Vitamin D is an essential precursor to hundreds of enzymes and proteins. It is not an overstatement to say that this vitamin affects everything from our DNA transcription to our moods.
The active form allows our cells to read DNA instructions more effectively. It also helps to regulate vital components of neurotransmitters (ie serotonin) and hormones. It is essential in mineral metabolism and is a major determinant of bone strength, regulating absorption and transport of calcium, phosphorus, and magnesium for bone mineralization and growth. Vitamin D also aids muscle and nerve function.
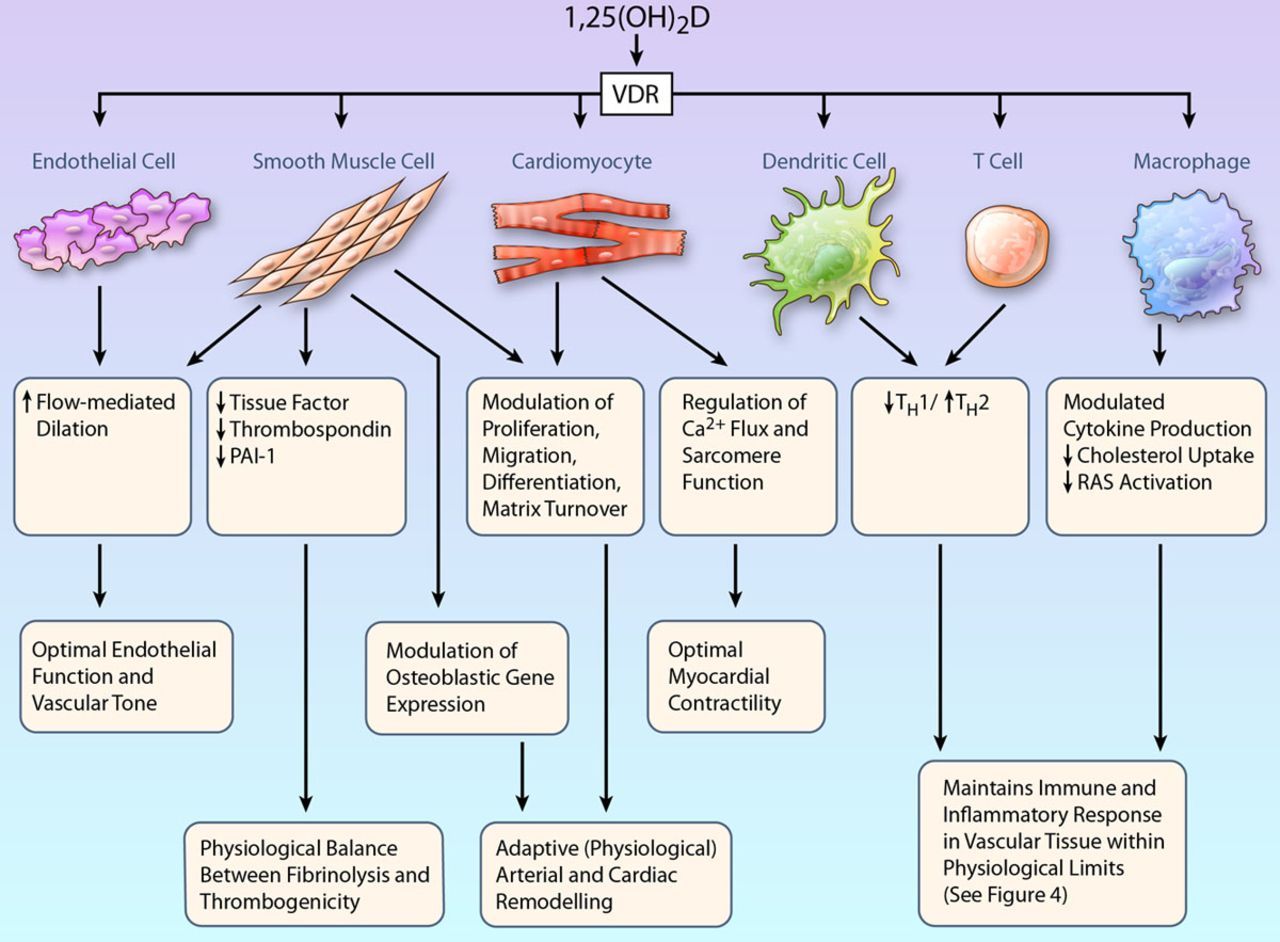 New research continues to shed light on vitamin D’s myriad physiological functions, and a recent wave of studies shows the ways in which deficiency contributes to autoimmunity, urinary incontinence in elderly, pregnancy loss, and heart disease.
New research continues to shed light on vitamin D’s myriad physiological functions, and a recent wave of studies shows the ways in which deficiency contributes to autoimmunity, urinary incontinence in elderly, pregnancy loss, and heart disease.
Vitamin D deficiency–arguably the most common deficiency in adults and children in the developed world–underlies many chronic conditions. Optimizing vitamin D should be an important clinical focus, as we strive to help our patients improve their overall health and wellness.
Heightened Havoc
A literature review published last year shows clearly that vitamin D deficiency is associated with increased inflammation and the pathophysiology of autoimmune conditions like multiple sclerosis, autoimmune thyroid diseases, primary biliary cirrhosis and scleroderma (Rosen Y, et al. Scand J Rheumatol. 2016;45(6):439-447).
Another 2016 study published in the European Journal of Clinical Nutrition, highlighted the inverse relationship between serum 25-hydroxyvitamin D and the severity and frequency of relapses in multiple sclerosis patients.
Simply put, in a cohort of 184 patients with relapsing-remitting MS who were receiving immune modulating drugs but no vitamin D supplements, the lower the serum vitamin D, the greater the number of relapses.
The investigators took 25(OH)D measurements in February and August 2014, along with the assessments of MS-related disability levels. When the researchers looked at 25(OH)D levels against the occurrences of relapses and the level of disability, the correlations were very clear across the seasons. In both winter and summer, serum 25(OH)D levels were lower in the patients with relapses than in those without (Brola W, et al. Eur J Clin Nutr. 2016;70(9): 995-9).
Increased Risk of Miscarriage
Numerous studies have linked vitamin D deficiencies to pregnancy complications including preeclampsia, gestational diabetes, bacterial vaginosis and compromised uterine growth. A study published last Fall documents an association with pregnancy loss.
Investigators at Xi’an Jiaotong University, China, collected plasma from 60 women at 7-9 weeks gestation (30 with successful pregnancy history and 30 with one or more previous first trimester pregnancy losses). They also looked at serum from 60 non-gravid women of childbearing age (30 who’d carried pregnancies to term, and 30 with first trimester losses).
They found that women who were able to carry their pregnancies to term generally had higher serum 25(OH)D levels than those who’d had miscarriages (49.3 vs 34.5 ug /L). Low vitamin D status was far more prevalent among the women who’d suffered pregnancy losses compared with those who had normal pregnancies (Hou W, et al. Eur J Clin Nutr. 2016 Sep;70(9):1004-8).
A Toll on the Old
Further along the lifespan, vitamin D deficiency raises the incidence of urinary incontinence (UI) in older adults, according to a prospective study published last year in the European Journal of Clinical Nutrition.
The University of Alabama at Birmingham Study of Aging involved 350 community-dwelling Medicare enrollees with a mean age of 74 years. Researchers tracked the incidence of UI every 6-12 months for up to 42 months.
At baseline 54% of the cohort was vitamin D deficient, with 25(OH)D levels less than 20 ng/ml, and an additional 25% were classified as insufficient, with 25(OH)D levels under 30.
This study showed a clear association between low vitamin D and the cumulative incidence of UI: 38% of those who were deficient at baseline, and 45% of those who were insufficient, had developed UI within the 42-month study period. In comparison, only 23% of those with adequate 25(OH)D levels had UI during the same period.
After adjusting for age, gender, race and ethnicity, the authors conclude that vitamin D insufficiency conferred an odds ratio for UI of 3.18, and frank deficiency conferred an odds ratio of 2.47 (Vaughan CP, et al. Eur J Clin Nutr. 2016;70(9):987-9).
The authors note that there are receptors for vitamin D in the bladder and the striated muscle of the pelvic floor, and suggest that incontinence may be a consequence of weakened muscle function caused by the deficiency.
“Vitamin D is a low cost, well-tolerated supplement and could provide an adjuvant treatment to currently recommended exercise-based behavioral therapy,” they write.
Taking the Pressure Off
The association between vitamin D and heart health has been well established. A new study presented at this year’s National Kidney Foundation Spring Clinical Meeting elucidates the relationship between this vitamin and blood pressure. It suggests that vitamin D, along with calcium, has a role in keeping blood pressure in check.
A team of researchers at the University of San Francisco and Loyola University analyzed data from 24,844 healthy adults (mean age 37.5 years) who participated in the National Health and Examination Survey (NHANES) from 2001-2006. The subjects had all completed dietary questionnaires and had a physical exam.
After controlling for a variety of demographic variables, they found a consistent inverse relationship between vitamin D status and systolic blood pressure. As 25(OH)D levels increased, systolic blood pressure decreased significantly, even after accounting for calcium intake. Self-reported calcium intake also showed an independent pressure-reducing effect.
Interestingly, the authors did not find a relationship between diastolic pressure and serum vitamin D levels (Bean S, et al. National Kidney Foundation 2017 Spring Clinical Meeting, Poster 306).
These findings are clearly not definitive: they are based on epidemiological data, and show only correlations not direct causal effects. However, the size of the population analyzed gives the study considerable weight.
Bean and colleagues did not evaluate the potential impact of supplementation, so unfortunately their trial does not shed new light on the question of whether we can help lower blood pressure by supplementing with vitamin D
Two years ago, European researchers published a systematic review of 46 small trials and came to the conclusion that the answer to this question is a big, fat “No.”
Louise A. Beveridge, from the University of Dundee, and colleagues aggregated data representing more than 4,500 patients. Overall, they found that vitamin D supplementation had no effect on systolic or diastolic pressure. Moreover, they could not identify any baseline factors that could predict a better response to vitamin D therapy (Beveridge LA, et al. JAMA Internal Medicine. 2015; 175 (5): 745-754).
But this doesn’t mean their verdict is final. Just as Bean’s positive findings are far from definitive, so is Beveridge’s negative assessment. The authors readily acknowledge that the metanalysis suffers from the common limitations of projects of this kind: small sizes of the trials under review, divergent protocols, variable quality, differences in baseline characteristics and outcome measures.
Further, they recognize that many of the trials they reviewed may not have provided high enough vitamin D doses to  engender a measurable anti-hypertensive effect.
engender a measurable anti-hypertensive effect.
“Levels of more than 30 ng/mL have been postulated as necessary for optimum health… Levels of vitamin D supplementation required to reach such levels vary widely depending on age, sex, obesity, and baseline 25OHD levels; doses ranging from 1,600 to more than 5,000 IU/d have been advocated as necessary. Most doses studied in this review were at or below the lower end of this range.”
What’s the Optimal Range?
The “more than 30 ng/mL” serum level cited in Beveridge’s comments is a common benchmark in the clinical literature. In practice, most holistic and functional medicine practitioners like to see serum vitamin D in the range of 50-80 ng/ml.
The reality is, many patients are far from even the bottom end of the healthy range.
If looking for a natural way to optimize vitamin D, you will need exposure of at least 40% of total skin surface to the sun just until it turns pink or one shade darker, noon- 1pm is the best time. A mineral based sunscreen can optimize conversion. Foods rich in vitamin D include: sea vegetables, fish, beef liver, some cheeses, portabella mushrooms, and egg yolks.
Be aware that increasing vitamin D intake can create a relative insufficiency of vitamins K, A, and E. Vitamin K2 or MK7 is needed for vitamin D to work effectively. Taking large amounts of vitamin D probably won’t do much if the K2 level isn’t also increased. Cod liver oil provides vitamin A, D3, and to a lesser extent, vitamins K, E, and DHA.
While vitamin D is generally safe, even at high doses, we do need to be careful when treating people who have hyperparathyroidism, Hodgkin’s or non-Hodgkin’s lymphoma, granulomatous diseases like sarcoidosis and tuberculosis, kidney stones or other kidney disease, and liver disease.
END
Madiha Saeed, MD is a holistic family physician in Naperville, IL. She trained at National University of Science and Technology and completed her residency in 2010 at St. Joseph Regional Medical Center. She is board certified in both Family Medicine and Integrative Holistic Medicine, and has a particular passion for women’s’ health and family health issues. A busy mother of four young boys, Dr. Saeed shares her “walk the talk” nutrition & lifestyle tips and her lively “bring it on” spirit with families worldwide via her HolisticMomMD website, and her forthcoming book, “The Holistic Rx: Every Patient’s Guide to healing and Preventing Chronic Disease.”







