 |
|
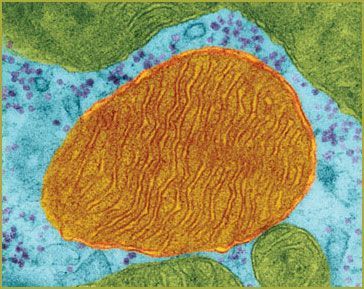
| Mitochondrion of a heart muscle cell: For decades, heart disease prevention has been focused on lowering lipids to slow coronary artery blockage. Metabolic cardiologists shift the focus to the myocardium itself, using nutritional strategies to improve ATP synthesis and improve heart muscle function. Photo: Copyright Dennis Kunkel, PhD/Visuals Unlimited. |
A new vanguard of “metabolic” cardiologists contends that cholesterol elevation has been overstated as a cause of heart disease, and that physicians would do well to pay closer attention to the myocardial metabolic dysregulation and chronic inflammation that play equally important roles in heart attacks, strokes, and congestive heart failure.
They describe a myocardial “energy crisis,” in which the heart muscle cannot produce sufficient energy for proper pump function. This metabolic dysfunction both contributes to, and is a result of, the overall cardiovascular disease process.
Metabolically-minded cardiologists do not categorically dismiss LDL elevation as a contributing factor, but they believe American medicine’s near obsession with lipid-lowering has become myopic. Clearing blocked arteries and reducing serum LDL does not necessarily restore normal heart function, as the rising tide of congestive heart failure (CHF) cases has shown. Nor will it always prolong survival in patients who’ve already had myocardial infarctions.
The good news is that in many cases, cardiometabolic dysfunction is reversible, or at least improvable through supplementation with four safe, and relatively inexpensive nutrients: D-ribose, L-carnitine, magnesium, and Co-enzyme Q10. The effects, in terms of improved heart function, can be profound.
Questioning Cholesterol
The ENHANCE (Ezetimibe and Simvastatin in Hypercholesterolemia Enhances Atherosclerosis Regression) study, released in January and debated hotly at the American College of Cardiology’s annual meeting in March, has raised questions about the seemingly ironclad equation that intensive LDL lowering leads to reversal of atherosclerosis, and therefore to reduced risk of cardiovascular events and death.
ENHANCE showed that the cholesterol-lowering combo-drug, Vytorin (Ezetimibe plus Simvastatin) did not reverse carotid artery plaque thickess despite the expected lowering of LDL (Kastelein JJ, et al. N Engl J Med. 2008; 358(14): 1431–1443). The findings are limited to that particular drug, and are not generalizable to all cholesterol lowering therapies. The consensus among cardiologists at the ACC meeting is that while the ENHANCE data were surprising, they are not grounds to dismiss statin-based lipid lowering.
But some doctors, and certainly many patients, take the findings as permission to question the premise of LDL-lowering as the primary means of preventing heart attacks. (Visit www.holisticprimarycare.net and read “Bad Cholesterol”: Good Marketing, But Is It Good Medicine? by Dr. Cleaves Bennett.) The fact that Merck and Schering-Plough, the drugmakers who jointly own and market Vytorin, kept the ENHANCE data from publication for two years, has only stoked suspicion, not only in medical circles, but in Congress as well; a congressionally mandated investigation into conduct of the trial is now underway.
The Merck/Schering official statement following ENHANCE rightly points out that the drug did exactly what it claims to do: maximally lower LDL. But people don’t take these drugs because they want to lower a blood lipid, they take them because they want to avoid dying prematurely of a heart attack. If maximally lowering LDL does not reduce atherosclerotic plaque thickness, can we still safely assume that it will reduce heart attack incidence?
Second-Thoughts About Statins
Stephen T. Sinatra, MD, a Manchester, CT, cardiologist, is among the pioneers of the new metabolic cardiology movement. He believes the relationship between cholesterol and cardiovascular disease, “has been way overplayed in this country.” In an interview with Holistic Primary Care, Dr. Sinatra suggested that physicians worry less about blood lipids and more about what’s actually happening in the heart muscle itself.
Dr. Sinatra has published a number of popular books on managing cardiovascular risk, including the widely acclaimed and recently revised, The Sinatra Solution (Basic Health Publications). He said ENHANCE really does not change his view or his practice; he has been very cautious about using statins for years now.
There’s only one category of patients for whom he routinely prescribes statins: males aged 50–75. “These are the people for whom statins have their greatest benefit with the least amount of baggage. And that’s because in addition to LDL lowering, statins have a potent anti-inflammatory effect. In this patient group, the anti-inflammatory effect may be as important as the LDL lowering.”
That premise was certainly given new credence with the early cessation this Spring of JUPITER (Justification for the Use of Statins in Primary Prevention: An Intervention Trial Evaluating Rosuvastatin), a massive 15,000 patient study showing that rosuvastatin (Crestor) rapidly reduced MI incidence, morbidity and mortality compared with placebo, in patients with already low LDL, but high c-reactive protein, a definite marker of inflammation.
Statins & Diastolic Dysfunction
Over the last 10 years, a period of widespread statin consumption, there has been a decrease of coronary artery disease, but a marked increase of CHF, which is really a disorder of heart muscle function. Aging of the population accounts for part of that increase, but Dr. Sinatra is convinced statins also play a role.
“We know statins can cause diastolic dysfunction. In a 2004 study by Marc Silver and colleagues, two-thirds of patients had diastolic dysfunction after 6 months of statin therapy. I think we’re going to see a real epidemic of CHF as the population of people on statins continues to age” (Silver M, et al. Am J Cardiol. 2004; 94(10): 1306–1310).
Lipid management does play a role in Dr. Sinatra’s approach to heart disease, but a small one. “I do a VAP test (Vertical Auto Profile, a 15-component cholesterol test developed by Atherotech). If the particles are small, dense and oxidized, I will be more aggressive. But generally, I’m not very aggressive about lipids. We need cholesterol. For example, vitamin D is made through sun exposure, but you need cholesterol in the skin to form 25-OH vitamin D. Some doctors drop peoples’ cholesterols so low, I think they’re playing with fire.”
Lee A. Surkin, MD, a nutritionally-oriented cardiologist in Greenville, NC, agrees that lipid lowering can have downsides and that it is only part of the picture of heart disease management. But he is not so quick to dismiss statins, and he believes the ENHANCE findings have been over-blown.
“How you interpret ENHANCE will depend on how much stock you put into intimal medial thickness as a surrogate marker for cardiovascular outcomes. The fact that simvastatin plus ezetimibe did not affect carotid plaque thickness? So what? To me, it is all about outcomes, and ENHANCE was not an outcomes trial. It was not powered to look at MI and stroke.”
Dr. Surkin, who acknowledged that he was not a big prescriber of Vytorin to begin with, said ENHANCE does underscore a major issue with the drug development, testing and approval process: drugs like Vytorin can get to market without actual outcomes data but based on favorable changes in surrogate endpoints only. “It would be great if the pharma companies had to show outcomes data before the FDA approved a drug. I wish the FDA required it.”
Niacin “Does Everything Right”
According to Dr. Surkin statins are appropriate for many patients at increased cardiovascular risk, but he also firmly believes doctors should be mitigating the potential side effects with Co-enzyme Q10. He also contends that niacin has much to offer, but is still underutilized. “Niacin does everything right. It lowers LDL and triglycerides, it raises HDL, and it changes lipid particle size to make it less risky. In a way, it’s close to the ideal drug.”
Flushing is, of course, the major downside. “It’s a nuisance rather than a serious health risk, and we don’t know why one person flushes and another does not. But in my practice I’ve found it tough to get people who do flush to stay on.” Aspirin can reduce both the incidence and severity of flushing. Dr. Surkin generally tells patients to take the Niaspan sustained-release niacin, along with a low fat snack, right before bedtime, and roughly 30 minutes after taking an aspirin.
Though he is more forgiving of statins, Dr. Surkin told Holistic Primary Care that he strongly agrees with Dr. Sinatra that doctors need to look at the metabolic aspects of heart disease and to make wider use of nutrients like Co-Q10, ribose, Hawthorn and omega-3 fatty acids, not only for preventing first cardiac events but in the long-term management of people with advanced disease.
The Awesome Foursome
The lipid lowering approach is focused on the vessel walls as the locus of heart disease. The metabolic approach shifts that focus to the myocardium itself. In any form of heart disease, whether it is coronary artery blockage, infection, congenital defect, or drug side effect, the myocardium will show some degree of impairment in the ability to make sufficient quantities of adenosine triphosphate (ATP), the biochemical currency that drives cell function.
This is why so many heart disease patients, regardless of the initial cause, end up with CHF. Even with revascularization and reoxygenation, many people who’ve suffered myocardial ischemia never fully recover normal myocardial function; the tissue itself is operating at an energy deficit.
“Metabolic cardiology aims to improve the energy transfer and the overall function of the myocardium and the endothelium,” explained Dr. Sinatra. “Of all the organs of the body, the heart uses the most ATP and has the most constant demand for it. So faulty ATP metabolism affects the heart more than it does other organ systems. The ischemic heart is leaking ATP constituents and cannot make it back fast enough. So you need to give agents that actually help make ATP.”
The key players, or the “Awesome Foursome” as he calls them, are magnesium, Co-Q10, L-carnitine, and D-ribose. Each plays a specific role in the Krebs cycle and other energy exchange processes, and combined, they are very synergistic.
Magnesium: This essential mineral is a co-factor for practically all enzymes involved in mitochondrial ATP production. It also has direct vasodilatory effects. In a sense, it is a natural calcium channel blocker, relaxing smooth muscle, lowering blood pressure, reducing arrhythmias, and alleviating angina. It can slow and normalize heart rate, so it is good for people prone to tachycardia. There’s evidence it can reduce symptoms associated with mitral valve prolapse.
Depending on a patient’s age, nutritional status and specific cardiovascular condition, Dr. Sinatra recommends between 400–800 mg of supplemental magnesium daily. He prefers chelated forms of magnesium, like orotate, glycinate or taurinate, which are better absorbed than the more common magnesium oxide forms.
Co-enzyme Q10: In addition to being an antioxidant, this compound is an electron “clearinghouse,” capturing electrons as they are spun out of the Krebs cycle, and passing them on to cytochromes in the electron transport chain. In short, Co-Q10 is a key facilitator of oxidative phosphorylation, the process by which ATP is built from adenosine monophosphate (AMP). Clinically, Co-Q10 can stabilize arrhythmias, reduce frequency and severity of angina, and improve heart function in people with diastolic dysfunction. It can also reduce mortality following MI.
Endogenous Co-Q10 production is based on the same biochemical pathway as cholesterol production, and it is equally inhibited by statin drugs. Tricyclic antidepressants also inhibit Q10. So patients on statins or TCADs are likely to be deficient in this critical co-enzyme.
For patients with stable angina, hypertension, intermittent arrhythmias, or diabetes/syndrome X, Dr. Sinatra recommends 180–360 mg of Co-Q10 per day; those with congestive heart failure, dilated cardiomyopathy and or other more severe conditions will need between 360–600 mg.
L-carnitine: This compound is the prime mover for ferrying fuel, in the form of fatty acid fragments, into mitochondria. Once inside the mitochondrial membranes, these two-carbon fatty acid fragments enter the Krebs cycle. Since fatty acids are the preferred myocardial fuel, this ability to transport them is especially important for healthy heart function. Dr. Sinatra noted that L-carnitine is characteristically deficient in people with ischemic heart disease, peripheral vascular disease, renal insufficiency, and lipid metabolic disorders.
Clinically, L-carnitine can ameliorate angina and claudication by optimizing the ischemic muscle’s ability to utilize whatever oxygen is being supplied. It also improves pump function in CHF patients. A massive European study (CEDIM-2), involving over 4,000 patients, is looking at whether carnitine given during acute MI can reduce myocardial damage and improve outcomes.
For stable but high CV risk patients, Dr. Sinatra gives L-carnitine at doses in the 1,000–2,000 mg range. For CHF or other advanced disease states, he pushes that up to 2,500 or even 3,000 mg per day.
D-Ribose: This 5-carbon sugar is the rate-limiting step formation of ATP, a unique triad consisting of an adenine nucleotide portion, a three-phosphate chain, and a pentose ring. That pentose ring is ribose. The body can make ribose from six-carbon sugars like glucose, but the process is inefficient by metabolic standards, and the enzymes required in the conversion are in short supply in most tissues.
In tissues with high ATP demand like myocardium and skeletal muscle, ribose stores are minimal, and the tissue depends on recycling of AMP and ADP to ATP for continued function. In prolonged ischemia, that process is impaired because these building blocks tend to be lost across the cell membranes.
In the absence of adequate ribose, the other myocardial support nutrients like Co-Q10 or L-carnitine will be of limited value, at least in generating the needed ATP. Supplemental ribose improves nearly all aspects of heart muscle function. For healthy people at elevated risk or those with mild disease, 5 grams per day is an adequate dose. Those with more severe disease should take 15 grams (5 g, thrice daily, mixed in juice).
Though it is a sugar, ribose is a glycemic-negative sugar, meaning that it cannot easily be converted into glucose, and does not stimulate an insulin response. In fact, ribose taken alone can actually lower glucose levels. For this reason, doctors who recommend ribose tell patients to mix the powder with orange juice, to ensure they don’t experience sudden drops in blood glucose.
After a few weeks on an “Awesome Foursome” protocol, many patients—even those with fairly advanced heart disease—show measurable improvements in heart function. Dr. Sinatra says he typically sees increased treadmill times, and delays of up to 1 minute in the onset of ST segment depression.
Ribose to the Rescue
Research on ribose goes back to the 1950s, but it was only recently that a supplemental form of D-ribose became available for wide clinical use. A company called Bioenergy developed and patented a process for manufacturing large quantities of D-ribose powder, which it markets as a bulk ingredient and also in its own line of Corvalen ribose supplements (www.corvalen.com).
Among the early adopters of ribose in cardiac care is David Perkowski, MD, a cardiothoracic surgeon at Saddleback Memorial Medical Center, Orange, CA. He uses it routinely before and after his surgeries and says it has profound positive effects on both heart function and clinical outcomes. (See related article from the current issue on our website, www.holisticprimarycare.net: Ribose Supplementation Improves Heart Surgery Outcomes.)
“The heart only has about 1 g of ATP at any one time, and it has to generate about 12 pounds of ATP every day! Any reduction in substrate will lead to a great reduction in the ability to generate needed energy.”
He noted that recurrent, repetitive angina and uncontrolled hypertension burn energy, and ischemic areas of the heart show marked decreases in energy production. As the myocardial cells burn ATP down to ADP and finally AMP, the constituent compounds become non-polar and are lost across the cell membranes. Which is why restoration of oxygenation following an ischemic episode will not necessarily restore full metabolic function. The limiting step is availability of ribose.
Dr. Perkowski operates on people with end-stage disease. But even in very sick patients, supplemental ribose can make a tremendous difference. “Cardiac output improves markedly when patients are on ribose. If a surgery is elective, meaning that it’s not an emergency procedure, I will keep patients on it for a week or two before the operation.”
CFS & CVD: It Takes Energy to Relax
Fibromyalgia and chronic fatigue syndrome are correlated with heart disease, said Dr. Sinatra. People with severe CFS have markedly increased incidence and mortality from cardiovascular events. Researchers at DePaul University, Chicago, found that heart failure was the most prevalent cause of death among a cohort of 166 recently-deceased CFS patients, the majority of whom were women (Jason LA, et al. Health Care Women Int. 2006; 27(7): 615–626). Orthostatic and hemodynamic instability are common in this population. “These conditions very definitely increase CV risk and they need to be taken very seriously.”
This makes sense when you consider that FM and CFS are disorders of energy metabolism, and a better understanding of ATP metabolism in muscle tissue helps explain why despite an overwhelming deficiency of energy, CFS/FM patients suffer intense muscle contraction and pain.
“It takes more energy to relax muscles than to contract them,” Dr. Sinatra explained. “Relaxation involves breaking the calcium bonds between the contracted muscle fibers, and it is an energy-dependent process. In FM/CFS, an individual does not have sufficient energy to break these bonds, as a result, they are in a state of chronic muscle contraction.” Increasing ATP production actually helps muscles relax, and that includes the myocardium.
Since nearly all physiological processes require ATP, one can begin to see how environmental and lifestyle factors fit together to compromise overall metabolic function. Someone who eats a lot of trans fats, is hyperinsulinemic, is under a lot of stress and is exposed to environmental toxins and cigarette smoke burns a lot of ATP to detoxify all of that. Inflammation, a critical factor in heart disease, causes a lot of tissue damage which requires repair, which also requires ATP. “You need to look at someone’s total energy cost,” said Dr. Sinatra.
He finds that when he treats heart disease patients using ATP-supportive nutrients, many other things also improve along the way. “It is very reliable. I’ve seen improvements in macular degeneration, memory problems, diabetes. I’ve actually had type 2 diabetics show improved glycemic control just from ATP-supportive therapy. Restore ATP and you restore health.” Dr. Perkowski says he’s seen similar collateral benefits.
Sometimes, this leads to drug-sparing. “I’m often able to get my patients off statins, diuretics, beta blockers, ACE inhibitors and other drugs. If we can’t get them off completely, we can usually lower the doses so they are taking less medication,” Dr. Sinatra said.
This can help offset the cost of the “awesome foursome,” which can run about $125 per month ($10 for magnesium, $25 for carnitine, $40 for Co-Q10, and $50 for ribose). That’s roughly the monthly cost of a prescription statin, the difference being that the drug would be at least partly covered by insurance while the supplements are not. All of the physicians interviewed said they routinely recommend fish oils, and some use vitamin K2, Hawthorn extract and other supplements, which can add to the total cost.
Dr. Surkin said he is certain that the tide of medical thinking will turn toward looking at how best to support myocardial recovery. The single-minded focus on lipids began to break down several years back as cardiologists began to recognize the role of inflammation. “It’s just that the LDL hypo–thesis has been around for a lot longer. But there’s good data to support Co-enzyme Q10, L-carnitine, Hawthorn, and ribose. The story is just emerging.”
Dr. Sinatra’s book, The Sinatra Solution: Metabolic Cardiology, is an exhaustively researched, well-referenced yet reader-friendly guide to the clinical application of the metabolic cardiology paradigm. Find it at www.basichealthpub.com. Both Dr. Sinatra and Dr. Surkin have formulated cardiovascular health product lines based on their analyses of the literature and their clinical experiences. Dr. Surkin’s Wellcor line can be found at www.cardiacwellness.com. Dr. Sinatra’s Advanced BioSolutions can be found at www.drsinatra.com.







