
Should people with Health Savings Accounts (HSAs) be permitted to use their tax-deferred dollars to buy dietary supplements and herbal medicines?
It’s a question that will once again confront members of Congress in the months to come.
Under current federal tax rules, supplements are excluded from HSAs and also from Flexible Spending Accounts (FSAs), unless they are explicitly prescribed by physicians. Over the years, self-care advocates and supplement industry trade groups have challenged that policy, to no avail.
Now, it appears the idea has found some new congressional allies.
On July 20, Rep. Darin LaHood (R-IL), son of longtime conservative stalwart Ray LaHood, introduced a new bill titled the Dietary Supplements Access Act, calling for amendments of the federal tax code that would include all types of supplements in HSAs and FSAs. LaHood has a senior position on the influential House Ways and Means Committee, which will likely have influence on the future of the bill.
LaHood’s co-sponsors are Reps. Brendan Boyle (D-PA) and John Curtis (R-UT), and John Gottheimer (D-NJ), a coalition that suggests the proposition has a fair degree of bipartisan support.

The bill emerged from a renewed joint effort by the five major supplement industry organizations–the Council for Responsible Nutrition, the American Herbal Products Association, the Consumer Health Products Association, the Natural Products Association (NPA), and the United Natural Products Alliance (UNPA)—to end the exclusion and redefine supplements as eligible HSA/FSA expenses.
According to Patricia Knight and Peter Reinecke, political advisors to the UNPA, more than 35 million Americans have tax-preferred HSAs, representing over $100 billion. An additional 21 million people have FSAs through their employers.
UNPA and the other industry organizations contend that the longstanding exclusion of supplements as an eligible expenditure denies HSA and FSA-holders full freedom of choice, and reflects a nonsensical bias against one of the cornerstones of a healthy lifestyle.
A Strong Case
On June 21, Steve Mister, CEO of the Council for Responsible Nutrition, along with executives from several member companies, met with representatives on both sides of the political divide to advocate for the new bill which, if made law, would include, “everything that has a ‘Supplement Facts’ box on the label” as an eligible FSA/HSA expense.
In an interview with Nutraingredients USA, Mister said he was optimistic about the future of the proposal.
The new bill is essentially the same as the Dietary Supplements Access Act (HR 5214), introduced in 2021 by Rep. Curtis. It declares all vitamin, mineral, amino acid, and botanical supplements to be eligible expenses.
HR 5214 failed to make it past the House Ways and Means committee in 2021.
Mister says CRN and other industry groups have done a lot of homework since then, and he feels they are now much more able to make a strong case.
Broad adoption of evidence-based supplementation strategies for six conditions—coronary artery disease, osteoporotic fractures, age-related macular degeneration, irritable bowel syndrome, and childhood cognitive disorders—could potentially cut over $400 billion from the nation’s medical bill by 2030.
Addressing Objections
Congressional objections to the proposal tend to fall into two general categories.

Some lawmakers view HSAs and FSAs as “tools for rich people as tax dodges,” he explained. They tend to view any expansion of HSA/FSA benefits as further opportunity for wealthy people to avoid paying their fair share.
To redress this perception, he points to a survey of HSA/FSA holders showing that, “the vast majority of people using these accounts are not wealthy “one-percenters,” but rather, ordinary middle-class working Americans.
Further, the survey showed that 78% of the 1,100-plus account holders want to be able to use their tax-exempt healthcare savings to purchase supplements.
“They want that flexibility. They want to be to do things that are more proactive on healthcare, and not just use their HSA reimbursements for co-pays on doctor bills and prescriptions when they’re sick,” Mister told NutraIngredients.
78% of the 1,100-plus account holders surveyed want to be able to use their tax-exempt healthcare savings to purchase supplements.
The other major congressional objection is the belief that expanding HSA/FSA benefits would encourage diversion of more money away from taxable income streams, which would negatively impact the national treasury.
To this, Mister cites data showing that in reality, peoples’ decisions about FSA/HSA allocations come down to how much they believe can afford to take out of their paychecks, which is typically not that much. Tax avoidance is rarely a driving factor.
Potential Cost Savings
He contends that measures to encourage wider use of supplements would lead to long-term, system-wide cost savings.
A 2022 study called Supplements to Savings indicates that broad adoption of evidence-based supplementation strategies for six conditions—coronary artery disease, osteoporotic fractures, age-related macular degeneration, irritable bowel syndrome, and childhood cognitive disorders—could potentially cut over $400 billion from the nation’s medical bill by 2030.
Data like that, Mister says, should be able to win over the nation’s elected officials. “In so many places, government is paying for healthcare—whether it’s VA benefits, or Medicare, or Medicaid. They’ve got a real interest in lowering healthcare costs. So, with all of that together, we had a pretty compelling argument.”
It remains to be seen whether the cost-savings argument will prevail in a gridlocked, highly partisan congress bent on “fiscal restraint,” as UNPA’s political advisors have termed it. Knight and Reinecke note that the influential Joint Committee on Taxation (JCT), which rates the budgetary impact of all tax-related legislation, has in the past scored proposals for supplements in HSAs as a net cost, not a savings, for the government.
Advocates for the revision are urging practitioners, patients, and any other interested parties to call or write to their congressional representatives and urge them to support and co-sponsor the bipartisan Dietary Supplements Access Act.
A Push for Vitamin D
The HSA/FSA campaign is not the only current attempt to crack the federal government’s intransigent attitude toward supplements.
Earlier this year, a coalition of nutrition advocacy groups led by the Organic & Natural Health Association (ONHA) is urging Congress to include vitamin D as an eligible expense under the federal Supplemental Nutrition Assistance Program (SNAP).

The campaign, titled All for Vitamin D: Building Stronger Families in a SNAP, is a joint effort between ONHA, the Council of Holistic Health Educators, the Independent Natural Foods Retailers Association (IFRA), Natural Grocers, and SENPA Natural Products alliance to improve the health impact of the SNAP program.
Dietary supplements, including vitamin D, are excluded from SNAP, aka “Food Stamps,” and from other federal healthcare programs.
“Permitting more low-income citizens to buy vitamin D with SNAP will ultimately reduce the burden of chronic disease, cut healthcare expenditures, and save taxpayer dollars.”
–Karen Howard, Executive Director, Organic & Natural Health Association

ONHA and its allies are working to change that by rallying health-conscious citizens, nutrition industry representatives, and medical professionals, to urge their elected officials to amend the Farm Bill which governs SNAP, to allow recipients to purchase vitamin D using their SNAP dollars.
An Affordable Solution
“Vitamin D3 supplements offer an affordable solution to address a range of health challenges faced by families, including preterm births, depression, respiratory infections, asthma, cancer, and chronic diseases like cardiovascular issues, high blood pressure, and Type 2 diabetes,” says Karen Howard, ONHA’s CEO, in a statement announcing the advocacy campaign.

Permitting more low-income citizens to buy vitamin D with SNAP will ultimately reduce the burden of chronic disease, cut healthcare expenditures, and save taxpayer dollars, says Howard.
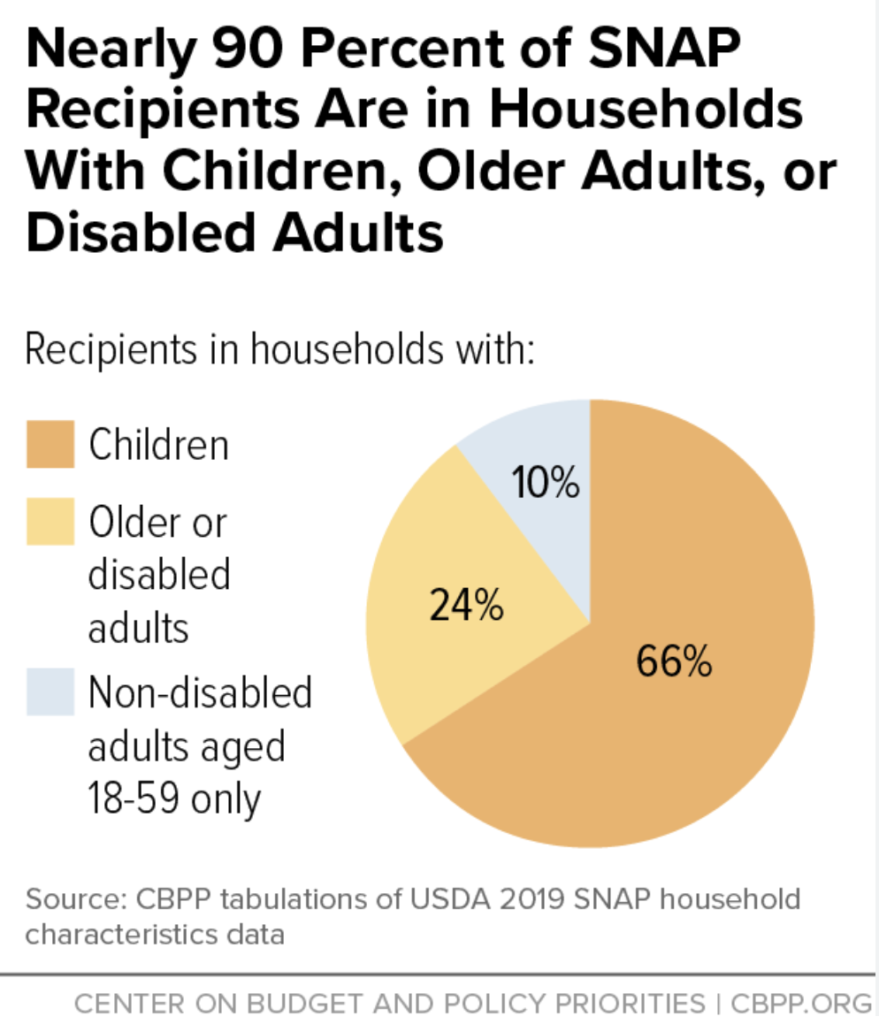
Over 41.2 million Americans—roughly 12% of the US population—are now enrolled in SNAP, which was born out of federal food assistance programs created during the Great Depression in the 1930s. The modern SNAP program’s stated intention is to provide “food benefits to low-income families to supplement their grocery budget so they can afford the nutritious food essential to health and well-being.”
Cruel Irony

In practice, a lot of products that people can buy using SNAP are very far from “nutritious” or “essential to health.”
Soft drinks, cookies, cakes, and a wide variety of nutritionally-void junk foods are considered “eligible” under existing SNAP rules. According to a 2016 report by the US Department of Agriculture, sodas are the top most-purchased commodity by SNAP beneficiaries.
All for Vitamin D’s leaders point out that, “While SNAP permits the purchase of a diverse range of foods, encompassing fruits, vegetables, grains, dairy, and proteins, it lacks explicit guidelines concerning the quality and nutritional value of these items.
When it comes to meeting therapeutic vitamin D levels (40-60 ng/ml), SNAP falls short, especially since it is very difficult to obtain these levels solely via food or sunlight exposure. This is doubly true for dark-skinned people, who represent a disproportionate number of SNAP recipients.
ONHA cites several studies showing that people who maintain their serum vitamin D levels 40 ng/ml obtain myriad health benefits, including a 60% reduced risk of preterm birth and a 65% lower cancer risk, and decreased incidence, severity, and morbidity from Covid-19.
In practice, a lot of products that people can buy using SNAP are very far from nutritious. Soft drinks, cookies, cakes, and a wide variety of nutritionally-void junk foods are considered eligible under existing SNAP rules. Supplements are excluded as “non-foods.”
An Ongoing Effort
The All for Vitamin D campaign is the latest step in a long, arduous effort to convince lawmakers to expand SNAP’s definition of “food.”
In 2017, Rep. Mike Rogers, an Alabama Republican, introduced the SNAP Vitamin and Mineral Improvement Act which would have modified the program to include a broad range of vitamins, minerals, and other supplements as an eligible expense.
Rogers’ bill had strong support from nutrition industry trade groups, as well as some high-profile policymakers, and was included in the House version of the 2018 Farm Bill. But was killed in the Senate, despite strong advocacy from longtime supplement advocate, Sen. Orrin Hatch.

At the time Senate agriculture committee chairman Pat Roberts (R-KS) and ranking Democrat Debbie Stabenow (D-MI) opted to cut all Farm Bill amendments that might be perceived as partisan obstacles to smooth passage. The committee deemed Rep. Rogers’ proposal as one of those obstacles, and nixed it from the final 2018 version.
Under SNAP’s current rules, vitamins and supplements are considered “non-food” and therefore ineligible for purchase with SNAP dollars. Policymakers justify the exclusion, arguing that if beneficiaries can use SNAP coupons for supplements, they will divert their limited funds away from “real” food. That’s ironic given the myriad junk foods and beverages now covered by the program.

Further, the notion that everyone can derive all important nutrients directly from food, and that supplements encourage people to skip “real” meals, ignores the fact that many people relying on SNAP and other forms of food assistance already miss meals simply because they don’t have enough to eat.
The average SNAP benefit equals around $4 per person per day, or approximately $1.40 per meal. That doesn’t go very far given today’s food prices.
By playing to the strong science on vitamin D, the widespread prevalence of deficiency, and the staggering scope of food insecurity, ONHA and its allies have a fighting chance to win the minds and hearts of some lawmakers.
Missed Opportunities
Outside of SNAP, many other food assistance programs such as local food banks and food pantries also exclude supplements.
The number of people visiting food banks, already high before Covid, has soared since the pandemic. Three years on, 80% of food banks still report either an increase in or a steady demand for emergency food relief month-to-month, according to Feeding America. Nationwide, food banks and related programs are serving 55% more people than before Covid. According to the organization, Feeding America, at least 60 million Americans visited food banks last year.
The average SNAP benefit equals around $4 per person per day, or approximately $1.40 per meal. That doesn’t go very far given today’s food prices.
As is the case with SNAP, many people who rely on community pantries are unlikely to get all the nutrients they need through diet alone. Yet these programs do not provide dietary supplements.
Administrators at food banks say they often receive donations of supplements from retailers, distributors, food drive collections, and manufacturers. But these products create a real conundrum. On one hand administrators recognize their potential for improving nutritional status, but on the other they are aware of issues like purposeful or accidental adulterations and exaggerated product claims.
There are no established standards for evaluating the safety and potential benefits of supplements, so food bank staffers—who are typically overwhelmed by the sheer number of people they must serve–are left to their own judgment in deciding whether or not to distribute supplements.
Supplements are not the ultimate answer to poor nutrition among the nation’s poorest citizens. But they could be important tools in helping people move toward better overall health.
In 2019, a national program called Healthy Eating Research (HER) convened an expert panel “to improve the quality of foods in food banks and pantries in order to increase access to and promote healthier food choices.”
The group issued a final report in March 2020 entitled, Healthy Eating Research Nutrition Guidelines for the Charitable Food System. The guidelines acknowledge the existence of dietary supplements, grouping them among protein powders, baby food, and other “miscellaneous items” that are “considered necessary only for specific populations or when treating specific disease states.”
Though HER does not categorically dismiss supplements, it definitely counsels against wide use, and does not provide practical guidelines for food pantry administrators.
The reality is, supplement products rarely make it to the pantry shelves.
Vitamins, minerals, and other supplements are not the ultimate answer to poor nutrition among the nation’s poorest citizens. But they could be important tools in helping people move toward better overall health.
END







