Pulmonary inflammation has been in the public spotlight since the start of the COVID-19 pandemic. Formerly obscure immunology terms like “cytokine storm” are now common, as we learn more about how the immune system responds to SARS-CoV-2 and other viral pathogens.
The intense immune reactions seen in severe COVID cases and other forms of Acute Respiratory Distress Syndrome (ARDS) are mediated in part by Inflammasomes–multi-protein complexes found in the cytosol of immune cells, pulmonary endothelial cells, and other epithelial cells.
What are Inflammasomes?
Inflammasomes are typically formed in response to specific stimuli including pathogenic microbes, environmental insults, or inflammatory signaling molecules. As part of the innate immune system and the body’s first line of defense, inflammasome activation leads to the release of pro-inflammatory cytokines IL-1B and IL-18. In the lungs, IL-1B is one of the most potent inflammatory cytokines, and it is a major factor in ARDS.
In ordinary circumstances, inflammasome activation is a discrete and limited process resulting in a clearance of the triggering noxious stimuli such as infectious pathogens, environmental or metabolic toxins. However, the excessive activation of inflammasomes can result in increased and prolonged cytokine release, chronic inflammation and pulmonary and endothelial damage.
Inflammasome activation also triggers pyroptosis, a rapid form of programmed cell death. Pyroptosis is a highly inflammatory state usually triggered in response to intracellular pathogens.
The good news is that many phytochemicals naturally occurring in certain herbs and plant foods can down-regulate inflammasome activation.
Inflammasome Dysregulation
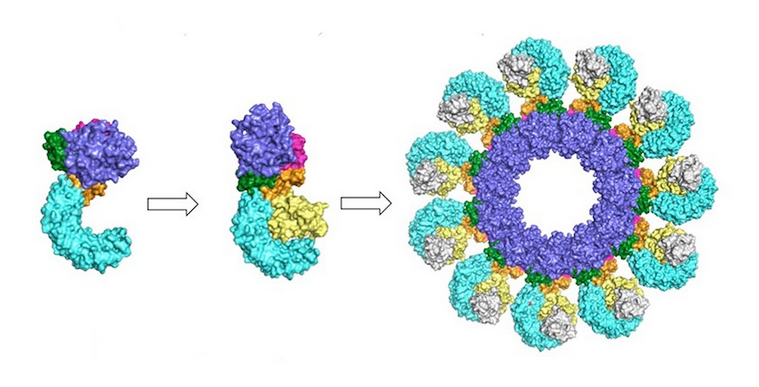
There are many different types of inflammasomes. The NLRP3 subtype is the most prevalent and most well studied pulmonary inflammasome. This has significance in the context of the COVID-19 pandemic because some viruses, including the corona family of viruses, activate the NLRP3 pulmonary inflammasome.
After exposure to a pathogen like coronavirus, NLRP3 Inflammasome activation is initiated in part by an efflux of potassium ions and an influx of calcium ions. At the same time, there is an increase in pro-oxidative Reactive Oxygen Species (ROS) and lysosomal proteases. This is accompanied by activation of NFkB, the nuclear factor that is upstream of a cascade of intracellular pro-inflammatory pathways and macrophage activation.
Combined, these processes create a highly pro-inflammatory environment, with high levels of oxidative stress and proteolytic enzymes, predisposing to thrombus and fibrin formation. At the cellular level, this is war.
When this response is mobilized, an infection can be quickly neutralized. The inflammatory cascade should then turn off, enabling the body to restore equilibrium.
In situations like we’ve seen with severe COVID and other acute respiratory infections, this cascade does not turn off, resulting in a prolonged cytokine “storm” that can cause serious, sometimes fatal tissue damage.
Inflammasome dysregulation leads to excessive cell death, tissue fibrosis, and ultimately, organ dysfunction. Chronic diseases such as COPD, auto-immune inflammatory syndromes, Crohn’s disease, Type 2 Diabetes, Alzheimer’s disease, atherosclerosis and cancers are all associated with dysregulation of the inflammasomes, upregulation of NFkB, and other inflammatory cytokines.
Respiratory distress in the context of inflammasome dysregulation is not always responsive to exogenous oxygen therapy. That’s because the alveoli themselves become damaged and dysfunctional. Further, there is also endotheliitis in the capillary beds surrounding the alveoli, leading to hypercoagulation and thrombus formation. The net result is that the alveoli are unable to deliver oxygen to the blood.
This creates a deadly feed-forward cycle, because the resulting hypoxia is itself a signal for activation of the NLRP3 inflammasome. This is a perfect storm for respiratory failure, severe morbidity, and all too often, death.
Quelling Inflammasome Activation
There are many natural compounds can act as regulators and modulators of pulmonary NLRP3 inflammasome activation and its sequela. Phytochemicals including lectins, flavones, flavonoids, stilbenes, catechins and other phenolic compounds derived from both food and therapeutic plants can modulate the NLRP3 Inflammasome activation and down-regulate inflammatory cytokines IL-1B, TNFa, NFkB as well as ROS.

Curcuminoids are lipid soluble polyphenol isolates derived from Rhizoma Curcuma longa (Turmeric). Small amounts of curcuminoids are also found in the rhizomes of Zingiber (Ginger) species. Curcumin is widely studied and has been found to be a negative regulator of NLRP3 inflammasome expression through multiple pathways. It is also a mediator of inflammatory signals including NFkB, TNF-α, and downstream cytokines including IL-1B.
Curcumin’s bright yellow color announces its value as a scavenger of ROS and modulator of oxidative stress. The absorption of curcuminoids from turmeric-rich foods and supplements is enhanced with the addition of black pepper. The most absorbable curcumin supplements are lipid based.
Resveratrol is a stilbene polyphenol present in abundance in the skins of red and purple grapes, and in the plant Polygonum cuspidatum. It is the trans-resveratrol isomer that is most biologically active. Resveratrol has been widely studied and like most polyphenols, it scavenges ROS and reduces oxidative stress.
Resveratrol up-regulates the expression of Sirtuin I which is a deacetylase enzyme that inactivates multiple inflammatory genes. Resveratrol also activates AMPK which attenuates NLRP3 inflammasome activation, NFkB transcription, and IL-1B secretion.
Epigallocatechin-3-gallate (EGCG) is the major bioactive polyphenol found in Green Tea (Folium Camellia sinensis). It inhibits NLRP3 inflammasome activation, and also reduces the expression of NFkB, matrix metalloproteinases, IL-1B, IL-6 and TNF-α. EGCG’s antioxidant properties and ability to scavenge ROS are also well-documented. A single cup (8 oz or 250 ml) of brewed green tea contains approximately 50-100 mg of EGCG. EGCG catechin is also available in capsules.

Sulforaphane glucosinolate (SFN) is a natural compound found in cruciferous vegetables. Sulforaphane inhibits activation of multiple inflammasomes including NLRP3. It also reduces IL-1B secretion and NFkB expression, and quenches oxidative stress and ROS. Food sources include kale, broccoli, broccoli sprouts, Brussel sprouts, cabbage, bok choy, mustard greens, and radishes.
Sulforaphane is an isothiocyanate produced from a precursor called glucoraphanin, in the presence of the myrosinase enzyme. It is best to lightly cook (steam or sautee) or massage cruciferous vegetables to liberate their phytochemicals. There are a number of supplement products now available that include Sulforaphane, Glucoraphanin, DIM (di-indole-methane) and I3C (indole-3-carbinol) in capsule or powder form. The highest quality products are derived from broccoli sprouts and broccoli seeds.
Quercetin is a flavonoid commonly found in a wide variety of fruits, vegetables and herbs. It has been shown to block NLRP3 inflammasome activation inhibit damage from ROS and modulate multiple inflammatory pathways and downregulate NFkB expression and IL1B secretion. The red skin of apples and purple onions are rich dietary sources of quercetin. Quercetin as a supplement is not highly absorbable and is best taken with healthy fats and oils or encapsulated as a lipid phytosome.
Ginsenosides are major active saponin components of Radix Panax Ginseng. Ginsenosides attenuate NLRP3 Inflammasome activation and NFkB expression. They also reduce IL-1B, IL-18 and TNF-α levels.
Modified Citrus Pectin (MCP) is a low molecular weight dietary fiber derived from the inner peel of citrus fruit. It is best known as a Galectin-3 antagonist. Galectin-3 is widely found in immune and epithelial cells and it promotes NLRP3 inflammasome activation and pyroptosis.
While unprocessed food pectin is a large lectin molecule that is not digested or absorbed through the intestinal epithelium, MCP is an enzyme-processed product that yields a small esterified molecule that can be absorbed through the small intestine and enter the bloodstream. By binding and inactivating Galectin-3, MCP down-regulates the activation of the NLRP3 inflammasome, reducing pyroptosis and cell death. It also reduces secretion of inflammatory cytokines IL-1B and IL-6, and matrix metalloproteinases. Further, MCP inhibits fibrin formation minimizing the hypercoagulation and thrombus formation that follows from dysregulated inflammasome activity.
The highest quality MCP nutritional products have the smallest particle size to insure intestinal absorption.
Potassium: Due to the potassium efflux that occurs at the initiation of inflammasome activation, oral potassium repletion makes sense, according to Joe Pizzorno, ND. For patients who follow a plant-based diet, there should be no shortage of potassium ingestion. However, an elderly, very ill, or hospitalized patient who is not eating normally could be potassium-depleted.
For such at-risk patients, it is wise to monitor potassium as well as the full range of electrolytes.
Food as Medicine
Cancer is also a chronic inflammatory illness. The selected natural compounds reviewed here also form the core Materia Medica found to shift the tumor microenvironment and the cancer terrain away from inflammation, hypercoagulation, immune suppression, carcinogenesis, proliferation, angiogenesis, and metastasis.
Many of the natural compounds that influence inflammasome activation are found in plant food. These phytochemicals are pleomorphic multi-taskers and can bind to many different receptors and influence a lot of different pathways and genes at once.
Therefore, encourage patients who are concerned about their immune system health to eat a plant-rich, colorful, rainbow diet that includes a variety of herbs and spices. A diet rich in phytochemicals has a powerful impact on long term health and enhances inflammation control. Remind patients that, “Our food is talking to our genes. This is why it matters what we eat.”
END







