
Exposure to polluted air is associated with increased depression symptoms in people with bipolar disorder (BPD), according to a new study by psychiatrist Joseph Hayes, MD, PhD, and Aaron Kandola, at the University College London.
In the first project of its kind, Hayes and Kandola tracked symptoms of depression and mania against real time changes in Air Quality Index (AQI) in a cohort of 1,423 women and men previously diagnosed with BPD.
To do so, they made use of a new self-tracking app called Juli, which—among other things—provides users with daily AQI reports based on their smartphone geolocations.

Many previous studies have suggested links between pollution—especially chronic exposure to particulate matter with the diameter of ≤2.5 μm (PM2.5)–and worsening of unipolar depression. A systematic review by University of Milan researchers looking at 39 small studies, found a small but significant increase in relative risk of depression among people with the highest exposures to PM2.5 (Borroni E, et al. Environ Pollut. 2022).
Kandola and Hayes are the first to document this association on an individual level in a BPD population, and the observed relationship was more pronounced. “As air quality worsened, symptoms of depression increased,” they write (Kandola A, Hayes J. BJPsych Open. 2023).
AQI & PHQ Scores
The AQI is a standardized indicator that integrates daily measurements of particulate pollutants ranging in size from ≤2.5 μm (PM2.5) to ≤10 μm (PM10), along with nitrogen dioxide, sulphur dioxide, ozone, and carbon monoxide. Data are drawn from thousands of sensor sites all over the world, with local AQI readings computed hourly and daily.
The AQI scale goes from 0 to 500, with higher values reflecting worse pollution. In general terms, AQI values below 100 are considered satisfactory, and values above 100 are considered “unhealthy.” Scores over 400 are deemed hazardous.
Hayes and Kandola used the Patient Health Questionnaire-8 (PHQ-8)—an 8-item survey—to assess depression symptom burden over two-week intervals.
They used the Altman Self-Rating Mania Scale (ASRM), a 5-question rating tool, to measure symptoms of mania. Both scales are well-validated and widely used both clinically and in research.
Users of the Juli platform completed these self-assessment scales every two weeks.
For each study participant, the researchers were able to plot depression and mania scores against daily local AQI readings reported during the two-week period prior to the assessment.
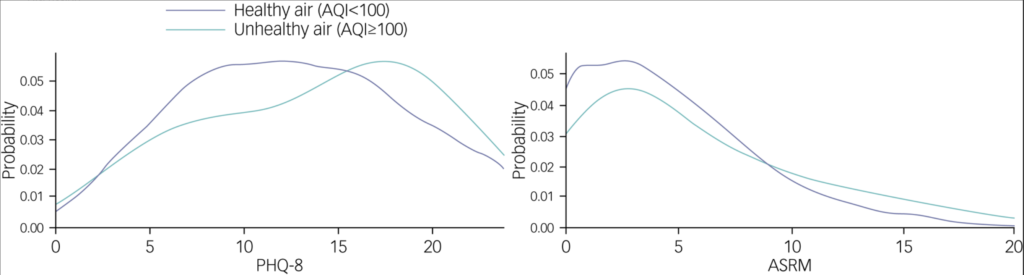
“After adjusting for age, gender, mean step count, temperature and humidity, we found an association between AQI and PHQ-8 score, such that total PHQ-8 score increased by 0.011 points for every one-point increase in AQI,” they write.
A Growing Concern
Essentially, that means a 100-point increase in AQI potentially translates into a 1-point increase in depression symptom scores. This summer many regions of the US have experienced sudden AQI surges of several hundred points as a result of the massive Canadian wildfires.
In New York City, for example, AQI soared from its typical summer range of 75 to 100, up to 407 in the first week of June, as a result of atmospheric changes that drove smoke from Quebec and Nova Scotia southward across the eastern seaboard.
In California and other western states, smog caused by fires is an all-too-common occurrence.
Degradation of air quality is a worldwide phenomenon.

“Where I live in London the air quality index is probably 100 most of the time, but there’ll be times when it goes a lot higher and so in those times you start to have a noticeable effect on individuals with bipolar disorder,” Dr. Hayes said in an interview with Fierce Healthcare.
Notably, in their study the University College London researchers found no association between AQI and ASRM scores, suggesting that pollution exposure preferentially exacerbates symptoms of depression but not mania in people with BPD.
Hayes is the Chief Medical Officer and co-founder of the Juli app and data platform.
Neuroinflammation
If the notion that air pollution directly affects human psychology strikes you as far-fetched, consider that many pollutants—including fine particulate matter—have been linked to neuroinflammation, neurotoxicity, and hormone dysregulation (Braithwaite I, et al. Environ Health Persp. 2019).

Kandola and Hayes point out that even brief exposures to high levels of PM10 are associated with elevations of inflammatory cytokines such as interleukins 1-beta (IL-1β) and 6 (IL-6), and tumor necrosis factor alpha (TNF-α) in people with depression.
“There’s also probably particular subtypes of bipolar disorder that we haven’t really identified yet, as there are with depression, that are more inflammatory in nature, and it might be that pollution has a particular impact on those individuals,” Hayes surmised in his interview with Fierce.
A Long, Troubling List
Depression is one more condition on a long and troubling list of disorders that are associated with poor air quality. Asthma, allergic rhinitis, and other respiratory conditions are obvious examples. Exposure to fine particulate matter has also been linked to increased mortality from ischemic heart disease and stroke. A large metanalysis of 56 studies found strong indication of a correlation between short- and long-term exposure to PM2.5 and increased risk of hypertension, stroke, and myocardial infarction.
Exposure to PM2.5 and carbon monoxide also raises the risk of stillbirth and spontaneous abortion, according to a 2018 systematic review of 35 human and 8 animal studies.
“Air pollution may be an important modifiable risk factor for symptom severity in various mental health problems, including bipolar disorder,” Hayes and Kandola conclude.
On one hand, that’s a hopeful discovery. On the other, it is troubling given the number of places worldwide that routinely have AQI readings far beyond the “safe” threshold of 100, and the increasing incidence of massive fires that can trigger rapid and precipitous rises in pollution levels.
END







