It is hard to remember that there was once a time when the medical community had to be convinced that Helicobacter pylori played a role in causing peptic ulcers. Over the last 3 decades, eradication of this organism has become almost a second-nature reflex on the part of most doctors.
Recently, however, some researchers have begun to question the wisdom of reflexively killing off this organism, which is one of the most widely prevalent microbes living in the human GI tract. They point out that H. pylori is so ubiquitous in many populations that it is more or less “normal,” and that in most people who carry it, it does not cause overt disease.
Moreover, they note that gastric colonization with organism inhibits ghrelin, a very important signaling molecule that increases appetite.
In particular, Dr. Martin Blaser and his team of microbiologists at New York University have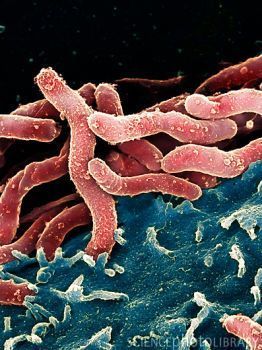 forwarded an argument that H. pylori could be playing an important role in preventing obesity, and that eradication of the organism may be contributing to the risk of obesity by increasing ghrelin output. Dr. Blaser and other H. pylori “defenders” also note that incidence of gastroesophageal reflux (GERD), asthma and obesity are inversely correlated with prevalence of H. pylori.
forwarded an argument that H. pylori could be playing an important role in preventing obesity, and that eradication of the organism may be contributing to the risk of obesity by increasing ghrelin output. Dr. Blaser and other H. pylori “defenders” also note that incidence of gastroesophageal reflux (GERD), asthma and obesity are inversely correlated with prevalence of H. pylori.
Blaser and those who align with his views make very important points, ones that underscore the complexity of the interactions between us human beings and the microbial worlds we host within our GI systems. The H. pylori story is not a simple one.
There’s no doubt that this organism can be pathogenic. It lives under the mucous layer, protected from stomach acid, and it provokes TH1 cells, and triggers gastric mucosal IL-8 secretion, which promotes inflammation. This organism produces ammonia, which raises stomach pH. It also damages acid-producing cells. On the other hand it can also induce hyperacidity by destroying somatostatin-producing antral mucosal cells.
H. pylori has been associated with a host of significant illnesses, including: Atrophic and autoimmune gastritis; Erosive gastritis and NSAID gastropathy; Hypertrophic gastritis; Duodenal ulcers; Gastric carcinoma; Gastric lymphoma; Functional dyspepsia; Coronary heart disease; Stroke; Rosacea; Raynaud’s syndrome; Sjogren’s syndrome; Parkinson’s disease and others.
My inclination is to treat H. pylori as a potential pathogen, and with due respect to Dr. Blaser, in practice I have never regretted controlling it in my patients. I have yet to see any blowback in the form of increased GERD or asthma.
That said, there is a middle ground between total eradication of this organism and total tolerance. It is possible to use natural therapies to control H. pylori without totally wiping it out.
Here’s what I’ve found helpful:
• Lactobacilli: Obtained from fermented foods & supplements, lactobacilli inhibit the growth of H. pylori.
• Mastic gum (P. lentiscus), used to make rice pudding, and for treatment of dyspepsia, can kill H. pylori.
• Garlic: Raw or as an aqueous extract, garlic can inhibit growth of H. pylori. It contains thiosulfinate, which has an MIC of 40 mcg/ml against H. pylori. It is interesting to note that garlic and onion consumption are inversely associated with gastric cancer.
• Cabbage & Broccoli: Sulforaphane, found in these vegetables, has an MIC of <4 mcg/ml against H. pylori. Cabbage juice and broccoli sprouts have been used successfully to treat peptic ulcers.







