 Urinary incontinence is far more common than many people realize. That’s because people with bladder issues are often ashamed of the condition and tend to hide their suffering and avoid seeking treatment.
Urinary incontinence is far more common than many people realize. That’s because people with bladder issues are often ashamed of the condition and tend to hide their suffering and avoid seeking treatment.
Adding to the challenge of treating incontinence and overactive bladder is the fact that the commonly prescribed anticholinergic drugs for these conditions can cause adverse effects so unpleasant that patients often drop the treatments. Recent studies link the long-term use of certain widely prescribed bladder drugs to serious cognitive issues including dementia.
Fortunately, there are alternatives. Medicinal herbs including Crataeva nurvala and Equisetum arvense (aka Common Horesetail), used in combination, can safely address urinary dysfunction without the concerning side effects.
As Common as Arthritis
Bladder control issues like incontinence affect roughly the same number of people as does arthritis. Yet we hear about achy joints, and the therapies available to treat them, far more frequently.
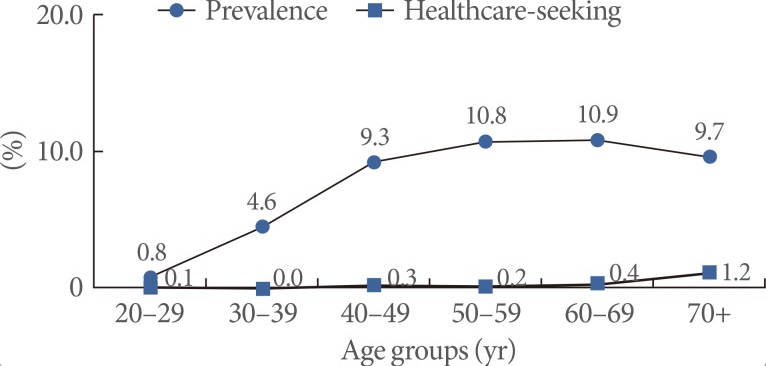
“Research shows that about 50% of people will not tell their doctor if they are experiencing bladder symptoms,” says Tracey Seipel, ND, a naturopathic physician based in Newmarket, Australia, whose particular interest is in natural therapies for urinary disorders.
Seipel told Holistic Primary Care that many people affected by incontinence are too ashamed to tell even their spouses or other close family members. Tracey Seipel, ND, Seipel Group Founder & CEO
Lower urinary tract symptoms (LUTS) fall into two main categories: overactive bladder (OAB) and urinary incontinence (UI).
According to the American Urological Association (AUA), an estimated 33 million Americans have OAB, making it a more common condition than either diabetes or asthma. OAB is marked by a sudden and pressing urge to urinate caused by bladder muscle overactivity.
UI impacts over 58 million Americans, according to a National Institutes of Health report from 2012––the most current year for which data is available. This occurs when the muscles in the bladder that control urine flow contract or relax involuntarily.
Assuming some overlap in patients with both OAB and UI, conservative estimates suggest that a minimum of 60 million people in the US––around one in six Americans––are coping with at least one bladder issue. But because symptoms are hugely underreported, it’s hard to determine exactly how many people experience OAB with or without co-occurring UI.
Silent Suffering
“The biggest obstacle we face right now is that nobody wants to talk about this,” Seipel explained.
Many with bladder issues become reclusive and withdrawn. “We see an acceptance and a resignation that there’s nothing that can be done.”
Suffering in silence takes a significant toll on patients’ mental health, sleep patterns, sexual wellness, nutrition, and overall quality of life.
Those who do not seek treatment tend to find ways to cleverly manage the problems on their own. Seipel described patients who’ve created makeshift absorbent padding, kept bottles next to their beds to urinate into at night, or simply learned to deal with getting out of bed five times nightly to use the bathroom.
 Few people realize that supplementing with the right medicinal herbs could help put an end to their silent suffering. Seipel says her work today remains largely focused on bringing bladder disorders “out of the closet.”
Few people realize that supplementing with the right medicinal herbs could help put an end to their silent suffering. Seipel says her work today remains largely focused on bringing bladder disorders “out of the closet.”
Coming Out
Seipel is well-versed in the holistic treatment of urinary disorders. After completing her naturopathic training, she worked as a product formulator for a number of Australian nutraceutical companies in the 1990s. During that time, she came across a surprising survey by Australian Women’s Weekly, a popular publication in Seipel’s home country. The magazine published a list of health conditions and asked readers to rank them in order of personal importance.
To Seipel’s surprise, readers identified UI among their top five health concerns.
“If this many women reading this magazine are identifying this as one of their biggest health concerns, this is a big issue.”
From that point on, Seipel prioritized researching natural treatments for bladder conditions. At the time, the mainstream medical community was still figuring out how to define different urinary disorders. It was not until 2002 that the International Continence Society formally defined “overactive bladder syndrome” (OABS) as a distinct condition.
Much like menopause 30 years ago, or male prostate issues 50 years ago, Seipel said that in the 90s, “bladder issues weren’t being discussed at all. There was a disconnect to this mysterious part of the body that nobody knew much about, so nobody talked or asked about the bladder.”
She launched her first botanical formula for bladder control in 1999. The key herbs were extracts derived from Crataeva nurvala, a small tree native to India and Southeast  Asia, the bark of which is used in Ayurvedic medicine for bladder-related problems, and Equistem arvense (aka Common Horesetail) which has a long history of use in Western herbal medicine as a treatment for eneuresis and incontinence.
Asia, the bark of which is used in Ayurvedic medicine for bladder-related problems, and Equistem arvense (aka Common Horesetail) which has a long history of use in Western herbal medicine as a treatment for eneuresis and incontinence.
In 2006, she received an award from the Nutrition Business Journal, in recognition of her opening of a new product category for natural bladder health. She was later inspired to found her own company, the Seipel Group, in 2011, for which she currently serves as CEO. The company has two flagship products: Urox––an update of Seipel’s original Crataeva / Equistem formula that also contains Lindera aggregata (Japanese Spicebush); and Prorox, a prostate health formula that combines the Urox formula with additional ingredients––Saw Palmetto extract, lycopene, vitamin D3, selenium, and zinc––that support prostate health in men.
Age Doesn’t Matter
One of the most pervasive myths about incontinence and OAB is that they are a normal part of aging, and that little can be done to prevent them.
It is true that incontinence is the third leading cause for admittance into elderly nursing care facilities (dementia and compromised mobility are the top two). With populations around the world now living longer than ever before, it is likely that clinicians will see an increase in patients with UI symptoms, Seipel says.
But that does not mean bladder problems are inevitable with advancing age. Nor are all affected people elderly. Incontinence can begin as early as one’s 20s or 30s, especially among women. A woman in her mid-20s might experience occasional bladder symptoms that she compensates for by making slight adjustments in her daily life.
“This is when intervention can really help,” Sepiel urged. “Because 30 years later, suddenly she finds that she is really changing her lifestyle because of her bladder issues.”
Several other factors can contribute to bladder symptoms, including sports-induced and other types of injuries. Damage to the spinal cord, for instance, can disrupt neural communication between the brain and the nerves that control bladder function, leading to incontinence.
Seipel’s own clinic employs a sports therapist who treats patients with injury-related urinary disorders. She stressed that age should not be a barrier to beginning treatment. She’s used her proprietary bladder formulas to treat multiple patients over the age of 100, each of whom she says experienced significant symptom improvement.
That said, the earlier urinary symptoms are identified and treated, the more likely patients will experience relief. Since symptoms tend to slowly worsen with age, there’s a possibility that use of the herbal combination early in life might prevent difficulties further down the road.
Gender Gaps
There’s another common misconception that bladder control problems are exclusively a “women’s issue.” While it is true that women are overall more likely to develop urinary incontinence, there are other bladder symptoms that uniquely impact men.
LUTS as a whole and OAB specifically are highly prevalent in both men and women and generally increase with advancing age.
“Contrary to popular perception, men and women have a similar prevalence of overactive bladder and symptoms such as occasional urgency, frequency, and nocturia,” states a Seipel Group white paper. Excessive nighttime urination is a key symptom of OAB.
“However, symptoms of occasional incontinence or leaks and accidents, are unique in their causes and how they are experienced by gender,” the authors note.
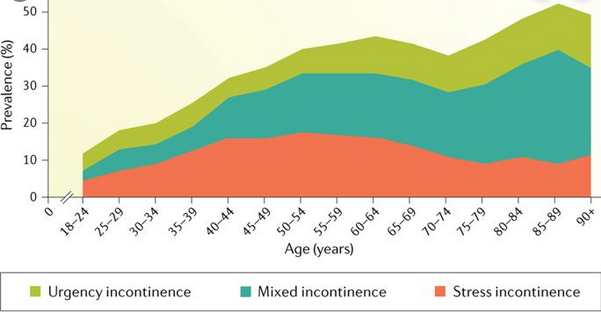
There are two main types of UI: stress incontinence and urge incontinence. They can occur separately, but some patients develop a mix of the two.
Stress incontinence occurs when weakness of or damage to the urethral sphincter, pelvic floor muscles, or both prevent the bladder from dependably holding urine. People experience urine leakage when a physical exertion––jumping, coughing, or laughing––puts pressure on the abdomen or bladder.
“Contrary to popular perception, men and women have a similar prevalence of overactive bladder and symptoms such as occasional urgency, frequency, and nocturia”
Urge incontinence is usually caused by an overactive bladder and occurs when the detrusor muscle––the smooth muscle lining the bladder wall––begins to contract, signaling a need to urinate even if the bladder is not full. This feels like an overwhelming impulse to urinate immediately, often followed by a release of urine before the person reaches a toilet. Nocturia and frequent urination (more than eight times in a 24 hour period) are common signs of urge incontinence.
Women are more likely than men to experience all forms of urinary incontinence, particularly stress UI. Bladder weakness affects 25% of reproductive-age women, 50% of post-menopausal women, and between 50–75% of women in nursing homes.
Pregnancy is also a factor. Up to 40% of women develop stress UI for up to one year postpartum, usually resulting from the increased pressure on the pelvic floor. The more children a woman has, the more likely she is to experience UI. Pregnancy-induced urinary symptoms usually resolve over time, but may return again after menopause and exacerbate with age.
Conditions like obesity or constipation may further increase pressure, heightening a woman’s risk. Incontinence also increases the likelihood of urinary tract infection due to more frequent urination.
LUTS are highly prevalent among men, too, occurring in up to 60% of males over the age of 40. In men, urge incontinence occurs more frequently than stress incontinence. Men are likelier than women to develop bladder voiding problems like hesitancy, poor stream, straining, intermittency, and dribbling, typically resulting from benign prostatic hypertrophy (BPH).
But keep in mind that urinary problems in men are not always prostate-related. “The problem with male LUTS is that men may often assume the prostate is the only culprit, whereas half the time the primary issue is OAB.” According to Dr. Seipel, many male patients are misdiagnosed with prostate conditions because clinicians overlook core bladder issues like detrusor muscle overactivity.
While it is important to support prostate health, this is only half the story. Seipel encourages clinicians to take a more careful assessment of the bladder.
Costly Treatments
To manage overactive bladder, many people rely on costly adult diapers or pads. In addition to the financial burden, these single-use diapers also generate massive volumes of waste that ultimately winds up in landfills.
Pharmaceutical options carry great costs of their own. Some physicians commonly prescribe anticholinergic drugs that help relax the bladder muscles. But many patients “don’t have great success with them, and others have to stop because of the side effects––especially increased thirst,” Seipel said.
Anticholinergics dry out the mucous membranes, causing dry mouth and constipation, and secondary problems like increased cold sores, thrush, and other infections, particularly in patients prone to those conditions.
These drugs can also cause drowsiness and short-term cognitive impairments like memory problems and confusion. Until recently, it was unclear whether or not the long-term use of anticholinergics raised the risk of more serious brain consequences.
According to a paper published this past June in JAMA Internal Medicine, these drugs are bad news for the brain.
The study involved more than 284,000 participants aged 55 years and older. Researchers identified statistically significant associations between dementia risk and exposure to anticholinergic bladder meds and antidepressants. Anti-Parkinson drugs, antipsychotics, and antiepileptic medicines are also problematic (Coupland, C et al. JAMA Intern Med. 2019; 179(8): 1084-1093).
The investigators, led by Carol Coupland, PhD, at the University of Nottingham, documented a nearly 50% increase in dementia risk associated with anticholinergic exposure of more than 1095 total standardized daily doses (TSDDs) within a 10-year period. That’s the equivalent of “3 years’ daily use of a single strong anticholinergic medication at the minimum effective dose recommended for older people.”
Coupland and colleagues argue that their findings “highlight the importance of reducing exposure to anticholinergic drugs in middle-aged and older people.” They advise considering alternative treatments where possible.
Theirs’ is not the only paper to caution against anticholinergics. A study published last year in the British Medical Journal also reported a “robust association between some classes of anticholinergic drugs” and dementia incidence. This included multiple antidepressant, urological, and antiparkinson drugs with “definite anticholinergic activity.” The negative cognitive effects persisted for “up to 20 years after exposure” (Richardson, K et al. BMJ. 2018; 361: k1315). The authors recommended limiting the use of anticholinergics to short periods of time and, in most cases, eliminating the use of these drugs as treatments for bladder control problems.
Ancient Herbs for Modern Health
Seipel contends that herbal remedies can provide a viable option for supporting bladder health. In developing Urox and Porox, she drew from her knowledge of ancient European and Asian herbal medicine and nutrition to create formulas that target multiple holistic aspects of the urinary system.
 The three herbs that comprise Urox––Lindera (Lindera aggregata) extract (root), horsetail (Equisetum arvense) extract (aerial parts), and three-leaf caper (Crateva nurvala) extract (stem bark)––have excellent safety profiles. The absence of adverse effects mean patients can start using the herbal formula at any time, regardless of age.
The three herbs that comprise Urox––Lindera (Lindera aggregata) extract (root), horsetail (Equisetum arvense) extract (aerial parts), and three-leaf caper (Crateva nurvala) extract (stem bark)––have excellent safety profiles. The absence of adverse effects mean patients can start using the herbal formula at any time, regardless of age.
The herbs work in tandem to strengthen and tone the muscles of the bladder wall, pelvic floor, and sphincter. They also support healthy connective tissues, allowing the bladder to fill appropriately and empty effectively.
“In a clinical trial involving 150 patients published last year, eight weeks of treatment with the three-herb combo, taken once daily, reduced OAB symptoms, incontinence, and the use of pads or adult diapers.“
Lindera aggregata is an Asian shrub that’s been used for centuries by traditional Chinese medicine practitioners. Also known by its Chinese name, Wu Yao, the herb is commonly used as treatment for bladder and kidney conditions, including frequent urination and loss of bladder control. It is said to promote the movement of chi and relieve pain and stagnation throughout the trunk of the body, especially in the lower abdominal region.
Modern research shows that Lindera exhibits impressive antioxidant activity (Han, H et al. Int J Mol Med. 2019; 43(1): 461-474); it can delay the progression of diabetic nephropathy in animal models (Ohno, T et al. Life Sci. 2005; 77(12): 1391-403). It is also an anti-inflammatory agent, used traditionally to treat rheumatic complaints like rheumatoid arthritis.
Equisetum arvense, commonly called horsetail or puzzlegrass, is another well-documented botanical whose therapeutic use in Europe has roots in ancient Roman and Greek medicine. It is the sole surviving member of the Equisetaceae family, a group of prehistoric vascular plants that reproduce by spores rather than seeds. The plant’s high silica content strengthens hair, skin, and nails, supports healthy tissue structure, and improves tissue toning and firming. Horsetail also balances urinary minerals, reducing the likelihood of bladder or kidney stone formation.
Crataeva nurvala is an Ayurvedic herb referred to as “the golden child for the urinary system in India,” Seipel said. Crataeva helps improve smooth muscle tone, enhancing bladder control and improving the force of urine expulsion. Lupeol, a Crataeva-derived triterpene, has anti-oxaluric and anti-calcuric effects that prevent kidney and bladder stone formation, aid with the passing of stones, and provide relief from stone-related symptoms.
Crataeva is also an effective treatment for interstitial cystitis. Both Crataeva and Lindera also have antibacterial properties and long histories of traditional use in treating chronic urinary tract infections.
In a clinical trial involving 150 patients published last year, eight weeks of treatment with the three-herb combo, taken once daily, reduced OAB symptoms, incontinence, and the use of pads or adult diapers. At week 8, mean daytime urinary frequency was 7.7 episodes per day in the Urox-treated subgroup versus 11 per day in the placebo group. Episodes of nocturia were also reduced (2.2 versus 3.1 episodes per night). There were no significant adverse effects associated with the herbal combination (Schoendorfer, N et al. BMC Complement Altern Med. 2018; 18(1): 42).
Other botanicals also show promise in treating urinary disorders. Italian researchers observed a reduction of mixed UI and stress UI symptoms in a group of 42 female patients taking a multi-herb bladder supplement called IncontinenzaMEV, that contains astragalus, thyme, lavender, hops, equisetum, red clover, cypress, and agrimonia.
After two months of daily treatment, 30.9% of participants reported a slight improvement in symptoms, and another 11.9% were “much improved” after two months of treatment. Unlike the situation with anticholinergic drugs in this context, the treatment withdrawal rates were low among the women taking the herbal combo; the adverse events were negligible (Risi, O et al. Archivio Italiano Di Urologia E Andrologia. 2017; 89(4): 293-295).
Prorox, the Seipel Group’s “male” formula, expands on the Urox blend’s ingredient lineup with additional herbs and nutrients––saw palmetto, lycopene, vitamin D3, selenium and zinc––to support a healthy prostate and reduce symptoms of prostate gland enlargement. Patients can purchase the consumer-branded versions of both Prorox and Urox directly from the Seipel Group’s Australian website.
For clinicians, the company also offers UroxPro, a standardized practitioner-only version of Urox, intended for health professionals who address conditions like calcium or urate kidney stones (renal calculi), other renal health issues, interstitial (non-bacterial) cystitis, diabetes mellitus (for renal protection from degradation), as well as urinary incontinence, urgency, frequency and nocturia. In the US, physicians can currently obtain UroxPro only through distributor Emerson Ecologics. Search for “Seipel Group” or “UroxPro” on the company’s website.
But before any treatment decisions can be made, the first step is to make patients feel comfortable enough to disclose their bladder symptoms. Sepiel underscored the importance of educating patients about common urinary issues to raise awareness, reduce the stigma, and open the dialog about non-pharma treatment options.
END







