Could cannabis be the solution to America’s opioid overdose epidemic? Mounting evidence indicates that medical marijuana may help save lives by reducing prescription painkiller misuse.
With opioids coming under intense scrutiny, and the hazards of long-term NSAID use becoming more apparent, patients and clinicians alike are finding themselves with a dwindling set of tools for managing chronic pain.
But a budding trend suggests that cannabis and its derivatives can be effective analgesics. Pain associated with inflammation, headaches, neuropathy, muscle damage, spinal injury, and fibromyalgia are among the most common reasons for cannabis prescriptions.
As of the November 2016 election, 28 states and the District of Columbia have legalized the use of marijuana for medicinal purposes. Yet marijuana legalization remains one of the most controversial policy issues brought forward in recent decades. The controversy stems in part from the fact that while it’s now legal in some form in more than half the country, marijuana is still classified on the federal level as an illegal substance. Under the FDA’s Controlled Substances Act (CSA) of 1970, the Drug Enforcement Administration lists cannabis as a Schedule I substance, placing it in the CSA’s most restrictive drug category.
Schedule I drugs — which also include heroin, LSD, and ecstasy — are characterized by their high potential for abuse, lack of accepted medical applications, and safety concerns even when used under medical supervision.
Compared with cannabis, many legal painkilling drugs have a far greater potential to cause harm and to engender abuse. Prescription opioid use — and abuse — is currently at an all-time high in the US. The sales of prescription opioids — whose side effects include physical dependence and addiction — have quadrupled since 1999, according to the Centers for Disease Control and Prevention (CDC). Analgesics now rank as the second most prescribed class of medications nationwide.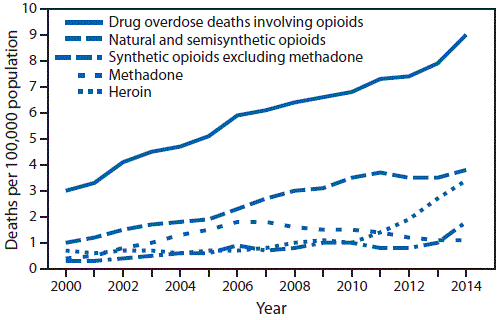
Paralleling the upsurge in prescription painkiller sales, are surges in the rates of opioid abuse and overdose deaths. Opioids — including both prescription pain relievers and heroin — killed over 28,000 Americans in 2014, more than any other year on record. Emergency department visits involving the misuse or abuse of prescription opioids jumped a massive 153% between 2004 and 2011 (Compton, W. et al. N Engl J Med. 2016; 374(2): 154-163).
The CDC estimates that today, at least half of all opioid overdose deaths involve a prescription analgesic.
In contrast, the likelihood of a marijuana overdose is extremely low. While occasionally listed as a secondary cause contributing to patient fatalities, cannabis overdose alone has never once been implicated as the primary reason for an individual’s death.
Cannabis Laws Reduce Opioid Use
Recognizing the gravity of America’s prescription drug abuse crisis, clinicians, politicians, and even popular recording artists are calling out for lifesaving fixes to the opioid epidemic. A body of epidemiological research points to cannabis as one promising answer to their calls.
Several studies conducted over the last few years indicate that in states where medical marijuana has been legalized, painkiller prescriptions — and subsequently, opiate overdose rates — have fallen substantially.
A 2014 report published in JAMA Internal Medicine showed a strong association between legalization of medical cannabis and lower state-level opioid overdose deaths. Data collected between 1999 and 2010, when only 13 states had legalized medical marijuana, showed that cannabis-friendly states had a 24.8% lower mean annual opioid overdose mortality rate (95% CI, −37.5% to −9.5%; P = .003) compared to states where marijuana wasn’t legal.
The researchers also showed that the association between legalization of medical cannabis and lower overdose mortality generally strengthened over time. The longer a state’s medical cannabis laws had been in effect, the larger the drop in opioid-related deaths (Bachhuber, M. et al. JAMA Intern Med. 2014; 174(10): 1668–1673).
Another more recent study, published earlier this year in the journal Health Affairs, showed similar findings. Challenging a common argument that only young individuals are interested in medical marijuana, investigators looked at data from all prescriptions filled by Medicare Part D enrollees to treat nine different clinical conditions between 2010 and 2013.
In states with medical cannabis laws, the use of FDA-approved pharmaceuticals for which marijuana could serve as an alternative fell significantly. The only exceptions were for spasticity- and glaucoma-related drugs, which continued to be prescribed at similar rates before and after medicinal cannabis legalization.
“Our findings and existing clinical literature imply that patients respond to medical marijuana legislation as if there are clinical benefits to the drug,” the researchers write, arguing that their data provide not only key insights into the impact of cannabis laws on prescription drug use, but also important evidence of marijuana’s outdated status as a Schedule I substance (Bradford, A. & Bradford, W. Health Aff. 2016; 35(7): 1230-1236).
The Bradford team note that in addition to its clinical merits, cannabis legalization may offer economic benefits to states where the herb is used medicinally.
Nationally, the Medicare program and its enrollees spent an estimated $165.2 million less in 2013 as a result of the changed prescribing behaviors induced by medical cannabis legalization. Greater budgetary relief could follow a more widespread approval and acceptance of medical marijuana as a legitimate form of therapy. The Bradfords argue that their study has implications extending beyond clinical practice, and into the evolution of medical marijuana policies at the state and federal levels.
Which is the Real Gateway Drug?
Since its legalization in many parts of the country, some have been quick to condemn the dangers of unregulated cannabis use.
A widely publicised case report documenting the death of a teenager in Colorado who fell from a balcony after eating an edible marijuana product led to concerns about marijuana over-consumption and physical safety endangerment. Impaired driving ability is another widely-cited cannabis critique. National studies currently provide conflicting evidence on the impact of marijuana use on traffic fatalities. The data are equivocal, and it is still an open question whether or not states with medical marijuana laws have higher traffic fatality rates (Ghosh, T. et al. N Engl J Med. 2015; 372(11): 991-993).
Another common criticism of marijuana is that it can act as a gateway drug, leading users down a path towards more dangerous substances. The same criticism, however, can also be made for prescription painkillers.
The reality is that pharmaceutical opioid abuse can–and often does–open the door to future heroin use. The National Institute on Drug Abuse reports that nearly half of young heroin users surveyed in three recent studies had abused prescription opioids before starting to use heroin. Some reported switching to heroin because it’s less expensive and easier to obtain than pharmaceutical drugs.
Cannabis, on the other hand, may assist users in reducing their consumption of nonmedical opioids.
Researchers examined cannabis consumption among 653 injection drug users in the cities of Los Angeles and San Francisco, and found a statistical association between recent cannabis use and lower frequency of nonmedical opioid use. According to participants’ survey responses, the mean and median number of times individuals used opioids in the previous 30 days were significantly lower among those who used cannabis than those who had not (Kral, A. et al. Drug Alcohol Depend. 2015; 153: 236–241).
Further research on cannabis as an analgesic is clearly warranted. But the reality is, advocates for this green movement are not waiting for definitive data, and neither are the hundreds of thousands of people using cannabis for medical purposes.
The favorable results from studies so far suggest marijuana is a pain treatment option worth exploring. Its potent analgesic properties, limited side effects, and the near impossibility of a cannabis overdose merit consideration.
To be sure, there are number of important questions still to be answered about dose standardization, the risks and benefits of combined cannabis and opioid treatment, and the best ways for practitioners and patients to communicate about cannabis and other controlled substances. These are, “all issues that deserve attention as we better understand the role of medical marijuana in the treatment of patients with chronic pain” (Becker, W. & Tetrault, J. Mayo Clin Proced. 2016; 91(7): 830–832).
END







