
Early in 2021, roughly one year after authorities declared Covid-19 a pandemic, a lot of people left their jobs, and business leaders began fretting about “the Great Resignation,” also known as “the Big Quit.”
Politicians, economists, and social scientists offered a wide range of plausible explanations: people had gotten used to spending time at home and wanted better work-life balance; the break gave workers a chance to re-assess their priorities and reassert their value; wages had not kept pace with living costs; compensation was not commensurate with hassle; the pandemic encouraged laziness. And on and on.
To some extent, all of these factors may be influencing the situation. But the experts missed one of the most important factors: post-viral fatigue.
Simply put, many people have experienced—and continue to experience–profound multi-system fatigue following infection with SARS-CoV-2. As is the case with other viral pathogens, this one can render people profoundly debilitated and, in many cases, unable to return to work.
A Widespread Problem
I believe the Great Resignation isn’t happening because people are lazy; it is happening in large part because many people are burdened with chronic illness.
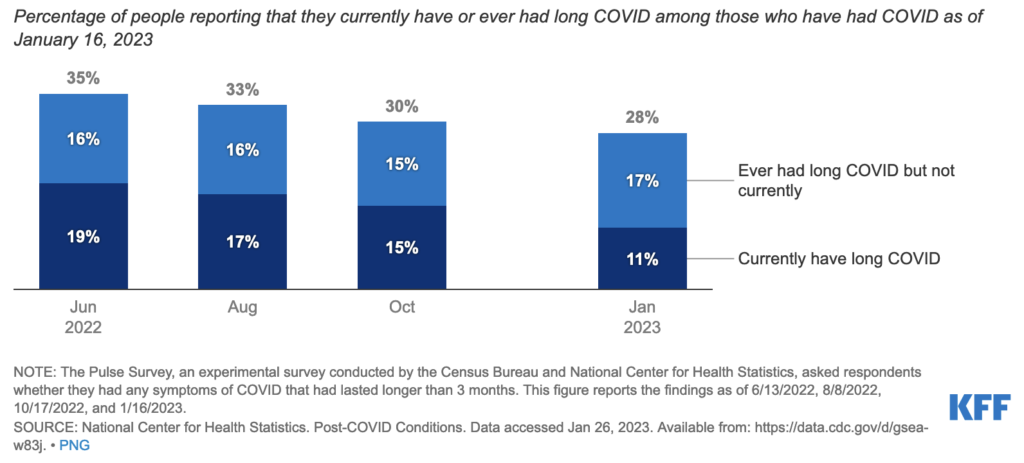
Countless infections can trigger persistent chronic fatigue syndrome or fibromyalgia (CFS/FMS). For example, Epstein-Barr virus (EBV), Herpes simplex (HSV-1), Lyme disease, and even polio have been implicated. We can now add SARS-CoV-2 to this list. Between 10 to 15% of people who’ve had Covid-19 develop persistent exhaustion, as part of the syndrome we’re now calling Long Covid.
According to the CDC’s National Center for Health Statistics, 79% of people with Long Covid experience limitations of their daily activities, and 27% have severe limitations. This assertion is based on a nationwide Household Pulse survey involving well over 60,000 individuals.
A Kaiser Family Foundation analysis of this and other surveys suggests that the debilitation caused by Long Covid, has affected at least 500,000 American workers, and the number may actually be as high as 4 million.
Gaslighting & Stigmatization
Unfortunately, our healthcare system seems to be treating Long Covid in the same way it has always treated CFS/FMS. Essentially, it is “gaslighting” people, telling them they are depressed or lazy. Historically, physicians have done this for complex, poorly understood, and time-intensive conditions, especially when they affect women and when they’re not easily diagnosed or quickly treated with profitable drugs or procedures.
Some examples? Multiple sclerosis used to be called “hysterical paralysis.” When I was in medical school, Lupus was still considered a neurosis. With CFS/FMS, patients often go for years without the correct diagnosis or thorough treatment. Too often, their doctors abusively insinuate that, “since I don’t know what’s wrong with you, you must be crazy.”
This is now occurring with Long Covid as well.
Long Covid carries considerable social stigma. A recent UK study of nearly 900 such patients showed that 95% experienced stigma at least sometimes, and 76% experienced it often. Practitioners may unintentionally contribute to the problem by failing to recognize that CFS/FM is rooted in actual post-viral pathophysiology, leading patients to believe their fatigue is a character flaw.
Exhaustion & Insomnia
Part of the challenge in treating post-Covid fatigue is that it is seldom an “all or nothing” condition, where people are either totally disabled or “just fine.” Many are “walking wounded”, so to speak. They’re marginally functional, but far from their pre-Covid energy levels.
Despite the fatigue, many have difficulty sleeping. A Cleveland Clinic study just published in the Journal of General Internal Medicine shows that 40% of a cohort of 962 patients with Long Covid have moderate to severe sleep problems.
The paradox of chronic exhaustion with insomnia is a typical feature of post-viral FM/CFS. The insomnia, along with brain fog, chronic pain, and weight gain, indicate hypothalamic dysfunction.

When someone is overloaded by viral infections, other types of infections, or extreme stress, the hypothalamus basically shuts down and the body loses one of it’s key ‘circuit-breakers’. This key control center in the brain regulates sleep, along with hormonal and autonomic function.
But it’s a tricky situation because in the first year after a primary SARS-CoV-2 infection, patients may experience hypersomnolence, which later gives way to insomnia.
I’ve created a simple 10-minute free quiz to help people make a CFS/FMS diagnosis. There’s also an easy-to-use one-page checklist for determining if someone meets the American College of Rheumatology’s 2016 diagnostic criteria for fibromyalgia. Though these tools are for CFS and FM in general, and not specific to Long Covid, they can be helpful in the post-Covid context.
Rise & SHINE
For CFS/FM of any cause, our published randomized double-blind placebo-controlled study showed that 91% improved, with an average 90% increase in quality of life, using a comprehensive approach I call the SHINE Protocol.
The acronym stands for: Sleep, Hormones (and Hypotension), Infections, Nutrition, and Exercise. By addressing these five domains, we can greatly improve the health of people with post-viral CFS.
SHINE includes supplements, botanicals, hormonal therapies and in some cases, antivirals, antifungals, antidepressants, and drugs for sleep. Exercise also plays a role. The basic protocol includes a multivitamin, magnesium plus malic acid, melatonin, and a Valerian/Melissa combination. But there are many additional options depending on an individual’s test results and clinical history.
I’ve written a number of articles on applying the SHINE protocol at the patient care level. If you’re interested in learning how, email me at FatigueDoc@gmail.com
Ginseng Revival
One herb that I’ve found to be particularly helpful for CFS/FM is Panax ginseng.
For centuries, Ginseng has been one of most popular herbal medicines in Asia, and for good reason: it can be dramatically effective for numerous conditions.
The problem is that for wild ginseng, it takes at least 17 years for a plant to mature and to develop high levels of active ginsenosides in response to harsh weather, threats from insects, and other challenges. And since it is the root portion that we use therapeutically, harvesting usually means ending the life of the plant.
Decades ago, over-harvesting of wild ginseng led to insane prices (over $700 a pound), encouraged adulterations and substitutions, and essentially drove the plant to the brink of extinction. In response, farmers began cultivating ginseng, but I found that products derived from farmed ginseng just weren’t as effective as those from wild plants. Because of this, I stopped using ginseng in my practice over 30 years ago.

Recently, cultivators developed a unique and ingenious aquaponic farming technique which reproduces the challenges the plants face in the wild. It results in a form of farmed ginseng, called HRG80TM Red Ginseng, that has the same active phytochemical profile as mature wild plants. Initially skeptical when I first tried it, I was shocked at how effective it was.
Enough so, that I decided to do an open-label study using the product with 188 patients with severe post-viral CFS. Prior to treatment, all patients reported that they were functioning at 50% or less of their pre-illness energy levels. They supplemented with 200–400 mg of the HRG80 in capsule form, or 100–200 mg in tablet form, daily for one month.
The results speak for themselves:
- 60% rated themselves as “improved,” with 13% rating themselves as “much better” (p<.001)
- 67% average increase in energy
- 44% average increase in overall well-being
- 48% average improvement in mental clarity
- 46% average improvement in sleep
- 33% average decrease in pain
- 72% average increase in stamina
The bottom line is, this unique form of aquaponically-grown red ginseng resulted in marked improvements in people with disabling fatigue, including post-viral fatigue.
Of the two delivery forms (capsule or tablet), I prefer the chewable tablets. They contain natural gamma cyclodextrin, which increases absorption almost eightfold. That means, one half to one tablet can be as effective as four capsules.
Important Considerations
Botanicals like ginseng, and other supplements, can be a big help in recovering from post-viral CFS/FM. But there are many other important things to consider:
- Recommend a good multivitamin high in B vitamins, magnesium, vitamin D, and zinc. I like the Essential multivitamin tablets by EuroMedica, two daily.
- Consider adrenal fatigue if the person gets irritable when hungry (“Hangry”).
- Give thyroid & reproductive hormone support if symptoms suggest they are needed.
- Address orthostatic intolerance (Postural Orthostatic Tachycardia Syndrome (POTS)): This is common. Here’s a quick POTS screening method you can do in the office or even have patients do at home. Ask the patient to lie supine quietly for 10 minutes, then check the pulse and blood pressure. Then, ask the patient to stand up and check the pulse and BP again, every two minutes, for 10 minutes. If the pulse goes up by 15 BPM any time during the 10-minute standing period, it is suggestive of orthostatic intolerance. If it goes up 30 BPM or more, it confirms the diagnosis. A drop of more than 10 points in systolic BP is also suggestive.
- Consider Low-Dose Naltrexone: For patients not taking narcotics, LDN by prescription from compounding pharmacies is helpful for both CFS/FMS and long COVID.
An Ounce of Prevention
Covid-related CFS/FMS is more likely in people who felt they needed to push through the acute infection phase, instead of resting. It’s so important to let patients know that rest is critical when fighting off a viral pathogen—or any bug, for that matter.
Metformin may also have a role in preventing Long Covid. According to a large phase 3 treatment trial of 663 overweight people in The Lancet earlier this year, metformin reduced incidence of long Covid by half, if the drug was given within the first four days of acute symptoms.
When starting patients on metformin, I begin with 500 mg on the first day, to make sure that nausea or diarrhea are not severe, and then increase the dose to 500 mg twice a day for 4 days. From there, I increase to 500 mg each morning and 1000 mg at bedtime for a total of two weeks. Metformin is especially important for people who already have CFS/FMS, to decrease the risk of a flare.
END
Jacob Teitelbaum, MD, is one of the world’s most frequently quoted integrative medical authorities. He is the author of several best-sellers, including From Fatigued to Fantastic!, the Beat Sugar Addiction Now! series, The Fatigue and Fibromyalgia Solution, and the popular free smartphone app Cures A-Z. He is the lead author of 4 studies on effective treatment for CFS/FM. In 1975, an extended bout of post-viral CFS left him homeless. He has dedicated his life to researching and writing about effective treatments for CFS/FM. Dr. Teitelbaum earned his MD from Ohio State University, and recently celebrated his 50th year as a physician.
Learn more at Vitality101.com.







