Depression impacts about 120 million people worldwide1, and each year about 6% of men and 9.5% of women experience an episode of depression. The World Health Organization predicts depression to become the second most burdensome disease by 2020, with the greatest burden in North America and the United Kingdom2.
Over 160 million antidepressant prescriptions are written annually, despite the fact that recent meta-analyses show they are no more effective than placebos to treat mild to moderate depression—the most common condition for which they’re prescribed3.
Other studies reveal these medications can cause a host of problems including sexual side effects, infertility4, increased risk of weight gain and diabetes5, blood pressure problems6, cardiac deaths7,8, heart defects in unborn children9, and even suicide.
The Holistic Advantage
Holistic practitioners are at a distinct advantage when treating people with depression. While conventional medical thought focuses on medications to augment neurotransmitter function, holistic care addresses the multitude of factors that contribute to the syndrome we call depression.
The situation reminds me of that old joke about the drunk man at night looking for his keys in a mostly dark parking lot. After circling for hours in the same small but well-lit spot, he runs into another man who’s not inebriated, and who asks him, “How do you know your keys are here, when there’s the rest of this lot to check?” The drunken man answers, “Well, they could be out there somewhere too, but the light is better here.”
As holistic practitioners, it is our job to start shining the light in other areas of depression’s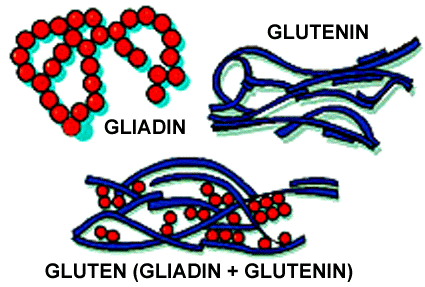 parking lot. We have tremendous opportunity to start looking into other factors, including sleep problems, diet, nutrient depletion, toxicity, stress, hormonal balance, and many others. This article will key in on the role gluten may play in mood and depression.
parking lot. We have tremendous opportunity to start looking into other factors, including sleep problems, diet, nutrient depletion, toxicity, stress, hormonal balance, and many others. This article will key in on the role gluten may play in mood and depression.
What, Exactly, is Gluten?
Gluten is comprised of the proteins gliadin and glutelin (glutenin is the most common among the glutelin family). Gluten is found in foods processed from wheat and related grain species. Gluten is ubiquitous throughout the modern world, both in foods prepared directly from wheat/grains like breads and other flour-based products, and as an additive to foods otherwise low in protein.
Unfortunately for many people, gluten can create unfavorable digestive tract reactions, leading to poor brain circulation, neurotransmitter imbalances, and poor nutrient absorption, all of which can promote low mood.
Gluten is found primarily in wheat, but is also found in rye, triticale, spelt, and barley. Many people believe that oats contain gluten, and that people with gluten sensitivities should avoid them. In reality, the evidence suggests that oats themselves are safe for most people with celiac disease; the issue is that oats and oat-containing foods are often processed in facilities that process other gluten-containing grains, and become contaminated with gluten from these other grains. Good health food stores will usually stock certified gluten-free oats10.
Celiac, Circulation, Neurotransmitters & Nutrients
Celiac disease is an inflammatory disease of the upper small intestine resulting from gluten ingestion in genetically susceptible individuals. Positive results on celiac blood panels can strongly suggest this condition; intestinal biopsy confirms the diagnosis.
We can learn a lot about the connection between gluten intolerance and mood by studying celiac disease. One small study showed that a high proportion of adults with celiac disease had a prior history of psychiatric treatment, even years before diagnosis. In this study, 21% of the 42 study participants had attended a psychiatric clinic due to ‘neurotic’ and mostly ‘depressive disorders,’ and six had been granted disability for chronic depression, versus only 5% of the control group11.
In one evaluation of brain circulation, 15 celiac disease patients given a gluten-free diet were compared with 15 untreated patients. Seventy-three percent of the untreated patients had at least one brain region showing hypoperfusion, compared with only 7% of gluten-free celiac patients. Cerebral perfusion was significantly lower in untreated celiac patients, compared with healthy controls in 7 of 26 brain regions.
By the end of the study, the gluten-free celiac patients and healthy controls were more or less equivalent in terms of cerebral perfusion. It is important to note that cerebral hypoperfusion correlates with higher levels of both anxiety and depression12.
Tryptophan, the amino acid that converts to 5-hydroxytryptophan, and ultimately to the “feel-good” neurotransmitter serotonin, is vulnerable to malabsorptive conditions like celiac disease. If gluten irritates enterochromaffin cells (aka, Kulchitsky cells, that store 90% of the body’s serotonin), large amounts of serotonin are released to increase peristaltic movements so that the gut empties. Functionally, this lowers serotonin stores, which will alter neurotransmitter balance.
Chronic gluten-induced inflammation causes atrophy of the villous structure of the jejunum, leading to malabsorption of several important nutrients13. For example, iron deficiency is often found in celiac patients14. Low iron stores are also shown to contribute intensity of fatigue and depression15,16.
Researchers studying the blood of children with celiac disease found significantly decreased plasma concentrations not only of tryptophan, but also citrulline, tyrosine, valine, isoleucine, and leucine. In untreated and treated children with celiac, plasma tryptophan was 84% lower and 62% lower, respectively, than in children without celiac. Nine of 15 children with untreated celiac showed signs of “behavioral disturbances,” and were irritable or apathetic17.
Studies of people with celiac disease show us that there are abnormally low amounts of tryptophan in spinal fluid of those with depression and behavior disorders, and this is reversible with a gluten free diet18.
For patients who are gluten-intolerant or have overt celiac, it is imperative to encourage a switch away from wheat and other gluten-containing grains, and toward non-gluten forms of carbohydrates (such as fruits, rice, millet, starchy plants like potatoes and root vegetables, amaranth, and wild rice).
Allergens, Exorphins & Endorphins
Given our knowledge of the connection between celiac disease and mood disorders, it is reasonable to consider other individual food sensitivities that may induce similar inflammation and malabsorption.
One double-blinded experiment on 30 subjects found a correlation between sublingual exposure of known food allergens and increased cognitive-emotional symptoms and heart rate changes19.
While considering food allergy and sensitivity, think about molecules called ‘exorphins’ which are derived from the incomplete digestive breakdown of dairy and grain derived foods20. Exorphins are small protein or peptides that have an action like morphine. Endorphins, exorphins and morphine all work by way of opioid receptors21. Five exorphins have been discovered in digests of gluten and eight others in digests of milk22.
The discovery of these psychoactive exorphins offers a possible explanation for some of the reported psychiatric reactions to these proteins including the sense of “brain fog” that often accompanies immune reactions to dairy and grain foods23,24. Exorphins may also modulate mood by depressing serotonin, dopamine and norepinephrine in the central nervous system.
You Tell Me That It’s Evolution
It is interesting that many of the foods that seem to be implicated in depression are also foods that—on the time-scale of evolution–are relatively new to humanity. Some of the problems may stem from the fact that as a society, we are consuming vast quantities of the very foods to which we’ve had the least amount of evolutionary time to adapt.
Celiac disease is characterized by an overt inflammation pathology that affects brain circulation, nutrient absorption, and neurotransmitter balance. These will all negatively affect mood, and can be remedied by avoiding gluten-containing foods. That said, we do sometimes see ‘withdrawal reactions’ when susceptible patients first remove offending gluten. In some patients, careful monitoring and slow dietary changes may be prudent.
Beyond gluten and dairy elimination, we have found in our practice that allergy elimination diets and subsequent challenges, careful diet/symptom diary recall, and blood type considerations are most helpful to characterize other individual food sensitivities.
For patients with predominantly gut-related mood disorder, the first step is to identify the offending food(s) and strongly encourage patients to eliminate them from their daily diets. Stress reduction work such as meditation, acupuncture, and psychological work are key to return parasympathetic activity and restore normal gut function to foster a more balanced mood.
For gut healing, I rely on naturopathic herbal remedies such as Robert’s Formula in between meals. This eclectic formulation of botanicals helps to reduce inflammation, remove unwanted bacteria, and heal the gut lining. Best taken in between meals, variations of this formula include Geranium maculatum, Althea officinalis, Hydrastis canadensis, and Ulmus fulva.
For repair, the nutrient glutamine can be given in the form of well-cooked cabbage, cabbage powder or as a glutamine supplement (1 teaspoon up to three times a day). I also rely on quercetin (250mg thrice daily) and turmeric phytosome (500 mg twice daily) in between meals for anti-inflammatory support. Probiotic repletion is also recommended, using a high quality potent supplement.
References
1World Health Organisation: Mental and Neurological Disorder – Factsheet 265. World Health Organization; 2001.
2WHO, Mental health: New understanding, new hope, WHO, Geneva (2001) The World Health Report.
3Fournier JC, DeRubeis RJ, Hollon SD, Dimidjian S, Amsterdam JD, Shelton RC, Fawcett J. Antidepressant Drug Effects and Depression Severity: A Patient-Level Meta-analysis JAMA. 2010;303(1):47-53.
4Tanrikut C, Feldman AS, Altemus M, Paduch DA, Schlegel PN. Adverse effect of paroxetine on sperm. Fertil Steril. 2010;94(3):1021-6.
5Andersohn F, Schade R, Suissa S, Garbe E. Long-Term Use of Antidepressants for Depressive Disorders and the Risk of Diabetes Mellitus. Am J Psychiatry. 2009; 166(5): 591-598.
6Licht CM, de Geus EJ, Seldenrijk A, van Hout HP, Zitman FG, van Dyck R, Penninx BW. Depression Is Associated With Decreased Blood Pressure, but Antidepressant Use Increases the Risk for Hypertension. Hypertension. 2009;53:631.
7Whang W, Kubzansky LD, Kawachi I, et al. Depression and risk of sudden cardiac death and coronary heart disease in women. Results from the Nurses’ Health Study. J Am Coll Cardiol 2009; 53:950-958.
8Hamer M, David Batty G, Seldenrijk A, Kivimaki M. Antidepressant medication use and future risk of cardiovascular disease: the Scottish Health Survey. Eur Heart J. 2011;32(4):437-42..
9Pedersen LH, Henriksen TB, Vestergaard M, Olsen J, Bech BH. Selective serotonin reuptake inhibitors in pregnancy and congenital malformations: population based cohort study BMJ. 2009; 339.
10Rashid M, Butzner D, Burrows V, Zarkadas M, Case S, Molloy M, Warren R, Pulido O, Switzer C. Consumption of pure oats by individuals with celiac disease: a position statement by the Canadian Celiac Association. Can J Gastroenterol. 2007 Oct;21(10):649-51.
11Hallert C, Derefeldt T: Psychic disturbances in adult coeliac disease: 1. clinical observations. Scand J Gastroenterol 1982; 17:17-19
12Addolorato G, Di Giuda D, De Rossi G, Valenza V, Domenicali M, Caputo F, Gasbarrini A, Capristo E, Gasbarrini G. Regional cerebral hypoperfusion in patients with celiac disease. Am J Med. 2004 Mar 1;116(5):312-7.
13Mäki M, Collin P: Coeliac disease. Lancet 1997; 349:1755-175
Jones S, D’Souza C, Haboubi NY. Patterns of clinical presentation of adult coeliac disease in a rural setting. Nutr J. 2006 Sep 14;5:24.
14Verdon F, Burnand B, Stubi CL, Bonard C, Graff M, Michaud A, Bischoff T, de Vevey M, Studer JP, Herzig L, Chapuis C, Tissot J, Pecoud A, Favrat B. Iron supplementation for unexplained fatigue in non-anaemic women: double blind randomised placebo controlled trial. BMJ 2003;326:1124
15Albacar G, Sans T, Martín-Santos R, García-Esteve L, Guillamat R, Sanjuan J, Cañellas F, Gratacòs M, Cavalle P, Arija V, Gaviria A, Gutiérrez-Zotes A, Vilella E.J. An association between plasma ferritin concentrations measured 48 h after delivery and postpartum depression. Affect Disord. 2011 Jun;131(1-3):136-42.
16Hernanz A, Polanco I: Plasma precursor amino acids of central nervous system monoamines in children with coeliac disease. Gut 1991; 32:1478-1481
17Päivi A Pynnönen,1 Erkki T Isometsä,2 Matti A Verkasalo,1 Seppo A Kähkönen,3 Ilkka Sipilä,1 Erkki Savilahti,1 and Veikko A Aalberg1 Gluten-free diet may alleviate depressive and behavioural symptoms in adolescents with coeliac disease: a prospective follow-up case-series study BMC Psychiatry. 2005; 5: 14.
18King DS. Can allergic exposure provoke psychological symptoms? A double-blind test. Biol Psychiatry. 1981 Jan;16(1):3-19.
19Zioudrou C, Streaty RA, Klee WA. Opioid peptides derived from food proteins: The exoprhins. J Biol Chem 1979;254:2446-9.
20Yarnell E. Exorphins, Food Cravings, and Schizophrenia http://www.healingmountainpublishing.com/articles/exorphins.html accessed June 24, 2009
21Fukudome S, Shimatsu A, Suganuma H, Yoshikawa M Effect of gluten exorphins A5 and B5 on the postprandial plasma insulin level in conscious rats. Life Sci. 1995;57(7):729-34.
22Food Allergies and Depression How Modern Eating Habits May Contribute to Depression. From Ron Hoggan M.A. & James Braly M.D.,for About.com
Updated: December 8, 2003. http://depression.about.com/cs/diet/a/foodallergies_2.htm?p=1
23Mycroft FJ, et al. MIF-like sequences in milk and wheat proteins. N Engl. J Med. 1982 Sep 30;307(14):895.
24Hallert C et al. Psychic disturbances in adult coeliac disease III. Reduced central monoamine metabolism and signs of depression. Scand J Gastroenterol, 1982;17: 25-28.
Peter Bongiorno ND, LAc, was a predoctoral fellow in clinical neuroendocrinology at the National Institute of Mental Health before attending Bastyr University for his naturopathic and acupuncture degrees. He has a thriving practice in New York City and Long Island, NY. He recently authored the textbook Healing Depression: Integrated Naturopathic and Conventional Treatments ( www.InnerSourceHealth.com/depression ); his new book, written for the general public and titled, How Come They’re Happy and I’m Not? will be released in the Spring of 2012.







