
In recent years, a number of prominent health influencers have embraced the idea that there is a “plant paradox,” and that people should stop eating kale and other common vegetables because they’re allegedly full of toxic “anti-nutrients” such as lectins, oxalates, goitrogens, tannin, and phytates.
In promoting this view, they are overturning decades of research—as well as good common sense—which tells us that eating a diet rich in plant foods correlates with reduced risk of many common disorders.
I myself have been confronted by people who hold strongly to this anti-nutrient perspective, and who see many common vegetables as villains. In fact, as I would give talks on “eating the rainbow,” I began to get these sorts of counter-statements in increasing proportions.
At first, I couldn’t believe that anyone could refute the idea that eating a preponderance of fruits and vegetables is healthy. The evidence clearly stacks in favor of plant-rich diets when it comes to reducing the risk for chronic diseases as well as mental health and cognitive problems. But rather than categorically rejecting it, I wanted to better understand this concept of “anti-nutrients,” a term that was introduced in the scientific literature in the late 1970s.
Being in the nutrition sphere for over two decades, I was used to pendulums of opinion swinging widely, and a fair degree of absolutism among adherents of particular dietary philosophies. It seemed that this campaign against anti-nutrients was yet another example of the strange human tendency to assign hard lines of “yes or no,” “good or bad” morality to eating. In focusing on specific plant compounds like lectins and phytates, and eliminating entire food groups, it seemed a lot of people were losing the proverbial forest for the trees.
Yet, I was also wondering whether there might be some wisdom in reducing anti-nutrients, and whether I might have to rethink the rainbow and embrace a different color scheme.
One of my graduate students, Weston Petroski, and I rolled up our sleeves to write a narrative review article to see whether there truly was anything to the idea that we should fear a cup of tea filled with tannins, or avoid spinach because of its oxalates.
I kept an open mind.
In 2020, we published the paper in the journal, Nutrients. It became so popular that the journal editors approached me to write another article. Discover magazine profiled me in one of their write-ups on anti-nutrients, and from there, I was able to speak on both “eat the rainbow” and “anti-nutrients” in the same breath.
Like many topics in nutrition science, the question of anti-nutrients is complex and nuanced. Rather than applying dogmatic rules, we need to consider the inherent complexity of plants, as well as the wide individual variances in how people eat and how they respond to different foods.
In this article, I’d like to discuss a few of the most cited anti-nutrient categories, to give you the high-level view, followed by my summary of the takeaways from our investigation of this subject.
What Are Anti-nutrients?
In the classical sense, anti-nutrients are referred to as plant compounds that interfere with the absorption or metabolism of vitamins and minerals. However, some people have broadened the definition, and now use the term colloquially to also include problematic plant compounds such as lectins, that may increase inflammation and gut permeability, or cause problems via other mechanisms.
Lectins
Lectins comprise a large class of proteins within humans, animals, fungi, algae, plants, and viruses, that bind to carbohydrates and, in some instances, cause agglutination of cells. According to some estimates, about 30% of all human foods contain lectins, which may be problematic if they are resistant to digestion.
Some of the first publications on “lectins” listed in Pubmed date back to 1946. By the late 1980s, the field of “glycobiology” began to emerge as researchers shed light on the ways in which sugars become linked with other types of molecules to form glycoconjugates. In the present day, many researchers have focused on the ways in which lectins bind carbohydrates, and the potential negative effects this might have on human health. Several authors in the health and nutrition field have popularized this concept through books, videos, and fad diets.
Much of the data linking lectins to human health risks have come from cell culture and animal studies. The associations between lectin intake and human disease risk have not been definitively proven by human studies.
Lectins in plants have been brought into the limelight in recent years, but it is worth noting that lectins are actually found throughout all of nature, including the animal kingdom. At least 12 categories of naturally-occurring animal lectins have now been identified.
For the most part, lectins play the same role in plants as they do in animals: they provide a defense system, protecting the plant or animal from pathogens (e.g., viruses, microorganisms, fungi).
The lectin-containing plant foods that have received most attention recently are the legumes (e.g., kidney bean, soybean), whole grains (e.g., wheat, rice), and even some fruits and vegetables (e.g., potatoes, tomatoes), particularly in their raw forms. If animals are fed those foods, they become exposed to the plant lectins in addition to their own endogenous lectins.
Common foods containing higher lectin content:
- Black beans
- White or red kidney beans
- Soybeans
- Green beans
- Fava beans
- Lima beans
- Lentils
- Whole grains (e.g., wheat)
- Cassava
- Tomatoes
- Potatoes
Indeed, it is true that consuming raw or undercooked beans would be problematic and gut-disruptive for most people. The undigested lectins may cause inflammation and loss of tight junctions at the gut barrier. They might also stimulate the production endotoxins, ultimately provoking a system-wide immune response due to the presence of lectin receptors on various tissues. Some authors have speculated that plant lectins could also cause nutrient malabsorption, and have proposed that symptoms of acute lectin toxicity include diarrhea, nausea, and vomiting.
The issue with food, however, is that the amount of lectins in a given plant food can vary substantially based on the growing season, as well as how the food is prepared. The degree to which exposure to plant lectins may be problematic also varies from person to person. It is also worth keeping in mind that lectins may be part of the body’s first-line response to immune dysregulation, and, therefore, advantageous to immune activity.
Much of the data linking lectins to human health risks have come from cell culture and animal studies. The associations between lectin intake and human disease risk have not been definitively proven by human studies.
That said, there may be a segment of the population, potentially those with autoimmune conditions, that have greater sensitivity to the effects of lectins. This sensitivity may be due to changes in the composition of the gut microbiome, the overall health status of the gut, or to immune dysregulation with increased autoantibodies and tissue damage.
Vojdani et al. detected lectin antibodies in a small percentage (7.8-18%) of a nominally healthy population of 500 individuals. Despite these findings, in their concluding remarks they state: “We strongly disagree with this kind of misleading blanket condemnation of all lectins at all times everywhere.”
For those who have autoimmune conditions or even inflammatory bowel disease, it may be helpful to try to reduce the lectin content of the diet by avoiding lectin-containing foods, or by adopting cooking methods known to substantially reduce lectin content.
Since lectins are water-soluble proteins, boiling, steaming, or stewing lectin-containing grains and legumes can reduce the amount of lectins consumed. Soaking and fermenting are also known to lower lectins. Dry heat cooking and microwaving, however, are not effective at reducing lectin content.
Overall, while the literature on lectins is vast, and I would not claim to be an expert in glycobiology, there seem to be four key themes worth keeping in mind:
(1) The diverse types of lectins: We need to look at the variety of different lectins, how they may be functionally different, and whether they have distinct functions in different environments.
(2) Individual variance in immune system function: Whether lectins in plant foods are problematic may depend in part on an individual’s immune system, and whether there is autoimmunity, dysbiosis, or gut dysfunction on some level.
(3) The totality of lectin-containing foods consumed and the context in which they are eaten: We don’t eat “lectins,” we eat foods, some of which contain lectins—along with thousands of other compounds and millions of microorganisms.
(4) How lectin-containing foods are prepared: As noted above, preparation methods make a big difference in the total amount of lectins consumed.
In evaluating the idea that lectin-containing foods are problematic, I began to question whether it is really the lectins, or if there is something else even more detrimental such as pesticides, herbicides, and insecticides, that may be causing problematic food-related responses. Many crops can be contaminated with any number of toxicants (e.g., glyphosate), in addition to mycotoxins, and heavy metals like arsenic in rice.
If we adhere to the principle of dietary diversity, ensuring that we get a rotation of different types of foods, we may be able to free ourselves from the tendency to become overly focused on the “trees” of trying to omit particular plant compounds, and rediscover the “forest” of a healthful, plant-rich diet.
In general, there are still many unanswered questions with respect to what might make an individual more sensitive to a lectin-containing food (e.g., gene variants, gut microbiome, immune imbalance). We also need to understand more about ways to reduce lectins if they are indeed problematic. We know that cooking methods can affect lectin content. But what about cultivation methods? I might suspect that if lectins are part of a plant’s defense system, they might be higher in organically-grown foods. But we really don’t know.
The topic of lectins also begs the question of whether we are too narrowly focused on one group of compounds, which leads some people to completely omit foods that for centuries have been part of the diets of many cultures that show longevity.
Let’s not forget that there are several large human population/epidemiological studies that support inclusion of lectin-containing foods like whole grains, legumes, and nuts in the diet. These food groups are associated with lowering the risk of cardiovascular disease and type 2 diabetes. They are also good sources of protein, fiber, minerals, and healthy fats. That’s why we cannot simply narrow in on lectins as the sole culprit and eliminate entire categories of foods. A balanced approach seems warranted.
Oxalates
Oxalate (oxalic acid) is an organic acid that can bind to minerals such as calcium, iron, and magnesium to create oxalate salts (e.g., calcium oxalate). Like lectins, oxalate is made in both plants and mammals. In plants, it is part of the defense system, and also plays a role in calcium regulation. In mammals, it’s a metabolic byproduct of glycine, glycoxylate, hydroxyproline, and ascorbate. Consequently, collagen powder, gelatin, and even vitamin C are potential contributors to urinary oxalates.
Unbound oxalates can bind to minerals in the intestine, reducing their absorption. Dietary oxalates, once absorbed, can contribute to the formation of kidney stones, which are made of calcium oxalate.
Plant foods with high oxalate levels include spinach, Swiss chard, rhubarb, sorrel, taro, sweet potatoes, and beets. Oxalates tend to be most concentrated in leaves. Other foods with smaller amounts include raw legumes, whole grains, nuts, tea, and cocoa. In the average diet, spinach (cooked and raw) tends to be the most common oxalate contributor (about 40%).
Similar to lectins, the oxalate content of plant foods can be modified by cooking methods. Wet methods such as boiling and steaming are efficient in decreasing soluble oxalates, although there can be quite a range of decrease depending on the vegetable and the surface area exposure. Boiling is more impactful than steaming. Wet cooking offers the double benefit of enhancing mineral availability.

Since oxalates tend to bind minerals, another way to offset the effects of oxalates is to pair oxalate-rich vegetables with calcium-rich foods.
A large prospective study involving three different cohorts (Health Professionals Follow-up Study with 45,985 men; Nurses’ Health Study I with 92,872 older women, and the Nurses’ Health Study II with 101,824 younger women) points to the importance of getting adequate calcium in the diet (800-1,000 mg daily) to buffer against the effects of oxalates. But this study also showed there was no difference in dietary oxalate intake between kidney stone formers and non-stone formers, which suggests that there could be other factors aside from oxalate exposure, underlying nephrolithiasis.
Researchers at Boston University hypothesized that the differential response to oxalates in food might be due not only to the oxalate content, the method of cooking/preparation, or the mineral intake, but also to the presence of Oxalobacter formigenes in the gut. This microorganism, present in 38 to 77% of the normal adult population, degrades oxalate. Testing for O. formigenes and supplementation with a probiotic that contains this bacterium may be a potential therapy to help people who are prone to urinary stone formation.
Phytates
Phytate, also known as phytic acid or myo-inositol hexaphosphate (IP6), is a storage form of phosphate and inositol found in whole grains, legumes, nuts, and seeds. Phytate is known to bind to divalent cations like iron, calcium, and zinc, preventing their intestinal absorption.
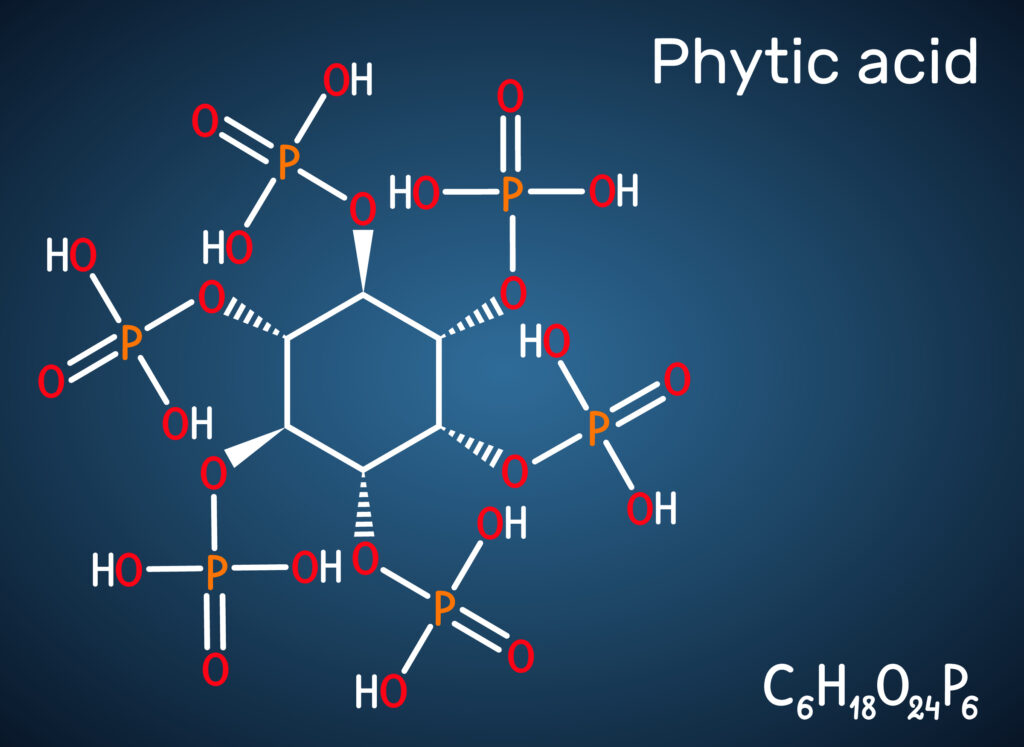
When evaluating the potential impact of phytate on mineral absorption, it is important to consider the food matrix, particularly the fact that the phytate co-exists in with dietary fiber in plant foods. The fiber can be fermented, which alters pH, and which can ultimately enhance the absorption of minerals.
Vitamin C may have a similar effect in that it may be able to override the inhibitory effects of phytate on iron absorption.
Furthermore, some researchers have suggested the concept of “phytate adaptation”. It refers to the adaptive ability of the intestinal microbiota to degrade phytates when presented with a consistent high-phytate diet.
As with lectins and oxalates, food preparation methods have impact on phytate content. Soaking, fermenting, and germination can all help to reduce phytates in foods such as legumes and grains.
Similar to lectins, there may also be beneficial effects of phytates. As Pujol et al point out in their very recent review article, phytate is the major phosphorus reservoir in nearly all whole grains, legumes, and oil seeds. These food groups represent a major part of the most well-studied, healthful dietary pattern–the Mediterranean diet.
Pujol and colleagues stress that the antinutrient effect of phytate in causing mineral deficiencies has not been reported in humans. Rather, based on its antioxidant, anti-inflammatory, anti-cancer, hypoglycemic, bone-protective, neuroprotective, and other healthful properties, phytate might have potential as a nutraceutical ingredient.
Lectins, oxalates, and phytates are three of the most frequently discussed anti-nutrients, but there are others, including: glucosinolates (goitrogens), polyphenolic phytoestrogens, and tannins. Based on our research, I compiled a colorful, easy-to-use 2-page guide describing the most important anti-nutrient categories, the foods which contain them, their potential health risks and benefits, and the ways to reduce their if they are problematic. The guide is available for download free-of-charge.

A Complex Question
The topic of anti-nutrients teaches us about complexity: of foods, of our bodies, and of the interactions between them. I don’t claim to have the absolute answer on anti-nutrients and whether or not large numbers of people need to be halting intake of tomatoes, tea, or spinach due to the presence of lectins, tannins or oxalates.
What I do think we know is that personalization is of utmost importance. There could be something about a food that simply doesn’t sit right with someone’s physiology in a moment in time. It may span the spectrum of quantity, timing, preparation, or even combinations of foods put together. It does not necessarily mean that this particular food is always “bad,” or “bad” for everyone.
Therefore, it’s good to continue to expand our knowledge base, yet keep what we think we know in check. If we adhere to the well-researched principle of dietary diversity, ensuring that we get a rotation of different types of foods for the benefit of many body systems, we may be able to free ourselves from the tendency to become overly focused on the “trees” of trying to omit particular plant compounds, and rediscover the“forest” of a diverse, plant-rich, and healthful diet.
END
Deanna Minich, MS, PhD, CNS, IFMCP, is a nutrition scientist, international lecturer, teacher, and author, with over twenty years of experience in academia and in the food and dietary supplement industries. She is the author of six consumer books on wellness topics, four book chapters, and fifty scientific publications. Her academic background is in nutrition science, including a Master of Science in Human Nutrition and Dietetics from the University of Illinois at Chicago (1995), and a Doctorate in Medical Sciences (nutrition focus) from the University of Groningen in the Netherlands (1999). For a decade, she was part of the research team led by the “father of Functional Medicine,” Jeffrey Bland, PhD, and has served on the Nutrition Advisory Board for The Institute of Functional Medicine. Dr. Minich is Chief Science Officer at Symphony Natural Health.







