Keeping uric acid in check is good for the gut.
“People who suffer from chronic elevated uric acid tend to harbor unhealthy biomes,” says neurologist David Perlmutter, MD. In his latest book, Drop Acid: The Surprising New Science of Uric Acid, Perlmutter presents several studies showing that adverse changes in the gut microbiome directly relate to our ability to metabolize and eliminate uric acid (UA).
Understanding the intricate interplay between hyperuricemia and the gut microbiome is still a relatively new field of research. But it has already led to some interesting discoveries.
“Gout bacteria”
Scientists first documented the well-known relationship between high UA and conditions like gout and kidney stones long ago. More recently, investigators began identifying unique patterns of “bad” gut bacteria in patients with gout, kidney stones and kidney disease.
“We know that elevated uric acid favors pro-inflammatory types of bacteria in the gut,” Perlmutter told Holistic Primary Care. A “very characteristic type of dysbiosis” occurs, for instance, in patients with gout, an auto-inflammatory disease.
Gout is marked by disordered purine metabolism, which results in chronic hyperuricemia as well as microbiome changes. Some refer to the microbiomes of hyperuricemia patients as “gout bacteria.”
“We know that elevated uric acid favors pro-inflammatory types of bacteria in the gut. “A very characteristic type of dysbiosis” occurs in patients with gout.
David Perlmutter, MD
In a 2016 study, researchers compared the intestinal microbiota of healthy individuals and of gout patients. They identified 17 specific bacteria associated with gout. Using that data, they were able to predict diagnoses of gout with almost 90% accuracy, simply by analyzing gut microbes (Guo, Z et al. Scientific Reports. 2016; 6: 20602).
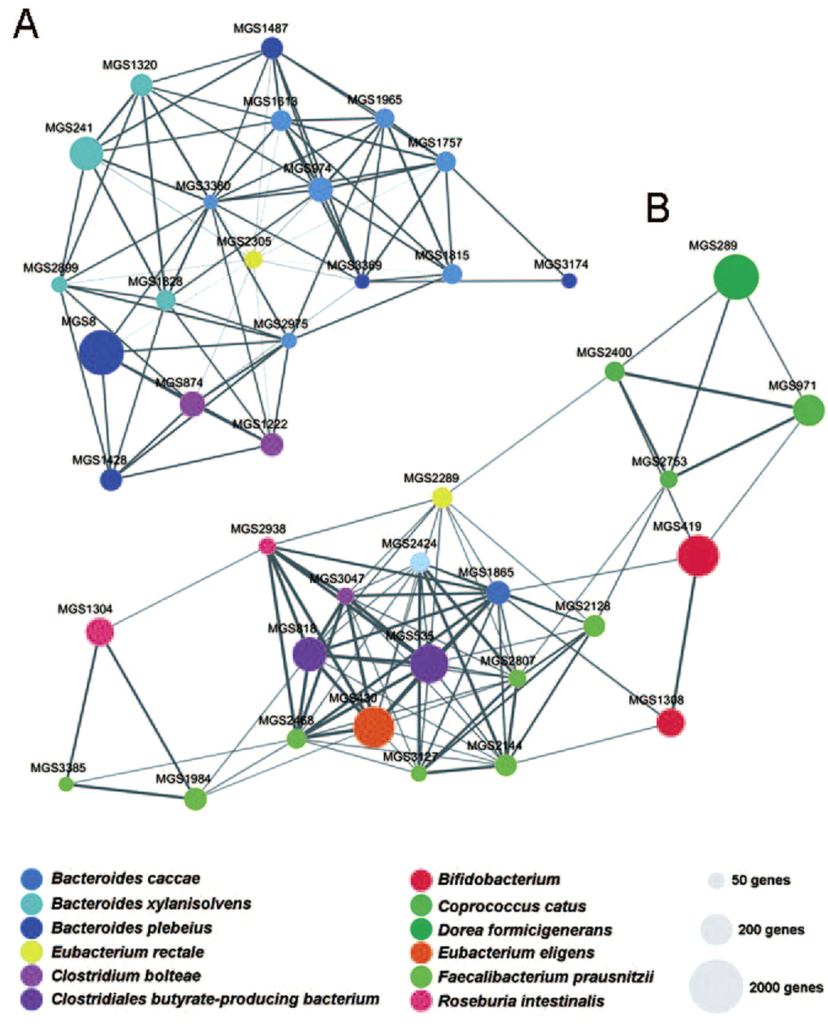
This team developed the Microbial Index of Gout (MiG) based on their findings. The gout microbiome closely resembled that of patients with type 2 diabetes or metabolic syndrome. Healthy individuals, on the other hand, showed a separate and distinct gut microbiome profile.
Guo and colleagues contend that their MiG model is more reliable than the typical UA blood tests physicians use to diagnose gout. They propose it as a novel non-invasive diagnostic tool for early detection.
UA in the Gut
So what does uric acid have to do with gut bacteria?
In healthy humans, around one third of all UA in is excreted through the gut. The rest is eliminated mainly via the kidneys. An over-accumulation of UA in the intestines can influence microbiome composition, encouraging the growth of pro-inflammatory strains.
Certain intestinal microbes play important roles in metabolizing both UA and purines. Organisms in the Escherichia coli group, for instance, can secrete xanthine dehydrogenase, an enzyme involved in purine breakdown. One of the natural byproducts of purine metabolism is uric acid.
Many common foods contain purines, including alcohol and some types of seafood and meat, all of which hyperuricemic patients should avoid, or at least minimize.
“We know that elevated UA is associated with increased gut permeability. And that’s really very important, because so much research has revealed relationships between intestinal permeability and various autoimmune and inflammatory conditions.”
David Perlmutter, MD
Other kinds of intestinal flora promote uric acid metabolism, improve its excretion, regulate UA absorption and secretion in the gut, and moderate intestinal inflammatory responses. A 2022 review indicates that beneficial bacteria like Bifidobacteria and Lactobacilli have UA-lowering effects that target the intestinal tract (Wang, J et al. Crit Rev Food Sci Nutr. 2022; 62(14): 3979-3989).
UA Linked to Leaky Gut
High UA damages the intestinal lining. This further “pav[es] the path toward systemic inflammation,” Perlmutter explains. Breaks in the intestinal wall allow food toxins and pathogens to exit the gut and enter the bloodstream. Once in the blood, those toxic elements can “[trigger] an aggressive and often prolonged immune response.”
“We know that elevated UA is associated with increased gut permeability. And that’s really very important, because so much research has revealed relationships between intestinal permeability and various autoimmune and inflammatory conditions.”
“Even in my field of neurology, we see strong relationships with gut permeability to things like Alzheimer’s, autism, depression, and even amyotrophic lateral sclerosis (ALS). It’s no wonder that researchers are now documenting a strong association between hyperuricemia, intestinal barrier dysfunction, and immune disorders,” he added.
While it’s clear that elevated UA induces changes in the microbiome, the reverse might also be true. “Changes in gut bacteria may be responsible for elevation of uric acid as well,” Perlmutter says, pointing to experiments on animals treated with antibiotics. The drugs induced changes in the animals’ gut bacteria that then lead to UA elevations.
Experiments in humans have explored fecal microbial transplants (FMT) as a treatment for both acute and recurrent gout. “FMT leads to a significant reduction of uric acid immediately after the treatment and decreases the frequency and duration of acute gout attacks.”
LUV Your Gut
According to Dr. Perlmutter, “there’s a lot you can do to nourish the health of your intestinal microbiome.” In Drop Acid, he presents the “LUV” (Lower Uric Values) Diet, designed in part to foster a healthy gut microbiota.

One of his top recommendations is to add prebiotic-rich foods to your plate. “Prebiotics are like fertilizer for your microbes, helping them grow and reproduce.”
Many prebiotic foods also inhibit xanthine oxidase, the enzyme required for making UA. This is the same enzyme targeted by allopurinol and febuxostat, the two main drugs for treating gout. Eating fresh fruits, vegetables, and whole grains that contain prebiotics provides the “double benefit” of encouraging good bacteria and tamping down UA production.
Fiber—especially inulin, found in many familiar vegetables like onions, leeks, artichokes, and asparagus—slows the release of sugars and cultivates a healthy microbiome. Inulin is not digested or absorbed. It instead acts as a prebiotic, remaining in the bowel and allowing certain beneficial bacteria to thrive. Because inulin has “long been found to enhance the composition of the gut bacteria,” it is abundant in the LUV Diet.
Probiotic-rich fermented foods including kimchi, kombucha tea, and cultured yogurt are also great for gut health. Probiotics decrease inflammation and improve metabolism of sugar and UA. For some people, probiotic supplementation may be appropriate as well.
Avoid Microbiome Disruptors
Sugar substitutes such as saccharin, sucralose, and aspartame can disrupt the microbiome in ways that favor dysbiosis, blood sugar imbalances, and an overall unhealthy metabolism. “It’s important to avoid anything that interferes with your body’s ability to break down and filter compounds and toxins, and that includes sugar substitutes,” Perlmutter cautions.
He also suggests reinforcing good gut bugs by avoiding foods that contain genetically modified organisms (GMOs) and eating organic whenever possible.
Ultimately, whatever path we take to get there, “the sooner we can drop acid to healthful levels and support the strength and function of our guts’ microbiomes, the sooner we can usher in better health,” Perlmutter urges.
END







