Correct diagnosis is the key to practicing good medicine. That sounds obvious, but in my experience, many of us do not make truly correct diagnoses. Why else would we have such high numbers of ill people in our country despite the huge amount of money we spend on “health care”?
Regardless of what specific problems my patients present, my goal is to facilitate a shift in the direction of autonomous homeostasis, and that almost bulletproof state of health we experienced in our youth. My own personal health experience, my work with pro-caliber athletes and with my patients has taught me that our health is intimately linked with our hormone levels. When hormonal levels are optimal, DNA is optimally transcribed, and autonomous homeostasis is better maintained and regained. Hormone levels start to decline around age 26–27, and susceptibility to illness starts to increase.
Health maintenance is like playing tennis. The point of strength for every tennis player is the center of the court. Every time s/he makes a return, s/he will try to get back to that point of strength. Each time s/he fails to get back to the center s/he loses a point (illness). If s/he fails enough times s/he loses (death). One’s health depends on the ability to get back to the homeostatic center even when life fires a 110 mph shot on one’s backhand side!
Diagnosing and treating hormonal imbalances is essential to good medical practice. You cannot have optimal muscle growth and repair without testosterone. You cannot facilitate growth and repair of brain neurons without estrogen. Without adequate cortisol, the immune system falters. The point is that returning your patients (or yourself) to optimal health depends on diagnosing and treating hormone imbalances.
Unfortunately, most of us depend almost exclusively on blood tests to detect hormone imbalances. Yet, deficiencies don’t show up in blood work until the patient is clinically in dire straights.
Nowhere is this need for accurate diagnosis more critical than with hypothyroidism. Because thyroid hormone plays a central role in energy metabolism and immune competence, and it synergizes with all other hormones, it is probably the most important hormone for maintaining homeostasis. You won’t make it back to the center of the physiologic court with low thyroid levels.
Regrettably, there are no lab tests that reliably diagnose hypothyroidism. Most physicians do their patients more harm than good by even ordering thyroid tests. It’s the odd physician that will treat a patient with normal lab values, even if the clinical picture screams “Hypothyroid!” Who wants to be labeled odd, right? Yet our patients continue to suffer.
If you understand the basics of thyroid physiology, you will understand the imperative to address hypothyroidism, and you’ll be better able to recognize it from what patients show and tell you.
Thyroid hormone underwrites transcription and assembly of glycoaminoglycans. These “water magnets” are building blocks for collagen. Without intracellular glycoaminoglycans, cells can’t retain water. Clinically, this manifests as dry, wrinkled skin, lusterless hair, brittle nails and the painful joints of osteoarthritis. Inability to hold water inside cells also results in fluid leakage into extracellular space. This presents as a rounded face, sub-orbital edema, leg edema, and a swollen/scalloped tongue.
Thyroid hormone assists insulin in moving glucose from the blood into cells. When thyroid levels are low, more insulin is needed to maintain normal glucose. More insulin means more fat cell hyperplasia, which shows up as increased fat deposition, especially around hips, thighs and abdomen (truncal obesity), all of which point to suboptimal thyroid levels.
Thyroid hormone is responsible for the strength of cardiac contractions, which, in turn, determines how much blood makes it down to the extremities. Low contractility manifests as a palpably reduced temperature in the feet and hands. The concomitant low oxygen state in the toes facilitates fungal overgrowth in nails and between toes.
The conversion of beta carotene into vitamin A is dependent on thyroid hormone. In a low thyroid state, conversion stagnates and beta carotene builds up, causing a yellow tint in palmar and plantar surfaces. The lack of immune-boosting vitamin A may lead to chronic respiratory, nasal, pharyngeal and ear infections.
Myxedema, the turgid accumulation of glycoaminoglycans, fat and extracellular water in the legs and arms, is pathognomonic of thyroid disease. This sign is only present in hypo- or hyperthyroidism. If you see it, there’s a thyroid issue, plain and simple.
The accompanying pictures are worth the proverbial thousand words. Learn to recognize them as reflecting hypothyroidism. You will see them in most patients because most chronically ill people have some level of thyroid compromise. The take-home lesson is to rely most heavily on what the patient and your head-to-toe physical exam tell you.
The book, Type 2 Hypothyroidism, by Mark Starr MD, has an excellent compilation of hypothyroid before-and-after treatment photos (www.type2hypothyroidism.com). It was my inspiration for starting to document clinical hypothyroidism. The endocrine volume of the Ciba Collection of Medical Illustrations by Frank Netter, MD, also has excellent illustrations.
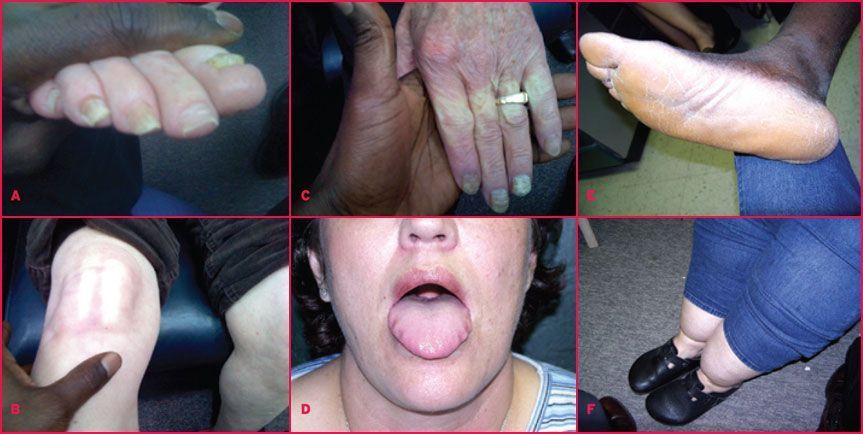 |
| A. Extensive fungal infection of the finger and toenails (onychomycosis) is often associated with hypothyroidism, a consequence of compromised cardiac contractility, leading to decreased blood flow to the extremities. The resulting low-oxygen state at the tips of the fingers and toes promotes fungal overgrowth. B. Slow capillary refilling, demonstrable by applying firm finger pressure to areas of thin skin, is a manifestation of reduced cardiac inotropy. As thyroid levels decline, cardiac contractility decreases. The worse this condition is, the closer to the heart it will manifest. It usually begins in the extremities, and patient will experience cold hands and feet. By the time it manifests above the knee, the patient has quite serious circulatory compromise. C. Poor capillary refilling, reflective of weak inotropy in the heart, leads to poor circulation at the extremities and facilitates fungal overgrowth in the nails. These signs are typical of longstanding hypothyroidism. D. Fluid leakage into extracellular spaces, a result of reduced glycoaminoglycan production also results in a characteristic swollen, scalloped tongue, which is very common in hypothyroid people. E. Conversion of beta-carotene to vitamin A is dependent on thyroid hormone. Thyroid deficiency will manifest as a yellowish buildup of carotene in the skin of the palms and soles. Poor circulation, also associated with hypothyroidism, facilitates fungal overgrowth between toes. F. Thyroid hormone drives production of glycoaminoglycans, responsible for keeping water inside cells. In hypothyroidism, water tends to leak into extracellular spaces causing significant edema, easily recognized around the legs and ankles. Photos: Roby Mitchell, MD, reproduced with permission. |
Roby Mitchell, MD, aka Dr. Fitt, is a family physician currently practicing orthomolecular and nutritional medicine with Jonathan Wright, MD, at the Tahoma Clinic, Renton, WA. He is a graduate of Texas Tech University School of Medicine, as well as the US Marine Corps Officer Candidate School.







