Ask anyone—patient or practitioner—to describe hospital food, and you’ll invariably get words like awful, horrible, or disgusting.
Hospital food is typically composed of highly-processed and refined ingredients, often laden with artificial sweeteners and preservatives. Vegetable portions are generally small, overcooked, and bad tasting. The meals may meet USDA nutritional guidelines for limiting sodium and trans fats, but few would consider them truly healthy.
That’s because for decades, hospital systems have viewed food as a line item, not as an intrinsic aspect of healing.
“Food situated in the hospital is not valued as a component of care. It’s overhead,” says Stacia Clinton, RD, program director of Healthy Food in Health Care, through the global coalition, Health Care Without Harm.
Clinton and others hope to change that mentality. Her organization is part of a growing movement to establish healthier hospital food systems. They hope to shift the mindset within hospitals toward one that truly recognizes food as medicine.
Farm to Bedside
The good news is that hospitals across the country are starting to wake up to the simple fact that healthier food nurtures healthier patients, and in the long run, healthier bottom lines. While there’s still much institutional inertia, many medical centers are taking meaningful steps to improve the meals they provide for patients.
“The root cause of chronic disease is poor nutrition,” says Thi Squire, Community Garden Project Manager for Grow2Heal, a South Florida organization that literally brings garden-fresh vegetables to the bedside by helping hospitals grow their own.
 Grow2Heal works with Homestead Hospital, part of the Baptist Health South Florida network, to grow produce right on hospital grounds. Last season, Grow2Heal harvested 3,000 pounds of fresh fruits and vegetables that fed patients, staff, and local community.
Grow2Heal works with Homestead Hospital, part of the Baptist Health South Florida network, to grow produce right on hospital grounds. Last season, Grow2Heal harvested 3,000 pounds of fresh fruits and vegetables that fed patients, staff, and local community.
Not all facilities have the resources or space to grow fresh food like Homestead. But that’s certainly not the only option. Some hospitals are joining with nonprofits like Partnership for a Healthier America, a group funded by the food and beverage industry and foundations, that offers its own healthy food service initiative.
According to Clinton, over one-third of US hospitals have already taken steps to improve the quality and healthfulness of their food services: serving less meat; providing daily vegan options; using more local produce; prescribing fresh fruits and vegetables for patients after discharge; and increasing nutrition education for patients, families, and communities.
State Mandates
With Burger King now serving plant-based Impossible Burger patties, and Ben and Jerry’s scooping up vegan ice cream, it is no wonder the Economist calls 2019 the Year of the Vegan . Hospitals are catch on.
In California, they must. California SB 1138 mandates health care institutions provide patients with vegan options.
In New York State, a similar bill just passed the state’s legislature that will guarantee all hospitalized patients a “healthful plant-based option” at every meal.
If it’s happening in California, your state may be next.
But even without legislative fiat, hospital systems all across the nation are making the plant-based shift.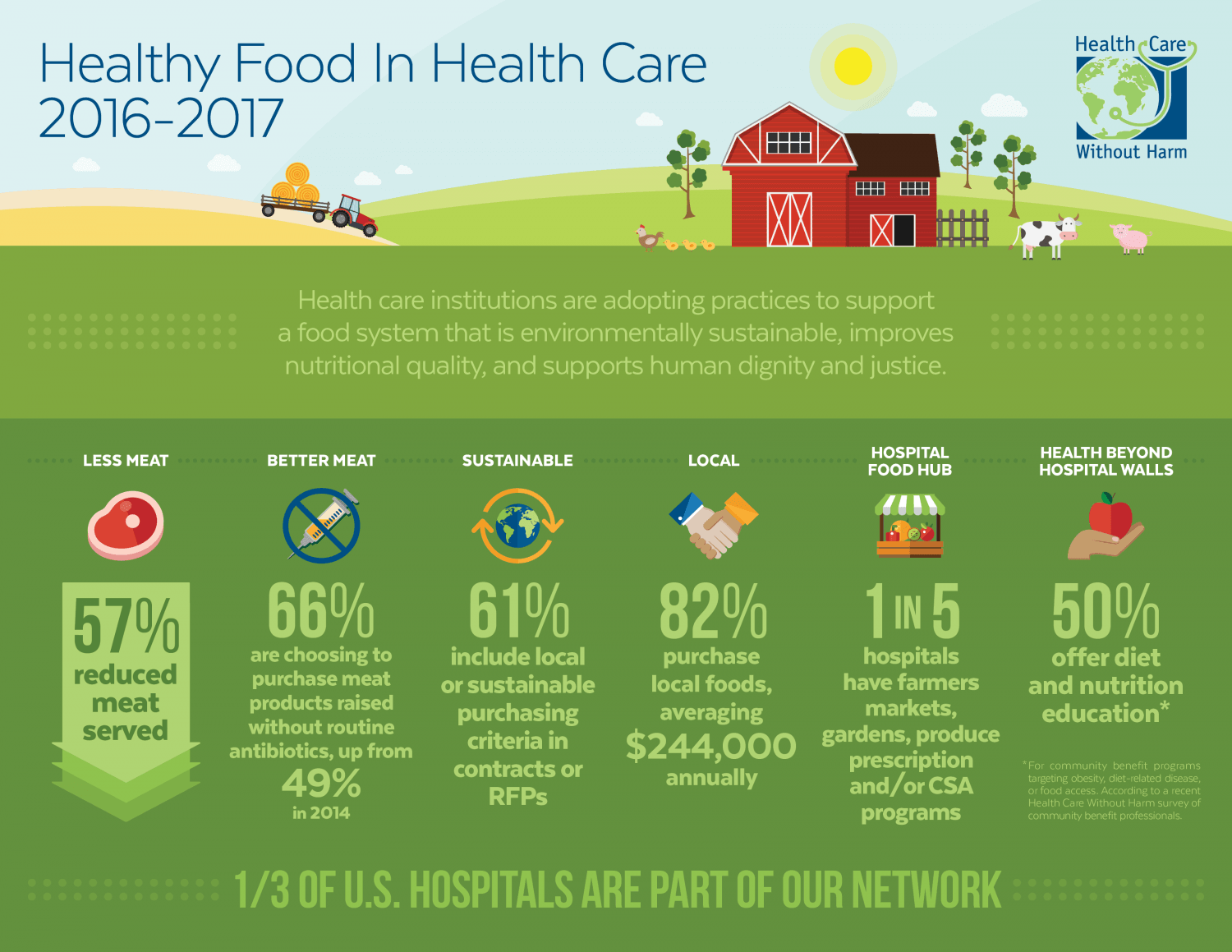
“We Saw the Need Early On”
Hospitals in the state of Maine are making great strides in that direction.
“Many health systems are coming on board, but MaineHealth was unique,” says Emily Kain, Prevention & Wellness program manager at MaineHealth’s Center for Health Improvement. “We saw the need early on.”
MaineHealth—a non-profit coalition of 11 community hospitals and 1,600 independent physicians’ practices– joined Partnership for a Healthier  America’s Hospital Healthier Food Initiative back in 2012. PHA provides its 700-member hospitals, including MaineHealth and health care giant Kaiser Permanente, the tools and metrics to make healthier changes. Together, they create goals for each hospital. PHA then sends external evaluators to conduct site visits to measure outcomes.
America’s Hospital Healthier Food Initiative back in 2012. PHA provides its 700-member hospitals, including MaineHealth and health care giant Kaiser Permanente, the tools and metrics to make healthier changes. Together, they create goals for each hospital. PHA then sends external evaluators to conduct site visits to measure outcomes.
“Our hospitals have made a lot of changes,” Kain says. “People would be surprised the number of healthy options you can find on a cafeteria line.”
Developing healthier menus for patients and cafeteria patrons has been relatively easy, she says. The hospital system met PHA’s goals of using produce with no added sodium or sugar within the first year. Harder, says Kain, was meeting the program’s data collection requirement.
Prior to working with PHA, MaineHealth’s food service lacked a systemwide database. “It was a huge ask of our food service team to analyze every single thing they were serving in terms of nutrient information.” It took over a year to get all its hospitals in compliance, but MaineHealth has been so successful in meeting objectives, PHA selected it as one of five finalists for Partner of the Year in 2017.
Nutrition Beyond the Bedside
According to a new Tufts University study, subsidizing fresh fruits and vegetables could save over $100 billion in health care costs and reduce 70% of chronic disease.
Federal veggie subsidies are not likely to happen any time soon. But some forward-thinking hospital administrators are realizing that many patients are chronically malnourished, and they want to do something about it.
 The New Hanover Regional Medical Center in Wilmington, NC, is experimenting with a program to extend healthy food aid beyond the walls of their facilities.
The New Hanover Regional Medical Center in Wilmington, NC, is experimenting with a program to extend healthy food aid beyond the walls of their facilities.
Up to 20% of all New Hanover inpatients are already suffering from malnourishment and food insecurity . Many eat better in the hospital, where patient meals are managed by corporate service provider Sodexo , than they do at home once discharged.
Whether the barrier to good nutrition is limited income or limited accessthe hospital has recognized that malnourishment impedes healing. It also costs over $160 billion in annual health care costs.
New Hanover responded by launching an assistance program that sends a dietitian to visit and council discharged patients. In some cases, the hospital sends patients home with food, like peanut butter, whole grain bread, and yogurt “to bridge a gap,” says Angela Lago, New Hanover Regional’s Clinical Nutrition Manager.
“We wanted to keep it simple. We don’t know what patients’ living conditions will be. Some are living in hotels, some may not have refrigerators, so we have foods that are easier to prepare, something that wouldn’t be expensive if they tried to buy it themselves.”
Funding for New Hanover Regional’s patient food assistance program came through the Duke Foundation but, says Lago, “I couldn’t do any of this without support from everyone — people who are helping me to generate data or get the grant, or the administrative executive team giving me a green light.”
She hopes to be able to add fresh produce going forward, through programming modeled on the Wholesome Rx system established by the nonprofit, WholesomeWave.
MaineHealth is already at work on this sort of program, bringing more fruits and vegetables grown by local farmers into its participating hospitals.
A Cultural Shift
“Local” and “seasonal” are more than just buzz words. Food grown this way offers patients and hospital staff fruits and vegetables with optimal freshness, flavor, and nutrient density. It also creates value within communities—especially rural communities—while reducing carbon footprints and shortening supply chains, which in turn, keeps costs comparable to frozen prepared produce.

But the transition from conventional industrial food service to more of a farm-to-bedside approach can be challenging. An already overworked kitchen crew may balk at having to chop and prep 25 pounds of fresh, local butternut squash rather than pouring out ready-to-go puree from huge containers.
“Changing the culture of the kitchen, retraining staff, is a lot of work,” admits Grow2Heal’s Squire.
All parties interviewed stress that nutrition education needs to goes beyond patient care. It needs to happen throughout an institution.
“We’ve talked about it so much, with hospital physicians and nurses, administration, marketing and analytics,” says Lago. “Everyone has an understanding of the importance of nutrition.”
“Bring the distributors and vendors into the room, too,” says Kain. “Success comes from educating them, too.” MaineHealth food service directors have been able to deter their distributors from pushing chocolate-covered granola, while steering them toward supplying lower sodium lunch meats and antibiotic-free poultry. These may not seem like monumental changes, but at a big institution, any change is a significant achievement.
Healthcare’s Purchasing Clout
If a distributor resists coming on board? “Thankfully, we have a million choices,” says Kain. “Based on our contract, we can purchase from other suppliers and distributors.”
Kain’s comment underscores an important truth: the health care sector wields significant purchasing power. Health Care Without Harm’s Greenhealth Exchange encourages hospitals to use it to their advantage.
Greenhealth Exchange serves as a buyers’ club for about a third of HCWH’s 1,200 participating hospitals. This kind of leverage has, for example, enabled Kaiser Permanente to get half of its fruits and vegetables from sustainable growers. “Through changes in purchasing, hospitals can impact the environment, social transformation and a large portion of the economy,” says Clinton.
Several organizations have stepped forward to help hospitals improve the quality and nutritive value of their food.
 Oldways, a non-profit focused on helping people adopt healthier veg-based diets, recently teamed up with plant-powered RD Sharon Palmer to launch Plant-Forward Plates, a toolkit for health care food services. Available at a negligible cost, it includes vegan recipes, scaled ordering, and HACCP protocols for hospitals of every size.
Oldways, a non-profit focused on helping people adopt healthier veg-based diets, recently teamed up with plant-powered RD Sharon Palmer to launch Plant-Forward Plates, a toolkit for health care food services. Available at a negligible cost, it includes vegan recipes, scaled ordering, and HACCP protocols for hospitals of every size.
Even food service giants, Sodexo and Aramark, have developed plant-based menus by partnering with Forward Food, a program developed by the Humane Society.
More than a rescue agency for puppies and kittens, the Humane Society is the country’s largest animal protection organization.
The group developed Forward Food in 2013 as part of its farm animal protection campaign. Forward Food gives hospital systems, schools and other institutions the resources—meatless meal plans and recipes, apps, infographics, hands-on chef training–to move their kitchens toward plant-based options. The program is nationwide, customizable, and best of all, it is free.
Healthier hospital food starts with what’s on patient plates, but that’s just the beginning. “We can have a broad impact on our community beyond wellness,” says Grow2Heal’s Thi Squire.
That’s a healthy outcome for everyone.
END







