 Vitamin C supplementation can improve glycemic and insulin regulation in some high-risk patient subgroups groups, according to researchers at Newcastle University’s Human Nutrition Research Centre in the UK
Vitamin C supplementation can improve glycemic and insulin regulation in some high-risk patient subgroups groups, according to researchers at Newcastle University’s Human Nutrition Research Centre in the UK
The Newcastle researchers conducted a systematic review and meta-analysis of randomized controlled trials examining the effects of vitamin C on glucose, hemoglobin A1C (HbA1c), and insulin concentrations. Their review covered 22 eligible studies looking at the effects of vitamin C on a total of 937 adult participants (Ashor, A. et al. Euro J Clin Nut. 2017; 71(12): 1371–1380).
They found that patients with diabetes, older individuals, and those who supplement longer-term are most likely to experience meaningful health benefits from the supplement.
Studies of the vitamin’s impact on different biomarkers of glycemic and insulin regulation have generated contrasting results. In their meta-analysis, the Newcastle team found that while overall, vitamin C did not significantly modify glucose, HbA1c, or insulin in healthy populations, it very definitely did improve glucose metabolism in a few key specific subgroups.
Benefits for Diabetics, Elders
Across the studies reviewed, they found greater reductions in glucose levels among subjects with diabetes, in older individuals, and among those who regularly took the vitamin for prolonged periods.
Subgroup analyses showed that supplementing with vitamin C significantly lowered glucose levels (−0.44 mmol/l, 95% CI: −0.81, −0.07, P=0.01) in participants with type 2 diabetes. Additionally, it appeared to have stronger effects on patients’ fasting insulin levels (−13.63 pmol/l, 95% CI: −22.73, −4.54, P<0.01) versus postprandial insulin concentrations.
The Newcastle group also found that vitamin C significantly reduced glucose concentrations when the duration of the supplementation intervention was greater than 30 days (−0.53%, 95% CI: −0.79, −0.10, P=0.02), suggesting that longer-term supplementation could be necessary to achieve meaningful health benefits.
Meta-regression analyses indicated that age was another important factor determining the vitamin’s effects on insulin concentration, with more positive outcomes observed in older participants. The effect size was further associated with participants’ baseline body mass index and plasma glucose levels, as well as the duration of supplementation.
Significant Risk Reductions
Other recent studies exploring antioxidant vitamin supplementation do highlight a potential role for vitamin C in diabetes treatment.
One small clinical trial investigated the influence of antioxidants vitamin C and E on the efficacy of metformin in a group of 40 adult males with type 2 diabetes (T2DM). “Recently, there has been an increasing interest in the influence of antioxidant vitamins on the efficacy of oral hypoglycemic therapy in type 2 diabetic patients,” the study’s authors write.
Patients who took vitamin C and/or E for 90 days showed improvements on a number of biomarkers for diabetes, including fasting blood sugar, HbA1c, lipid profile and insulin concentrations, when compared with diabetic patients receiving placebo only (El-Aal, AA. et al. Diabetes Metab Syndr. 2018; 12(4): 483-489).
An earlier 12-month randomized controlled trial showed that treating T2DM patients with both metformin and vitamin C was more effective at 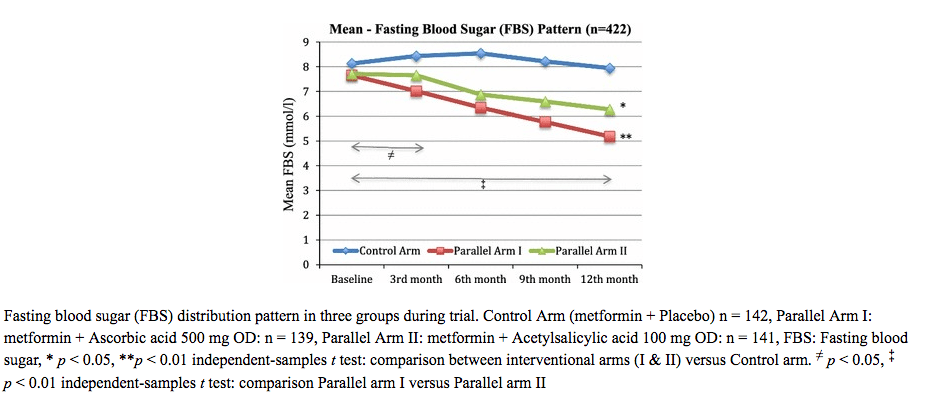 reducing HbA1c and risk factors for long-term diabetes-related complications than metformin alone. This study involved 452 patients, randomized to three parallel arms: one took metformin alone; the second took metformin plus vitamin C (500 mg ascorbic acid); the third got metformin plus aspirin (100 mg salicylic acid). In all groups, the mean age was roughly 38 years.
reducing HbA1c and risk factors for long-term diabetes-related complications than metformin alone. This study involved 452 patients, randomized to three parallel arms: one took metformin alone; the second took metformin plus vitamin C (500 mg ascorbic acid); the third got metformin plus aspirin (100 mg salicylic acid). In all groups, the mean age was roughly 38 years.
Patients treated with metformin and a vitamin C supplement over the course of one year showed marked reductions in fasting blood glucose compared with those on metformin alone. On average, there was a 3 mmol/l difference in the glucose levels between the two groups. Those taking the metformin-aspirin combination also showed lower fasting glucose levels compared with those on metformin alone, but the difference was not as great.
There was a similar pattern with HbA1c: the patients taking the vitamin C were twice as likely to show reduced HbA1c than patients taking metformin alone (OR 2.31 (95% CI 1.87-4.42) p < 0.001). On this parameter, both ascorbic acid and aspirin produced similar reductions.
Treating patients with the metformin/vitamin C combination also significantly reduced risk factors contributing to long-term diabetes complications (Gillani, SW. et al. Cardiovasc Diabetol. 2017; 16(1): 103).
“This trial showed significant reduction in fasting blood sugar, HbA1c, diabetes related long-term complications, LDL-c, TG, Total cholesterol, also Framingham score for 10-years risk of developing CVD with ascorbic acid group compared to control group,” wrote the authors, who represented an international team of researchers based in Saudi Arabia, Malaysia, the Philippines, Pakistan, and Dubai.
With diabetes on the rise globally, there is a glaring need for novel strategies that can help people regulate their glucose and insulin levels, and maintain their health.
While the Newcastle authors encourage a cautious interpretation of their metanalysis, owing to the limitations inherent in the primary studies, they nevertheless conclude that “personalised interventions with vitamin C may represent a feasible future strategy” to enhance treatment benefits and efficacy.
The data from the Gillani and El-Aal studies certainly support that conclusion.
END







