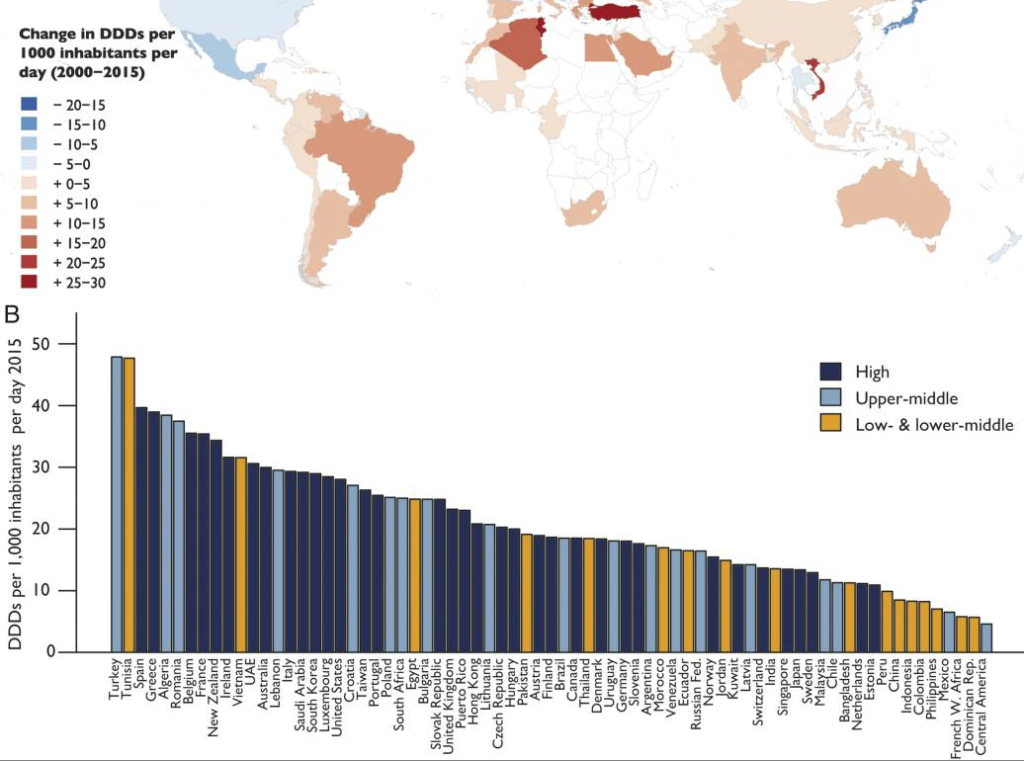
Globally, there are striking regional variations in per capita antibiotic consumption.
A 2018 study of prescription patterns in 31 European countries showed that Greece tops the list in Europe, at roughly 40 doses per 1,000 inhabitants per day (Klein E, et al. PNAS 2018). That’s a 4-fold difference from the Netherlands, where use is lowest.
Other high-prescribing nations include France, Belgium, Spain, and Romania. At the other end, Estonia, Sweden, Latvia and Norway are close to the Netherlands’ low prescription rates.
The variance does not reflect major differences in prevalence of serious bacterial infections that would require antibiotic therapy. Rather, “this reflects culture and practice habits,” says Martin J. Blaser, MD, director of the Rutgers University Center for Advanced Biotechnology and Medicine.
A multicenter analysis of 184,032 US outpatient visits revealed that 12.6% of those encounters resulted in an antibiotic prescription. Based on 2010-2011 data from the National Ambulatory Medical Care Survey, the annual antibiotic prescription rate in the US was 506 per 1,000 population. However, only 353 of those prescriptions (69.7%) were deemed medically appropriate (Fleming-Dutra KE, et al. JAMA. 2016).
Greece tops the list in Europe, at roughly 40 doses per 1,000 inhabitants per day. That’s a 4-fold difference from the Netherlands, where use is lowest. The variance does not reflect major differences in prevalence of infections that require antibiotic therapy.
In a 2015 paper, Gerber and colleagues at the University of Pennsylvania looked at antibiotic prescription rates at 25 pediatric practices associated with the Children’s Hospital of Pennsylvania. Of 399,798 acute visits, nearly 30% resulted in an antibiotic prescription.
After adjusting for patient age, sex, race, and Medicaid status, Gerber found that the highest prescribers wrote twice as many antibiotic prescriptions as the lowest. The rate ranged from 18% to 36%. Again, the differences were not attributable to differences in infectious diseases. (Gerber JS et al. J Pediatric Infect Dis. 2015.)
Medical organizations worldwide have urged physicians to be more judicious in prescribing antibiotics, but there’s little evidence that practitioners are heeding the message, or that patients understand the problem.
Though the US has a fairly high rate of antibiotic use, it is by no means at the top of the global list. In some developing countries, like Pakistan and Bangladesh, the average child has more than 10 courses in the first few years of life. Worried parents routinely go to local pharmacies that freely sell antibiotics, often to treat conditions which might not actually have bacterial etiologies.
For well over a decade, medical organizations worldwide have urged physicians to be more judicious in prescribing antibiotics, but there’s little evidence that practitioners are heeding the message, or that patients understand the problem.
Back in 2014, the CDC’s National Action Plan for Combatting Antibiotic-Resistant Bacteria established the goal of reducing “inappropriate outpatient antibiotic use” by 50% by 2020. One year past the deadline, the US is still far from that objective. The situation is even worse in many other countries.
“We all need to prescribe them less often, especially in children, when the indication and the necessity are minimal,” Dr. Blaser said.
END







