Zonulin, an endogenous protein that regulates the size of intestinal tight junctions, could be useful as a serum marker for non-celiac gluten sensitivity—a condition that has been the subject of much controversy in recent years.
People fitting the clinical picture of non-celiac gluten sensitivity show circulating zonulin levels four times higher than healthy control subjects, reported Dr. Giovanni Barbara of the University of Bologna.
Speaking at the 23rd United European Gastroenterology Week in Barcelona, Dr. Barbara also noted that patients with celiac disease showed a nearly five-fold elevation in serum zonulin. Those with irritable bowel syndrome showed levels that were just shy of two times greater than in healthy people.
Initially discovered 15 years ago by Alessio Fasano and a team he headed at the University of Maryland, zonulin is produced by intestinal cells and regulates the permeability of the intestine by modulating the size of the gaps between intestinal cells. It also regulates passage of nutrients and water and into and out of the gut.
Excessive zonulin production is triggered by a wide range of bacterial 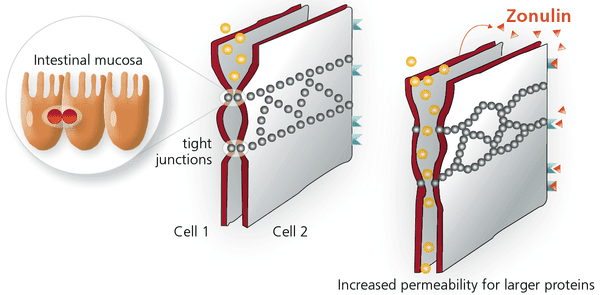 pathogens as well as food allergens, including gluten. When zonulin production rises, so does intestinal permeability.
pathogens as well as food allergens, including gluten. When zonulin production rises, so does intestinal permeability.
“Increased intestinal permeability has been implicated in a range of autoimmune conditions including celiac disease, type 1 diabetes, rheumatoid arthritis and multiple sclerosis,” Dr. Barbara said.
He believes the molecule—which is easily measurable in serum– is over-expressed in all disorders in which tight junction dysfunction is central.
A Landmark Study
In the current study, which has not yet been published, Dr. Barbara and colleagues measured serum zonulin in 15 healthy volunteers, as well as 15 patients with confirmed celiac disease, 15 with diarrhea-predominant IBS, and 27 with non-celiac gluten sensitivity (NCGS).
The latter group represents patients who do not show the classic tissue changes or immunologic signs of celiac disease, but whose symptoms appear to be connected with gluten exposure, and who show improvement when following a strict gluten-free diet.
Dr. Barbara’s team calculated that the mean circulating zonulin level in the control group was 0.007 ng/mg. Among those with frank celiac disease it was 0.033 ng/mg, and among those with NCGS it was 0.030 ng/mg. The authors note that in the latter group, zonulin levels dropped significantly when the patients practiced strict gluten avoidance.
“We were intrigued to find that blood levels of zonulin were almost as high in patients with NCGS as in those with celiac disease,” Dr. Barbara said at the UEG Week meeting.
The findings provide objective support for the reality of a condition that some clinicians and researchers dismiss as a questionable or contrived diagnosis. The dismissal has been based, in part, on the fact that there were no reliable biomarkers definitively associated with the condition.
Immunologically, people fitting the NCGS pattern usually do not show the anti-tissue transglutaminase antibodies seen in those with celiac disease; roughly half show anti-gliadin IgG antibodies.
Dr. Barbara’s work, along with continued studies by Dr. Fasano, now at the Massachusetts General Hospital, points to zonulin not only as a key for understanding the pathophysiology of gluten sensitivity but as a practical diagnostic marker for this and other diseases characterized by intestinal permeability.
While it is too soon to posit zonulin testing as a definitive diagnostic tool, Dr. Barbara believes it is a worthy direction for future research.
“Hopefully, our work will lead to new diagnostic and therapeutic strategies for patients with these and possibly other autoimmune conditions.”
END







