Technology continues to redefine nearly every aspect of our personal and professional lives. Smart phones, tablet computers and the applications they support are changing not only the frequency with which we access and utilize information, but also how we relate to and internalize that information.
If you own one of these devices—and most doctors do–you know firsthand how they’ve shaped your personal and professional life. Even if you don’t own one, it’s hard not to be aware of the conveniences they afford and the changes they have made, especially in health care.
shaped your personal and professional life. Even if you don’t own one, it’s hard not to be aware of the conveniences they afford and the changes they have made, especially in health care.
Within nine months of Apple’s first iPad release, nearly a quarter of physicians were using them in their practices.
A Pew Internet study conducted in 2010 indicated that 17% of all 18-29 year olds had a health-related app on their phones – nearly twice as many as those in the 30-49 age group. Given that our need for health information generally increases with age, we can expect these percentages to grow markedly in the next decade as today’s app-enabled young adults start to feel the effects of time.
The question is not should physicians engage with mobile technology, but how and to what extent?
Smart Phones, Smarter Docs
At the apex of the smart-med revolution is IBM’s Watson computer system, currently being evaluated for its acumen in diagnosing cancer. Most apps available for mobile phones and tablet computers are a good bit more humble, but they certainly have a lot to offer.
There’s a rapidly evolving field of applications that can facilitate the practice of medicine, and that the FDA actually regulates as medical devices. There are apps that can act as online storage mechanisms where patients and practitioners can both access radiology images (like Mobile MIM for example). There are apps like AirStrip that allow you to monitor patient vitals from a distance. There are even iPhone apps like ePetri that take repeated pictures of a Petri dish so it needn’t be removed from its incubator.
Since it takes FDA approval to be considered a medical device, this category of apps is the only one subject to much regulation and quality control. You are most likely to encounter apps like these if you work in a hospital system or network that advocates telemedicine. Though these and many other apps are free for download, they are ineffective if not used with the necessary software that needs be purchased by the establishment.
There’s also a whole world of medical and health related apps that are not specifically marketed for patient care but are nonetheless useful in medical practice. Since these are not considered medical devices, they are not nearly as thoroughly regulated as the previous category.
Practitioners and medical students alike can access a host of reference apps that simply provide information: medical dictionaries (for both conventional and alternative health information), diagnosis and billing code guides, anatomical references, drug interactions databases, and PubMed reference guides.
There are also dozens of apps created to help screen or diagnose patients. As with any online diagnostic tool, these ought be used to assist and not to replace the medical practitioners’ clinical judgment.
“Doctor, My iPhone Says….”
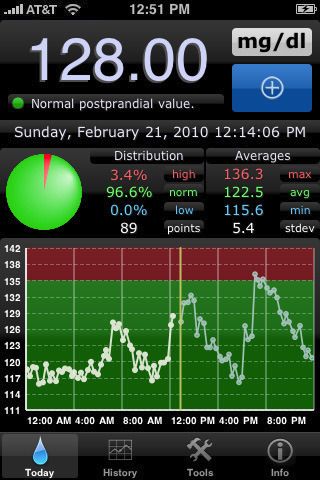 Whether or not you’ve waded out into the sea of health apps, odds are good that some of your patients have! The vast majority of offerings in the medical and health and fitness sections of iTunes are actually for consumers. So, you might be wondering, “What sort of information are my patients receiving? Where are they getting it? Are they helpful? Are there any risks? How do I help my patients find good apps?”
Whether or not you’ve waded out into the sea of health apps, odds are good that some of your patients have! The vast majority of offerings in the medical and health and fitness sections of iTunes are actually for consumers. So, you might be wondering, “What sort of information are my patients receiving? Where are they getting it? Are they helpful? Are there any risks? How do I help my patients find good apps?”
The majority of apps help consumers do one of two things: obtain health information or track their own health measures. Examples of the former include:
• Epicurious, a recipe app which can be tailored for dietary restrictions.
• MyAllergies Food Diary, which provides food allergy information.
• Is That Gluten Free, and Food Additives which help food-sensitive people assess which foods to avoid.
• Daily Yoga, one of a host of yoga-related apps that can guide people through daily yoga routines.
• My Plate and My Diet Steps, which give people serving size guidelines.
• Daily Workouts, and other exercise-related apps that, like the yoga apps, lead people through 10-30 minute fitness routines.
• iTherapy and Healing Foods, which offer information on complementary, alternative and integrative health care.
• Meal Snap, a food scanning app that can calculate caloric and nutrient composition of a food the user photographs with his/her mobile phone.
Apps that track the user’s health information include:
• Daily Burn, which tracks calories.
• Insight Timer—daily meditations.
• iPeriod—menstrual cycles.
• Weight Watchers App—weight changes over time.
• BGluMon—blood sugar.
• iBP Blood Pressure—blood pressure changes.
• My Quit Coach—cigarette consumption & quit adherence produced by the LIVESTRONG organization.
• BrainWave Headache Relief—headache frequency.
Beyond these fairly basic tools, there’s a host of apps that blend the aforementioned categories. A few recent innovations that caught my eye are:
• Sing Fit – an app created by music therapists that allows users to more easily get the health benefits and pleasures of singing by enabling them to change pitch and tempo of the backing music for their favorite songs.
• ZeoMobile–this app, along with its lightweight headband, allows people to track REM sleep throughout the night.
• Mosquito Buster—a tool that allegedly emits a high-pitched noise that wards off mosquitoes but is undetectable to the human ear.
• Simply Being–a highly rated guided meditation application.
All of these apps are termed consumer convenience applications, the FDA’s only other apps category next to medical devices. Regulation is not nearly as stringent as for apps considered medical devices, so a patient’s enthusiasm for health apps should be balanced with healthy doses of critical thinking and due diligence.
apps category next to medical devices. Regulation is not nearly as stringent as for apps considered medical devices, so a patient’s enthusiasm for health apps should be balanced with healthy doses of critical thinking and due diligence.
Health-focused apps can be handy, even fun, as people gain knowledge and keep track of their own health indicators. They also have great potential for information sharing among large numbers of consumers. This can be seen as both a positive or negative cultural development.
On an individual level, rapid access to information and experience from a worldwide virtual community is extremely beneficial when someone needs to learn about a particular disease, condition or therapy. Apps that support tracking of specific medical information can also facilitate sharing of that information between patient and practitioner(s), which is clearly a good thing.
With a doctor’s advice, patients who aren’t yet personally invested in making behavioral changes can use apps to chart their health behaviors. This sometimes renders them more reflective and engaged. Wide and rapid sharing of information can enable you as a doctor to easily introduce patients to alternative therapies such as music, yoga or meditation through the use of applications.
New Tech, New Benefits, New Risks
As with all technological innovations, there can be downsides. The risks of mobile health apps fall into three major categories:
• Susceptibility to a virus that could steal personal information – medical and otherwise
• Breach of confidentiality when personal health information is transferred between patient and practitioner
• Misinformation
A virus can be inadvertently downloaded if an otherwise legitimate app is recreated with malicious code. The FDA does not monitor apps for consumer convenience and, for that matter, neither does anyone else.
The best bet against downloading a malicious recreated app and/or virus is to purchase only from secured sources (iTunes for Apple, Google Apps or Amazon for Android phones) or directly from the company’s website (assuming you trust the company creating the app). Advise patients to avoid pop-up prompts that encourage them to download apps.
 Concerning breach of confidentiality, HIPAA does not directly address information exchanged via mobile and tablet apps in its privacy laws. Actually, the use of apps for exchange of medical information is still a legal gray area. That said, common sense should tell you that the repercussions if someone hacks your phone containing patient information could be devastating and could extend far beyond individual identity theft, so be sure you follow your own advice!
Concerning breach of confidentiality, HIPAA does not directly address information exchanged via mobile and tablet apps in its privacy laws. Actually, the use of apps for exchange of medical information is still a legal gray area. That said, common sense should tell you that the repercussions if someone hacks your phone containing patient information could be devastating and could extend far beyond individual identity theft, so be sure you follow your own advice!
The American Medical Association includes the following disclaimer on its My Medications app (used for tracking the medications one is taking and for sharing that information with one’s medical providers):
“When you purchase this application, you will be responsible for protecting the privacy and security of the information that you enter, and for deciding who to disclose, and give access to, the information. The AMA assumes no responsibility, and shall have no liability, for protecting the privacy or security of the information entered in the application or shared with others either intentionally or unintentionally.”
This is a good reminder that once private information is stored on a mobile app, it is the device owner’s responsibility to protect that information. Anytime a patient shares information with a practitioner or charts it through the use of an app, s/he runs the risk of having that information compromised.
Encourage patients to check an app’s privacy policy to see whether it allows the company to share a user’s personal information with advertisers. It’s also a very good idea to remind patients to transfer personal information only over secured networks.
As for the risk of misinformation, that’s a problem as old as the practice of medicine itself. Practitioners have always been concerned that patients will find and follow flawed information. But in lieu of other mandates, the veracity of apps and the information they provide–medical and otherwise—is largely being verified by social media in the form of consumer reviews and ratings.
Scary as it may seem, determining validity through crowd-sourcing is becoming more and more common. A recent study showed that users who found medical information on youtube.com believed it to be significantly more reliable than that found on a nondescript website. Needless to say, what is considered “trustworthy” is changing with advances in information, technology and social media.
The role of practitioners is also changing. No longer are clinicians the gatekeepers to medical information. For much of the last 20 years, anyone with Internet access and the wherewithal to read it can educate themselves with up-to-date medical knowledge. What practitioners need to provide today is help in navigating through the onslaught of available medical information (both good and bad, safe and unsafe).
This is the true meaning of patient-centered medicine – a relationship in which both practitioner and patient synthesize information and contextualize it to create the most effective medical plan for each individual. Health apps can be a helpful part of this process. As with drugs, supplements and nutritional advice, your opinion as a physician still counts! Patients will appreciate your recommendations on health apps you’ve personally tried and found valuable. At their best, health-related apps facilitate better practitioner/patient communication, but they can certainly never replace it.
END
Sarah Showalter, MA, is a corporate health coach who conducted her thesis on how social media influences a user’s perception of online alternative health information.








