
“Food is medicine.” It’s an idea that goes all the way back to Hippocrates, if not before him. In one form or another, this notion is found in many cultures all around the world.
It is easy to say, and it has been getting a lot of lip service in recent years. But what does it really mean? How can we make it practical for the good of our patients?
We know that diet-related disease is a leading cause of death and disability in the US, as the 2019 Global Burden of Disease study clearly points out. “Among all forms of malnutrition, poor dietary habits, particularly low intake of healthy foods, is the leading risk factor for mortality,” the authors point out.
As the COVID-19 pandemic drags on, the consequences of poor diet and unhealthy lifestyle become even more apparent. There are clear, well documented correlations between heart disease, diabetes, obesity and other metabolic disease states and increased risk of becoming infected with and dying from SARS-CoV-2.
Preserving Health, Mitigating Risk
There is an easy and inexpensive way to reduce the risks across the board: eat healthy food. As healthcare professionals, we need to start prescribing food as medicine. To do that, we need to learn about food—and not just its calorie content or its saturated fat levels. We need to understand how food works, and teach that to our patients.
While food cannot replace medication entirely, it can be an invaluable daily tool to help preserve health, and prevent, reverse or at least mitigate heart disease, hypertension, diabetes, and many inflammation-related conditions.
What we eat is the main culprit behind many chronic diseases. American diets are high in added sugars, sodium, and saturated fat commonly found in processed foods. These foods are intentionally developed to be addictive. Over the past 30 years, fast-food restaurants have adopted this flavor profile. As a result, we as a population have become sicker and less resilient. The COVID crisis is making us all too aware of this fact.
Food is a major contributor to the chronic disease problem, as Akash Goel, and his co-authors Chef Michel Nischan, Chef Tom Colicchio, and former Senator Bill Frist underscore in their recent editorial on CNN.
“Poor metabolic health stems, in part, from poor-quality diets and poor nutrition. Just as baseline chronic disease portends a worse outcome for individuals with Covid-19, our food system is our country’s pre-existing condition that leaves us all at greater risk,” they write.
But food can also be the solution. Using food as preventive medicine can keep people healthy. Eating a whole-food, mostly plant-based Mediterranean style diet that minimizes consumption of heavily processed foods is the foundation for healthier people and a healthier planet.
Medically-Tailored Meals
If chronically ill people eat a nutrient-rich diet, they may need less medication, reduce emergency room visits, and require fewer hospital admissions. That’s the premise behind the Food is Medicine Coalition—a non-profit organization providing medically-guided food and nutrition plans to thousands of people struggling with chronic conditions and who are unable to shop or cook for themselves.
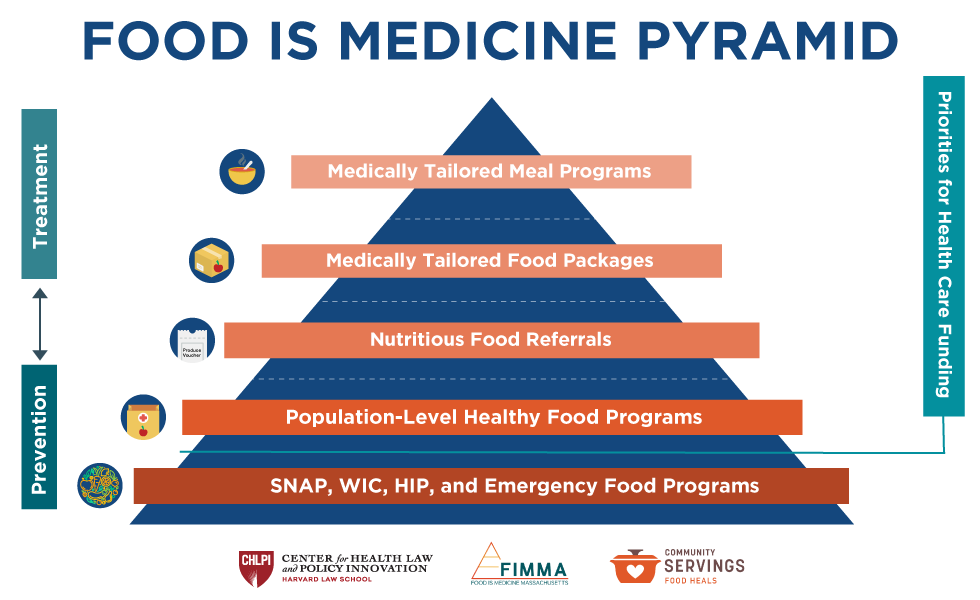
The Coalition holds that medically-tailored meal programs should be part of the treatment plans for all people struggling with chronic metabolic disorders—the 5% of the population that generates 50% of all healthcare costs. The coalition specializes in working with specific sub-populations including the elderly, people with HIV/AIDS, those with chronic kidney disease, those with metabolic syndrome or diabetes, and those with congestive heart failure.
The organization’s meal plans are developed by registered dietitians who assess each patient individually, and they consist of healthy foods tailored to meet that person’s specific health needs.

Certain eating patterns can be as effective as prescription medications for some health conditions. These include:
- Mediterranean diet for cardiovascular disease, type 2 diabetes, and more
- The Dietary Approaches to Stop Hypertension (DASH) diet for high blood pressure
- Plant-based diet for a variety of conditions such as high blood pressure and diabetes
- An anti-inflammatory eating pattern for rheumatoid arthritis and other diseases
- Specific diets for gut health, including a low FODMAP diet.
But it is very important to recognize that the same diet does not work for everyone. Different clinical conditions require different meals, foods, and beverages.
Making it Easy
According to the Food is Medicine Coalition, a medically tailored meal, “does not simply mean putting someone on a diet. Our clients’ medical lives are complex – many are living with more than four serious illnesses at once – and they require an equally complex nutrition intervention. This is why our model requires an assessment by a Registered Dietitian Nutritionist who then tailors the meal plan to the unique needs of the individual.”
The group has developed a sophisticated set of food and nutrition standards, well-grounded in research, that have been shown to result in better health outcomes, lower medical costs, and improved patient well-being.
Another company working along similar lines is Performance Kitchen, which employs a team of Registered Dietitians to design meals in alignment with many of the evidence-based diets. The company ships prepared frozen meals directly to its clients. Performance Kitchen also offers free 30-minute nutrition consultations to determine which foods each individual needs. I serve as Performance Kitchen’s scientific advisor and chef.
Deserts & Swamps
In many communities across the country, people simply do not have access to proper grocery stores and fresh, healthy produce. These are the so called “food deserts.” They’re typically low-income communities—urban or rural—where shopping choices are very limited, and most of what’s available is processed and packaged foods that are loaded with sugar, salt, saturated fats, preservatives and artificial flavorings and colorings.
These same areas are often “food swamps” in the sense that cheap fast-food restaurants—serving up similarly unhealthy convenience foods—are plentiful (read Bodegas Predict BMI in Inner City Youth).

The net result is that people who are already vulnerable–owing to the myriad health problems that accompany poverty—have ready access to foods that will exacerbate health problems, but limited access to the nutrient-dense plant-based foods that will strengthen their resilience and heal their bodies.
If we are going to be serious about “food is medicine,” we must recognize that ease of access and convenience are major drivers of peoples’ food choices. We need to make healthful meals more readily available to at-risk people at prices they can afford.
Performance Kitchen’s CEO, Christine Day, says she joined the company because she saw its potential to address the access issue. It began with personal experience: her mother had type 2 diabetes and Christine–formerly the CEO of the popular yogawear company, Lululemon–had difficulty finding convenient, nutritious, ready-made meals for her father to prepare.
She made it part of her mission to ensure that Performance Kitchen’s meals are nutritious, accessible, and affordable so that everyone can access healthy meals.
A FRESH Approach
The food we eat gives our bodies the information it needs to function properly. If we don’t get the right information then our metabolic processes suffer and our health declines. It really is that simple.

In working with patients over the years, I’ve developed a series of simple steps, guidelines, and recipes to help them implement food-as-medicine and positive lifestyle change into their lives, in a fun and sustainable way.
I call this system the FRESH 5. The acronym stands for Food, Relaxation, Exercise, Sleep and Happiness.
We recently put it all together in a patient-friendly course available free of charge on my Fresh Medicine website. We’ve found over the years, that a few simple steps can make a profound difference in peoples’ lives, as they discover the healing power of the food they eat and the choices they make.
END
Robert Graham, MD, is a Harvard trained physician, Board Certified in both Internal and Integrative Medicine and has over 15 years of clinical experience. He is also a trained chef, who has been working at the crossroads of healthcare and culinary culture for years. Among his many achievements are the Lenox CHill Initiative, which brought yoga and meditation to clinicians working at NYC’s Lenox Hill Hospital; and the Victory Greens project, which created a rooftop vegetable garden that provides “rooftop to bedside” food service for Lenox Hill patients. With his wife Julie, he co-founded FRESH Med, an integrative medical practice in Lower Manhattan that focuses on Food, Relaxation, Exercise, Sleep, and Happiness.







