Thorough, restful sleep is a physiological necessity and an essential factor for overall health. Yet for many Americans, good sleep has become a rare luxury.
Long working hours, economic woes, interpersonal stress, discordant schedules, poor diet, aging, and medication side effects are contributing to an epidemic of sleeplessness that has dire personal and public health consequences.
Consider these statistics:
• According to the National Center on Sleep Disorders Research at the National Institutes of Health, 30-40% of US adults say they have some symptoms of insomnia; 10-15% have chronic insomnia.
• National Sleep Foundation (NSF) polls dating back to 1999 consistently show that over 50% of American adults experience problems with sleep at least a few nights a week.
• In a 2005 public poll by NSF, 38% of Americans report that they often wake up feeling unrefreshed; 32% wake frequently during the night; 21% wake too early and are unable to get back to sleep.
• A 2008 Centers for Disease Control report indicated that 70% of adults say they obtain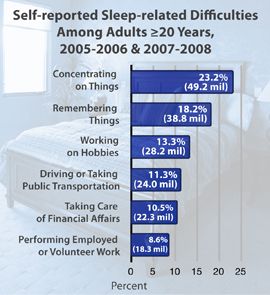 insufficient rest at least once each month, and 11% report insufficient sleep or rest every day.
insufficient rest at least once each month, and 11% report insufficient sleep or rest every day.
• NSF’s 2008 Sleep in America poll showed that 36% of Americans reported driving drowsy or falling asleep while driving; 29% regularly fall asleep or become very sleepy at work; 14% miss family events, work functions, and leisure activities due to sleepiness.
• Roughly 15% of the general population is affected by sleep-disordered breathing, including obstructive sleep apnea; many do not fit the “textbook” apnea profile (ie, middle-aged, overweight, white male)
• Narcolepsy/cataplexy and other forms of hypersomnia affect 1 in 2,000 people. Restless legs syndrome affects more than 1 in 20.
• There were 66 million prescriptions for hypnotics and sedatives in 2010, up from 52.3 million in 2006, according to a recent report by IMS Health’s Institute for Health Informatics.
• Insomnia costs the average US worker 11.3 days, or $2,280, in lost productivity each year, according to a 2011 report from the American Academy of Sleep Medicine. For the nation, insomnia carries a total price tag of $63.2 billion per year.
A Major Public Health Issue
In multiple studies in the US and abroad, disordered sleep has been associated with significantly increased risk of obesity, diabetes, hypertension, cardiovascular events, stroke, depression, substance abuse, and all-cause mortality (Institute of Medicine. Sleep Disorders and Sleep Deprivation: An Unmet Public Health Problem. Washington, DC: The National Academies Press; 2006). Disordered sleep may be a contributing factor in breast, colorectal and prostate cancer, as well as obesity, diabetes, and various gastrointestinal disorders.
All of these risks are on top of the impaired cognitive function, irritability, poor work or school performance, memory lapses and other psychosocial consequences of sleeplessness.
The impact of sleep disorders is not lost on the nation’s public health institutions. Earlier this year, the Department of Health and Human Services declared sleep disorders a high-priority for basic and clinical research, and urged the National Center on Sleep Disorders (NCSD) within the National Heart, Lung & Blood Institute (NHLBI) to redouble its efforts.
To that end, the NCSD issued a comprehensive research agenda focused on five core goals:
• Advance the understanding of sleep and circadian functions and mechanisms, in both the brain and the body, across the lifespan.
• Identify genetic, pathophysiological, environmental, cultural, lifestyle and gender differences that contribute to sleep/circadian disorders.
• Improve prevention, diagnosis, and treatment of sleep and circadian disorders, chronic sleep deficiency, and circadian disruption.
• Enhance the translation and dissemination of sleep and circadian research in ways that improve health care and enhance human health.
• Increase sleep and circadian research training across scientific & clinical disciplines, accelerate the pace of discovery, and translate enhanced therapies from bench to bedside to community.
Sleep Stages & Sleep Architecture
Sleep disorders are far more varied and complex than simply the inability to fall asleep. Consequently, they require more than a quickly jotted prescription for a sedative drug. In fact, long term use of sedatives and hypnotics can ultimately exacerbate sleep problems as they adversely affect progression from one sleep phase to another: the drugs may induce sleep but they do not promote fully restorative sleep.
 The stages of sleep were first described more than 70 years ago by Alfred Lee Loomis, a pioneer of electroencephalography. Loomis defined five distinct stages, labeled A-E, based on the EEG wave patterns he observed. In the 1950s, Dement & Kleitman recognized that the rapid eye movement (REM) stage was unique and distinct from the other non-REM stages.
The stages of sleep were first described more than 70 years ago by Alfred Lee Loomis, a pioneer of electroencephalography. Loomis defined five distinct stages, labeled A-E, based on the EEG wave patterns he observed. In the 1950s, Dement & Kleitman recognized that the rapid eye movement (REM) stage was unique and distinct from the other non-REM stages.
In the late 1960s, building on this earlier work, Rechtschaffen & Kales developed a schema which divided non-REM sleep into four stages, with Stage 1 being the state between ordinary wakefulness and sleep; Stage 2 being light sleep; and Stages 3 and 4 classified as “deep” (slow wave) sleep. The Rechtschaffen & Kales classification held sway for almost 40 years.
In 2007, the American Academy of Sleep Medicine published the first major revision to this staging system by combining the “classic” Stages 3 and 4 into a single stage (The AASM Manual for the Scoring of Sleep and Associated Events). In practice, many clinicians and researchers still consider the two slow-wave phases as distinct. In Stage 3, less than 50% of total wave patterns are delta waves—the slowest frequency EEG waves, characteristic of the deepest sleep; in Stage 4, delta waves equal 50% or more of all waves.
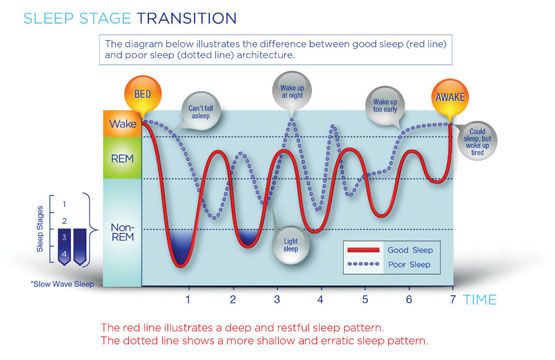
Generally, the course of a night’s sleep follows a pattern of alternating non-REM and REM phases, with the first REM phase occurring within 90 minutes of falling asleep. During REM blood flow to the brain increases by 50%-200%. This is when dreaming occurs, and it enables the brain to regenerate its own energy.
Typically, after initially falling asleep, an individual will pass through non-REM stages before entering the first period of REM sleep. Sleep researchers term this initial transition period the “latency to REM sleep.”
After this, the sleeper typically moves through non-REM Stages 1 and 2, and into Stages 3 and 4, characterized by high-amplitude, slow frequency delta wave activity. The course of a night’s sleep follows a parabolic curve of repeating “ascents” through the non-REM stages, into REM periods, and “descents” back into deep sleep.
The cycle speeds up toward morning, with more time spent in REM and Stages 1-2, and less in Stage 3-4 sleep. In a healthy sleep, roughly 25% of total sleep time is spent in REM activity, and 75% in non-REM phases.
Sleep Phases & Endocrine Function
What regulates the shift from one phase of sleep to another? There are many theories and likely many different factors. The truth is, researchers have not yet identified the precise neural pathways and neurotransmitters that regulate these transitions.
According to sleep scientist Dr. Makoto Bannai, of the Institute for Innovation, Ajinomoto Co., Inc., Kanagawa, Japan, this is a subject of great interest. “Nobody really knows which specific part of the brain regulates these transitions. However, the ventrolateral preoptic area (VLPO) is one of the regions that seems to be very important for non-REM sleep.”
Sleep–especially deep sleep—is far from being a metabolically passive state. Quite the opposite is true: sleep is characterized by heightened anabolic activity and tissue repair in all major organ systems. A host of hormonal and metabolic cascades take place during the various phases of sleep.
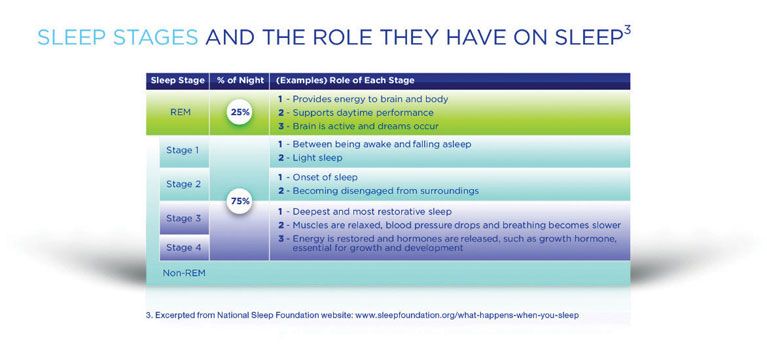

Growth hormone, essential for tissue repair, is released during a sleeper’s first pass through Stage 3-4 sleep. University of Chicago researchers showed that men who spent the longest amount of time per night in slow-wave sleep (average of 24% of total sleep time) had significantly higher growth hormone secretion than those who spent the lowest amount of time (9% of total sleep time) in slow-wave sleep stages (Van Cauter E, et al. JAMA 2000. 284(7): 861-8).
Prolactin release is also associated with onset of Stage 3-4 sleep. Follicle stimulating hormone and luteinizing hormone, which regulate maturational and reproductive processes, are also released during sleep but are not as closely correlated with specific sleep stages as growth hormone (Rubin R, et al. Psychosomatic Medicine. 1973; 35:4). Cortisol and thyroid-stimulating hormone, on the other hand, are released during theta-wave stages of sleep.
Sleep—or lack thereof—also affects ghrelin and leptin levels, which have profound influence on appetite. Lack of sleep or poor quality sleep tend to increase ghrelin production, leading to heightened appetite—particularly for high-carb and high-calorie foods; leptin levels decline, leading to a diminished sense of satiety. The result? A tendency toward overeating and weight gain.
The entire endocrine system is involved in and affected by sleep. This is why sleep problems are so often associated with endocrine and metabolic disorders. Simply put, when people don’t get enough slow wave non-REM sleep, they are more prone to metabolic dysregulation, weight gain, and cardiovascular risk.
Slow Wave Deficiency
For many people, the problem is not in falling asleep but in entering into or staying in the deep sleep stages that are most important for tissue restoration and metabolic balance. These patients are not the ones who lay awake all night wishing they could fall asleep, so they may not state that they have insomnia when you’re taking their history. But they do in effect have a serious sleep disorder because the deficiency of deep sleep can result in intense fatigue, and also increase the risk of cardiometabolic disease.
Make it a routine to ask patients when was the last time they woke up feeling truly refreshed. Many will tell you that they cannot remember, or that it has been years. Though they have no trouble falling asleep or staying asleep, some people seldom wake up feeling rested. This indicates inadequate slow wave sleep.
Many people wake up repeatedly through the night. Sometimes this is due to a physical issue (ie, apnea, nocturia), but in many cases it is a dysregulation in sleep cycling itself. Again, this fragmented sleep architecture can be extremely debilitating as well as frustrating.
It is important to make these distinctions, because a treatment that helps induce sleep will not necessarily benefit someone who has problems entering into deep sleep stages, or who wakes up repeatedly. In fact, it may cause further harm.
Limitations of Drug-Based Treatments
Many prescription sleep medications are good for inducing sleep, but they impair deep sleep, which is why patients on these drugs tend not to wake rested, though they reliably fall asleep after taking their meds.
Benzodiazepines attach to specific GABA receptors and induce Stage 1-2 non-REM sleep; however they block the transition to the deepest stages of sleep. Patients taking benzodiazepines may end up perpetuating their fatigue, though the drugs do cause them to fall asleep. Many people taking these drugs experience daytime sleepiness and impaired cognitive function, a consequence of the impairment of slow wave sleep.
Ambien (zolpidem), also popular for sleep induction, attaches to a smaller subset of GABA receptors than benzodiazepines, and causes less impairment of deep sleep. In principal, it should be a better choice. But patients using zolpidem often require escalating dosages over time. It can be very difficult to get off this drug, which can interfere with appetite and libido.
Lunesta (eszopiclone) has the longest follow-up data (12 months) of any sleep drug, and it is generally safe and effective. However, it can cause significant taste-disturbances (metallic taste in the mouth) that many patients don’t like. Some clinicians find that if patients stop taking Lunesta, sleep problems rebound and are worse than prior to starting the drug.
Rozerem (ramelteon) is a newcomer to the sleep drug line-up. It binds to melatonin receptors, and induces sleep quickly. It’s manufacturer claims it is non-addictive and non-habit-forming. However, it can induce apnea, so it should not be used in patients at risk. It can also raise prolactin, and interfere with normal hormone cycling. There is no evidence that Rozerem is any more effective than melatonin itself, which can be bought without prescription at a fraction of the cost.
Natural Therapies for Sleep
Some patients who have trouble sleeping will try alcoholic drinks as a means of inducing sleep. This is generally a bad idea. Though alcohol will cause people to fall asleep, there is often a rebound effect later in the night, resulting in highly fragmented sleep architecture. Alcohol also reduces REM sleep, so the brain does not get properly recharged.
Many people want “natural” non-pharmaceutical sleep aids, and there are a number of options available including herbs like valerian, chamomile and kava, as well as nutraceuticals like tryptophan and its metabolites, 5-HTP and melatonin (see Nutritional Treatments for Insomnia).
Melatonin has become popular in the US over the last decade. A naturally-occurring hormone, it is normally released at night by the pineal gland to induce and maintain sleep by blocking excitatory neurotransmitters. Many people take melatonin supplements to induce sleep and “reset” chronobiological rhythms. In clinical studies of insomnia, melatonin has given mixed results.
According to a 2004 research review from the Agency for Healthcare Research and Quality (AHRQ), melatonin can reduce sleep onset latency (time to falling asleep) in people with primary sleep disorders and increases sleep efficiency in those with secondary sleep disorders. Importantly, it does not reduce waking after sleep onset.
Glycine: A New Drug-Free Option
Glycine, a naturally-occurring non-essential amino acid, is a new addition to the spectrum of non-pharmaceutical options for people with disordered sleep, especially those prone to waking up in the middle of the night. In high concentrations, it promotes the prolongation of stage 3-4 sleep in the first sleep cycle and prevents sleep fragmentation, without sedative or hypnotic effects.
Japanese scientists have been at the forefront of glycine research, and a specially formulated product has been very popular in Japan. Ajinomoto North America, Inc., recently introduced a dietary supplement product in the US, as a nutraceutical non-prescription sleep aid available only through physicians.
The product, called Glysom, does not induce sleep like Ambien or benzodiazepines, nor does it induce daytime sleepiness as does melatonin. Rather it reduces core body temperature, which reduces fragmentation of sleep architecture, and promotes longer periods spent in deep slow-wave sleep during the early parts of the sleep curve.
When someone is hot, he or she tends to run through sleep cycles more rapidly and more frequently than when someone is cool (There’s wisdom in the old folklore that it’s wise to sleep with the windows open!). Glycine reliably produces this core temperature change in a way that promotes better sleep quality. It won’t necessarily get someone to sleep faster, but it will enable him to enter into and stay in the restorative deep sleep phases for longer periods.
Ajinomoto’s Dr. Bannai, who has been involved in several glycine studies, said that this amino acid has an affinity for the suprachiasmatic nucleus (SCN), which is the brain’s master circadian switchboard. “By maintaining the low core body temperature during sleep, glycine increases sleep stability, and improves sleep quality. The sleep-restorative effects appear as a tertiary benefit.”
Glysom delivers a natural lemon-flavored glycine preparation as a powder in pre-measured “stick packs” that patients are best recommended to take directly into their mouths with water or simply mix it with water and drink shortly before bed. Each stick pack delivers the recommended 3g daily dose.
Dr. Bannai is part of a team that tested the 3 g glycine formulation in 11 otherwise healthy adults (8 women, 3 men) who had histories of unsatisfactory sleep (fatigue, not waking refreshed). They were randomized to treatment with glycine or a placebo powder (reduced malt sugar in a similar package) and evaluated over two consecutive nights and days.
The assessment included thorough interviews, subjective assessment of sleep (using the St. Mary’s Hospital Sleep Questionnaire) and polysomnography. Evaluations were repeated twice for each patient, with a week-long interval between assessments.
Compared with subjects taking the placebo, those taking glycine had more frequent segments of deep sleep, fewer episodes waking after sleep onset, and shortened time to first appearance of Stage 2 and Stage 3 non-REM sleep. The time of transition from non-REM to REM periods was not altered (Yamadera W, et al. Sleep and Biological Rhythms. 2007; 5: 126-131).
Greater Sleep Satisfaction
Glycine-treated subjects reached Stage 2 in a mean of approximately 10 min, compared with 25 min in the placebo group; they reached Stage 3-4 within 35 min versus 55 min. This translated subjectively into greater satisfaction with sleep, less trouble falling asleep, and better sleep “efficacy” (amount of total time-in-bed actually spent sleeping). Evaluation of daytime cognitive function showed that glycine reduced sleepiness, and improved performance on memory tasks.
The Yamadera study built on earlier work by Inagawa who reported on the effect of bedtime ingestion of 3 g glycine in 15 women (aged 24-53 years). All had histories of sleep problems, and scores of 6 or greater on the Pittsburgh Sleep Quality Index. In this protocol, subjects took glycine one hour before bed on Monday-Thursday night, then took nothing on Friday-Sunday. The following week they were given a similarly flavored & colored placebo.
Assessment of sleep quality and daytime fatigue showed a consistent pattern of improved energy, greater sense of waking refreshed, and clear-headedness when subjects were taking glycine There were no changes in sleep time, suggesting that the observed benefits reflected better sleep quality. This study did not include polysomnographic evaluation (Inagawa K, et al. Sleep and Biological Rhythms. 2006; 4: 75-77: 20-32).
The development of Glysom is the latest indicator of Ajinomoto’s commitment the production of research-based nutritional ingredients, and a reflection of the company’s core competency in amino acid science. Established in 1909, Ajinomoto has set the global standards in amino acid production, and currently holds the biggest global market share of amino acids used in clinical applications.
Glycine is found naturally in beef, poultry, fish and seafood. The amount in a nightly dose of Glysom is equivalent to that of 10 large sea scallops or shrimps. Though glycine can be absorbed from food, it would be difficult on an ordinary diet to absorb enough to saturate the blood. At saturation levels, glycine readily crosses the blood brain barrier via passive diffusion. A supplemental dose of 3 g before bed readily accomplishes this.
There were no adverse effects associated with ingestion of supplemental glycine in either of the two clinical studies. Inagawa’s team published a study of 12 healthy volunteers who took as much as 9 g/day (thrice the recommended Glysom dose). There were no serious adverse effects, the most significant being soft stools and minor abdominal pain. Moreover, there was no daytime sleepiness or grogginess (Inagawa K, et al. Seikatsu Eisei Journal of Urban Living & Health Association. 2006; 50 (1).
A study by US researchers showed no adverse effects from glycine doses as high as 30 g/day (Garlick PJ. J Nutr. 2004; 134: 1633S-1639S).
Because it has an entirely distinct mechanism of action, glycine is not likely to interfere with other sleep aids. According to Dr. Bannai, there may even be some synergies. “If the mechanisms of other products to improve sleep are different from those of glycine, the simultaneous intake should be good for sleep. Since glycine has a unique mechanism, simultaneous intake with the other sleep supplement should work.”







