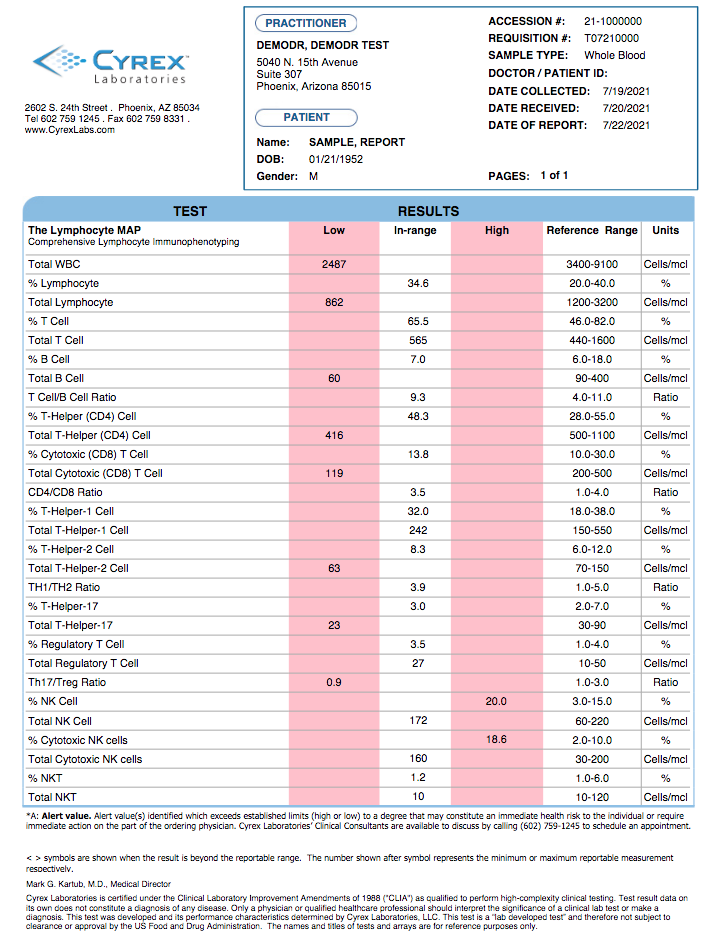
By measuring the integrity of the immune system at the cellular level, based on 29 key biomarkers, The Lymphocyte Map allows providers to classify a patient’s immunophenotype patterns into 13 different immunotypes. This can reveal hidden patterns and trends regarding immune system weaknesses, imbalances, and overall fitness.
Practitioners can also use immunophenotypes to design treatment plans to reduce or prevent the progression of disorders and mitigate the influence of exogenous pathogens.
Now, more than ever, this remains a critical component of patient care in the face of this season’s looming twindemic.
Chad Larson, NMD, DC, CCN, CSCS, holds a Doctor of Naturopathic Medicine degree from Southwest College of Naturopathic Medicine and a Doctor of Chiropractic degree from Southern California University of Health Sciences. He is a Certified Clinical Nutritionist and a Certified Strength and Conditioning Specialist with particular interest in advanced developments in the fields of endocrinology, orthopedics, sports medicine, and environmentally-induced chronic disease. Dr. Larson is an Advisor and Consultant on the Clinical Consulting Team for Cyrex Laboratories.
Mark Engelman, MD, is the Director of Clinical Consulting for Cyrex Laboratories. He is also the Founder and President of the Engelman Health Institute. His career history includes 23 years as the director of St. Joseph’s Medical Center emergency department; and a term as President of the Maricopa County American Heart Association. He is also the Founder and CEO of AmeriMed American Hospitals in Mexico; and is known as an expert speaker on emergency medicine both nationally and internationally.







