 The surge of microbiome research over the last decade is reshaping much of what we thought we knew about human biology. Nowhere is this more true than in the emerging discoveries about how the microbiome—or substances produced by it—affect estrogen metabolism.
The surge of microbiome research over the last decade is reshaping much of what we thought we knew about human biology. Nowhere is this more true than in the emerging discoveries about how the microbiome—or substances produced by it—affect estrogen metabolism.
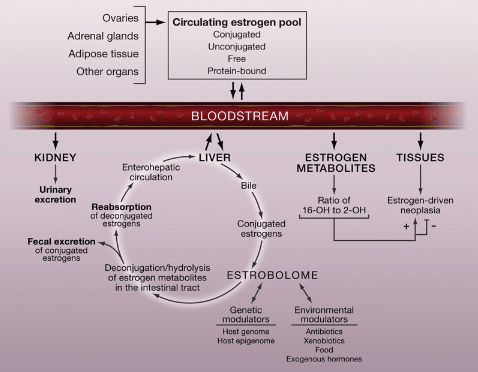
The “Estrobolome” –representing the aggregate of enteric bacterial genes whose products are capable of metabolizing estrogens—is a major influence on a woman’s lifetime exposure to circulating estrogens (Plottel CS, et al. Cell Host Microbe. 2011: 10 (4): 324-335). It also, therefore, affects a woman’s risk of developing estrogen-driven cancers.
Specific nutraceuticals, probiotics and botanicals can be used to promote a healthy and protective microbiome that favors estrogen conjugation and excretion. This, in turn, reduces the likelihood of oncogenesis, tumor progression, and recurrence.
Dysbiosis & Estrogen Metabolism
Dysbiosis, a disruption in the healthy ecology of the microbiome, may promote deconjugation and recycling of estrogens via the entero-hepatic circulation, increasing a woman’s estrogenic exposure and contributing to increased risk of breast cancer and other estrogen-driven cancers. Dysbiosis also causes local and distant increases in inflammation and inflammatory cytokines, a hallmark of cancer (Belkaid Y, Hand T. Cell. 2014; 157(1): 121–141. Shapira I, et al. ISRN Oncol. 2013)
Normally, circulating estrogens are metabolized and conjugated in the liver via glucuronidation resulting in glucuronides, which do not bind to estrogen receptors. Estrogens conjugated with glucuronic acid are more hydrophilic, allowing for excretion via bile or urine. Glucuronides (conjugated estrogens) are primarily excreted from the liver into the bile and then later out of the body in the stool. A small amount is excreted in the urine.
The gut microbiome modulates estrogen metabolism and affects the proportion of re-circulated versus excreted estrogen and estrogen metabolites.
Some gut bacteria produce the beta-glucuronidase enzyme that leads to deconjugation of glucuronic acid from estrogen, in effect reversing the normal hepatic detoxification process. Beta-glucuronidase (BG) is produced in increased amounts with a dysbiotic intestinal ecology. The more BG that gets produced, the less estrogen excreted and the more it is recirculated.
That’s because the bacterial BG leads to the deconjugation of estrogen metabolites in the intestinal tract. These deconjugated estrogens are now eligible for re-uptake and recirculation via enterohepatic circulation. Deconjugation may result in greater reabsorption of free estrogens, increasing the risk of estrogen-driven cancers such as breast, ovarian, and endometrial cancers (Plotnikoff GA. Glob Adv Health Med. 2014; (3):33-43).
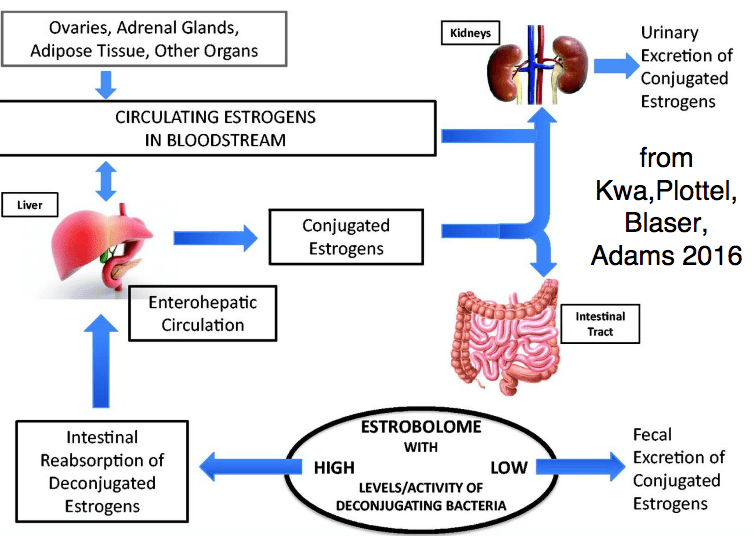
In the presence of elevated circulating estrogens, Sex Hormone Binding Globulin (SHBG) also increases. Elevated SHBG is an established risk factor for breast cancer.
Goedert et al demonstrated that b -glucuronidase is produced in increased amounts by dysbiotic intestinal ecology. In post-menopausal women newly diagnosed with ER+ breast cancer there is a less diverse fecal microbiome. Fecal b -glucuronidase is inversely correlated with fecal total estrogens, both conjugated and unconjugated.
The good news is that the deconjugation, or reversal of liver detoxification caused by increased microbial production of BGis a modifiable risk factor.
Reduction in the population of Clostridium and Bacterioides bacteria and increases in Lactobacillus and Bifidobacteria species enhances fecal excretion of conjugated estrogens and decreases in urinary estrogens. (Plottel CS, Blaser MJ. Cell Host & Microbe. 2011: 10 (4): 324-335, Paul B, et al. Clin Epigenetics. 2015 7 (112)).
But there’s more to the story than just b -glucuronidase. It appears that intestinal microbial richness itself has influence on the levels of non-ovarian estrogens in the enterohepatic re-circulation. (Goedert JJ, et al. J Natl Cancer Inst; 2015 107(8)).
Dietary, the Microbiome, and Estrogen
The diet has a profound and highly dynamic impact on the composition and function of the microbiota. Multi-directional interaction exists between a woman’s diet, her immune system, and the commensal microflora living in her GI tract. The immune system is not only controlled by its symbiotic relationship with the microbiota, it is also exquisitely sensitive to the nutritional status of the host.
Microbial BG production is increased in women who eat high fat, high protein diets and it is decreased with diets high in fiber. Simply put, diets high in animal proteins increase BG while plant based vegetarian diets low in animal protein contribute to lower levels of intestinal beta glucuronidase. This is one reason why researchers have consistently observed lower incidence of breast cancer among women who are vegetarians.
Vegetarian diets are associated with reduced concentrations of Clostridial cluster XIVa bacteria which produce BG. Changing to a raw vegan diet from standard American meat-rich diet rapidly and significantly reduces BG activity. The difference can be striking.
Vegetarian women excrete 2 to 3 times more estrogen in feces than do omnivores. Omnivores have about 50% higher mean plasma level of unconjugated estrone and estradiol than vegetarians.
In vegetarians, a greater amount of the biliary estrogen escapes reabsorption and gets excreted with the feces (Harmon B. Public Health Nutr. 2014; 17(9): 2087-2093. Fuhrman BJ, et al. J Clin Endocrinol Metab. 2014; 99(12): 4632-4640,
Add Fiber, Reduce Risk
Dietary plant fibers may be classified as insoluble or soluble. Insoluble Fiber which does not dissolve in water is not a substrate or fuel for enteric microbiota. Soluble Fiber does dissolve in water and is substrate and fuel for enteric microbiota.
A meta-analysis of large prospective cohort studies representing 16,848 subjects showed that:
- High dietary fiber intake is a protective factor for breast cancer (RR = = 0.89; 95% CI: 0.83–0.96) compared with low intake.
- Every 10-gram per day incremental increase in dietary fiber intake was associated with a 7% reduction in risk of breast cancer.
- High fecal fiber inhibits absorption of estrogens in the gut, reducing the total body pool of estrogen
- Binding of unconjugated estrogens to fiber in the gut decreases estrogen reabsorption (Kotepui M, et al. Contemp Oncol (Pozn). 2016; 20(1): 13-19).
Nutrition Strategies to Lower BG
Traditional Cultured or Fermented Foods: Sauerkraut, Kim Chee, Cultured Olives, Cultured Goat’s and Sheep’s Milk Yoghurt or Kefir, Kombucha, Kanji, and Beet Kvass.
Prebiotic Foods: All of the following foods are high in soluble fiber and fructo-oligosaccharides, which promote the growth of beneficial bacteria: chicory, asparagus, banana, Jerusalem artichokes,  garlic, onions, leeks, shallots, beetroot, fennel, peas, cruciferous vegetables, nuts and seeds.
garlic, onions, leeks, shallots, beetroot, fennel, peas, cruciferous vegetables, nuts and seeds.
Prebiotic Supplements: Fructo-Oligosaccharides, Inulin, Acacia, and Psyllium
Probiotic Supplements: Certain probiotics can be helpful for decreasing bacteria that produce b-glucuronidase. Lactobacillus and Bifidobacteria are especially helpful, particularly the Lactobacillus plantarum and Lactobacillus GG strains.
Plant Polyphenols & the Estrobolome
Dietary polyphenols and their metabolites modulate gut microbial balance by stimulating growth of beneficial bacteria such as Lactobacillus and Bifidobacterium, while simultaneously inhibiting pathogenic bacteria.
But it is a bi-directional interaction, because polyphenols also depend upon gut microbiota for their transformation to the active metabolites that play a role in regulating inflammation, carcinogenesis, apoptosis, cell proliferation and modulation of enzymes (Chen F, et al. J Ethnopharmacol. 2016; 179: 253-64. Ozdal T, et al. Nutrients. 2016; 8(2): 78).
Black Currant Fruit Concentrate or Powder significantly increases Lactobacilli and Bifidobacteria, while decreasing Clostridium and Bacterioides, leading to a decrease in the activity of β-glucuronidase (Molan AL, et al. Phytother Res. 2014: 228(3): 416-22).
Culinary Spices: Spices play a role in regulation of intestinal microbiota and enhancement of gastrointestinal health. Oregano, black pepper, cayenne pepper and ginger possess prebiotic‐like effects that promote growth of beneficial bacteria and suppress pathogenic bacteria. Black pepper, cayenne pepper, cinnamon, ginger, oregano, rosemary, and turmeric promote the growth of Bifidobacterium and Lactobacillus (Lu QY, et al. J Food Sci. 2017: 82(8): 1807-1813)
Curcumin (Turmeric): Curcuminoids are degraded to their active metabolites by human fecal microbes. Curcumin promotes a healthy and diverse microbiome, which secondarily increases the bioavailability of many other phytochemicals (McFadden RM, et al. Inflamm Bowel Dis. 2015P 21(11): 2483-94; Shen L, Crit Rev Food Sci Nutr. 2018 [Epub ahead of print])
Scutellaria baicalensis: Known in Chinese medicine as Hang Qin root, Scutellaria is rich in the polyphenol called baicalin, a BG Inhibitor. It is a common constituent of modern Chinese botanical formulas for tumor control, reduction of inflammation, and infection control (Narita M, et al. Xenobiotica. 1993: 23(1): 5-10. Li-Weber M. Cancer Treat Rev. 2009: 35(1): 57-68).
Helpful Nutraceuticals
Several readily accessible and inexpensive vitamins and nutraceuticals can also be helpful in positively affecting the estrobolome to lower lifetime estrogen exposure and reduce cancer risk. These include:
Vitamin A (Retinoic Acid). Vitamin A is required for the induction of protective immunity, and it also influences the composition of the microbiome. In the intestines, retinoic acid contributes to the specialization of mucosal dendritic cells, which are an integral part of local gut immunity (Hibberd MC. Sci Transl Med. 2017; 9(390).
Vitamin D3: Supplementation with vitamin D changes the microbiome in the upper GI tract(gastric corpus, antrum, and duodenum) resulting in a reduction in opportunistic pathogens and an increase in bacterial richness (Bashir M, et al. Eur J Nutr. 2016: 55: 1479-1489)
Omega-3 Fatty Acids (EPA-DHA): Omega-3s promote significant changes in the gut microbiota associated with health. Specifically, they promote the increase of butyrate-producing bacteria. EPA also results in the enrichment of Lactobacillus species (Costantini L, et al. Int J Mol Sci. 2017; 18(12): 2645)
The key point in all of this is that a woman’s lifetime burden of estrogen exposure may reflect the metabolic function of her Estrobolome, the aggregate of enteric bacteria that metabolize estrogens.
A healthy Estrobolome favors estrogen conjugation and excretion. But with overgrowth of bacteria that produce b -glucuronidase, there is an increased deconjugation of estrogen, followed by enterohepatic recirculation of estrogens, thus increasing a woman’s lifetime exposure. Higher lifetime estrogen exposure is correlated with increased risk of several common forms of cancer in women.
Fortunately, the composition of the Estrobolome and the activity of b -glucuronidase can be modulated by dietary factors, prebiotic soluble fibers, culinary herbs and spices, and targeted use of specific phytochemicals and nutraceuticals.
By paying greater clinical attention to nurturing a healthy Estrobolome, we can go a long way in helping our patients reduce their risk estrogen-driven cancers.
To learn more about how to support people with cancer or elevated cancer risk, visit: American Institute of Integrative Oncology (www.aiiore.com).
Nalini Chilkov, LAc, OMD is a seasoned clinician and innovator, building bridges between modern and traditional healing paradigms and partnering with physicians to achieve the best outcomes for patients. She is formally trained in acupuncture and oriental medicine and specializes in the integrative care of people with cancer and other serious chronic illnesses. She is the author of “32 Ways to Outsmart Cancer,” and founder of the American Institute of Integrative Oncology. She practices in Santa Monica, CA







