
Patient self-assessment tools, along with remote consultation technologies, have evolved rapidly over the last decade. Until recently, they’ve been considered luxuries for highly motivated patients and future-forward clinicians.
In the post-COVID world, where many physicians have closed their clinics and patients are deferring all but the most essential in-person visits, telemedicine and remote monitoring are no longer luxuries, they’re necessities. And they will shape the future of clinical practice—especially in preventive medicine.
Here are a few home monitoring and self-assessment strategies that allow patients to take more active roles in their care, while providing practitioners with pertinent information to guide them along the way.
Befriend Technology
The current situation is obliging all of us in medicine to befriend new technologies. I have found a few basic tracking devices particularly helpful. These gadgets are user-friendly and built for ease-of-use at home. They can accurately track various health measurements and are compatible with many different wireless and internet platforms. They make it easy for patients and their practitioners to view and manage health data together as a team.

Blood Pressure Monitor: Maintaining a healthy blood pressure is essential. I suggest using a device like the Omron wrist blood pressure monitor. It is lightweight and portable, allowing patients to track their blood pressure on the go. It stores the readings, and the app interfaces with the patients’ computers, so they can keep and share comprehensive records of their recordings. I personally find the wrist version less cumbersome than the arm version.
Digital Stethoscope: Digital stethoscopes such as Eko stethoscopes use Bluetooth to pair with smartphones and tablets through the Eko App. Clinicians can listen to, visualize, and share auscultations of the same quality as if they were listening directly to their patients’ hearts in person, through ordinary stethoscope earpieces. This foregoes the need for close doctor-patient contact. Wireless stethoscope technology makes telemedicine exams much easier.
Assessing Cardiovascular Function
Heart Rate Monitors: The Resting Heart Rate is the number of times the heart beats per minute when someone is at rest. A good time to check this is in the morning after a good night’s sleep. For most of us, the RHR is between 60 and 100 BPM. But this can be affected by factors like stress, anxiety, hormones, medication, and level of physically activity. Athletes and highly active people may have RHRs as low as 40 BPM. When it comes to RHR, lower is definitely better, because it means that the heart muscle is in better condition and doesn’t have to work as hard to maintain a steady beat. Studies show that a higher RHR is linked with lower overall fitness, higher blood pressure, and overweight.
The Peak Heart Rate is 85 to 100 percent of someone’s maximum heart rate. I like to strive for a resting pulse rate of 50 BPM or less while asleep, and not more than 100 BPM when active.
Most of the current generation of smart phones come with the capacity to monitor both resting and peak heart rates. There are dozens of heart rate monitoring apps that make use of this built-in capacity to provide quick and easy analyses, no math required. I recommend looking for one that suits your patients’ needs. They are very useful.
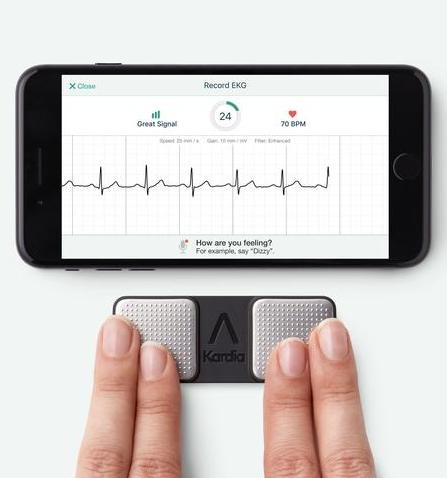
Detecting Atrial Fibrillation (AFib): The irregular heartbeat patterns associated with AFib can lead to blood collecting in the heart, which can form stroke-causing clots. Tracking Afib at home is pure common sense. Just over two years ago, the FDA approved the AliveCor Heart Monitor— a smartphone app plus a special phone case with a set of sensors. Together they convert the phone into an EKG machine that patients can carry around in their pockets or purses. It allows you and your patient to see a simple version of the heart’s electrical activity in real time on the phone screen.
The system is very easy to use. A patient activates the app, places the index and middle fingers of each hand on the sensor pads, and records an EKG tracing. In the latest version, called Kardia, the sensors just need to be near–not necessarily on– the phone.
Heart Rate Variability & Autonomic Nervous System Assessment: The effect of heart activity on brain function—and vice versa–has been researched extensively over the past 40 years. Early research mainly examined the effects of heart activity occurring on a very short time scale – over several consecutive heartbeats at maximum. Scientists at the HeartMath Institute have extended this research by looking at larger-scale patterns of interaction between the heart, the brain, and the nervous system.
Heart rate variability (HRV) is a measure of the beat-to-beat changes in heart rate. The normal variability in heart rate is due to the synergistic action of the two branches of the autonomic nervous system (ANS). The sympathetic nerves accelerate heart rate, while the parasympathetic (vagus) nerves slow it down. The sympathetic and parasympathetic branches of the ANS are continually interacting to maintain cardiovascular activity in its optimal range and to permit appropriate reactions to changing external and internal conditions.
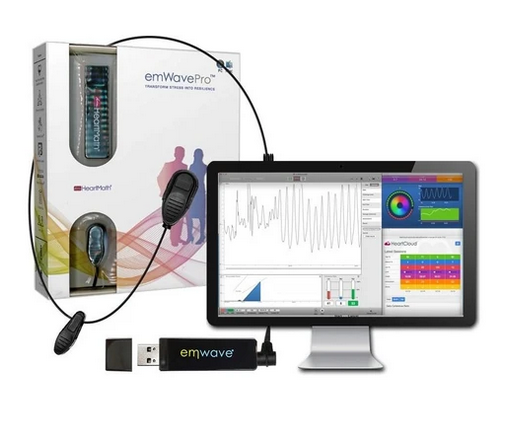
With that in mind, analysis of HRV over the course of someone’s day therefore serves as a dynamic window into the balance of the autonomic nervous system. While this seems complicated, it can be tracked fairly easily via a set of user-friendly smartphone-based tools. I recommend looking at Heart Math’s devices & apps that patients can use to monitor their HRV and self-entrain healthier, more coherent, and balanced physiological states.
Remote Lung Assessment
Spirometry & Lung Function Assessment: For patients with asthma, and others in need of frequent and regular spirometric testing, the Aluna Spirometer is the perfect solution. It enables patients to measure their lung function at home, which is a great asset for those who’ve had COVID or who are at high-risk, as it can potentially eliminate clinic visits.

The Aluna system consists of a special breath test device that links wirelessly to a smartphone, and an app for collecting the spirometry data. It calculates FEV1 instantly, and records, stores, and shares the readings. The app also has a medication utilization tracker, and a video game component—particularly well-suited to children and young patients—that explains what the readings mean and allows users to set lung function goals.
Aluna gives doctors an online dashboard on which to monitor their patients’ spirometry data as it is being collected. Alternatively, patients can choose to share the results over the internet. Aluna can help doctors and patients work together to build a more precise, customized treatment plan that keeps patients engaged in their own self-care.
In addition to these helpful devices and smartphone systems, there are 5 low-tech self-assessments that I recommend that we all use routinely. You can find complete protocols for these simple self-assessments at https://www.perqueintegrativehealth.com/lifestyle/self-tests/.
Low-Tech Options
First Morning Urine pH: The first morning urine pH is a good indicator of the body’s mineral reserve and its acid/alkaline state. The body routinely uses overnight rest time to excrete excess acids. One’s capacity to do so varies based on toxin load, individual ability to inactivate toxins, and to excrete them. Using a pH test strip, this is a simple, inexpensive at-home test. Maintaining a pH within 6.5- 7.5 is ideal, indicating that overall cellular pH is appropriately alkaline. Cells in all tissues of the body function best in an alkaline state.
Digestive Transit Time: The state of one’s digestive system affects all aspects of health. Measuring digestive transit time gives an idea of how long it takes for food to be digested and for waste to be eliminated. The ideal transit time is between 12-18 hours. Most people who eat the standard American diet have transit times of 36-96 hours, which is detrimental to overall health.
With the help of a few charcoal capsules, patients can easily and painlessly find out how well their digestive organs are doing their jobs. This can help guide decisions about the amount of fiber, probiotics, and other digestive support they need.
C Cleanse: This test uses buffered vitamin C (ascorbate)–the body’s universal antioxidant—to identify a person’s risk of oxidative stress and extent of antioxidant protection.
The process involves taking buffered ascorbate powder in increments of 15 minutes till there is a complete evacuation of the GI tract, or a flush/cleanse is achieved (watery stools). In people who are generally healthy and getting enough vitamin C, this “C cleanse” protocol will give a result of ≤4g. But it is not uncommon to see results of 50, 75 or even 100g, indicating that someone is very deficient in ascorbate. I recommend doing the C cleanse every week.
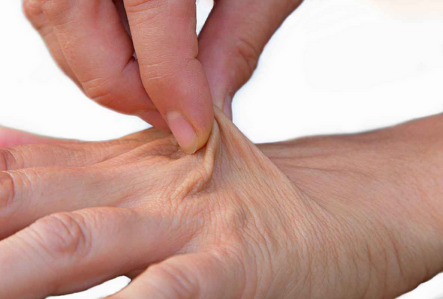
Wrist Skin Pinch Test: Drinking enough water each day is crucial for many reasons: to regulate electrolyte balance, support kidney function, keep joints lubricated, prevent infections, deliver nutrients to cells, and keep organs functioning properly. Being well-hydrated also improves sleep quality, cognition, and mood.
A simple self-test for hydration status that I like to recommend is called the wrist skin test:
– Gently pull up about ½ inch on the skin on the back of the wrist with the hand extended out (not flexed either up or down).
– On releasing the pinch, if the skin immediately flattens, it is a sign of well-hydrated tissues. However, if the skin maintains a little ‘tent’ i.e., stays pinched and then slowly goes back to normal over 5-10 seconds, it is usually a sign of significant dehydration
Urine Specific Gravity (SG): Urine specific gravity is another important measure of hydration and kidney health that can be used to assess the kidney’s ability to concentrate or dilute urine. Ideally, urine SG measurements will fall between 1.002 and 1.030 if the kidneys are functioning normally. Numbers above 1.010 can indicate mild dehydration. The higher the number, the more dehydrated someone will likely be.
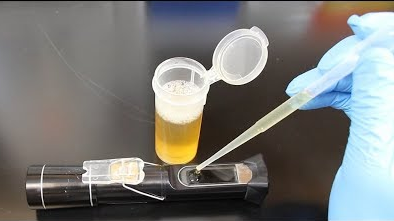
I like to use a refractometer for this test which projects light into the sample and helps determine the density of the urine.
There’s no question that the COVID pandemic has moved telemedicine and remote monitoring from the margins of healthcare into the mainstream. In many ways, this shift provides new opportunities for patient empowerment and practitioner emancipation.
Office visits will always have a prominent place in medical practice, but they need not be the default setting for everything.
Telemedicine is not the be-all, end-all solution to the problem of healthcare access—many people do not own smartphones or computers—but this technology can help many people improve their health and wellbeing in ways that are convenient and affordable. It opens exciting new possibilities for how we practice and experience healthcare—possibilities we are just beginning to explore.
END







