Most scientific research portrays the kidneys as victims of high blood pressure. Yet, the evidence and good logical thinking suggest that kidney disease can act as the “perpetrator” in hypertension.
Though we in medicine commonly use the term “essential” hypertension, the truth is there is little that is essential about high blood pressure: it is a vital sign indicating that something has gone vitally wrong.
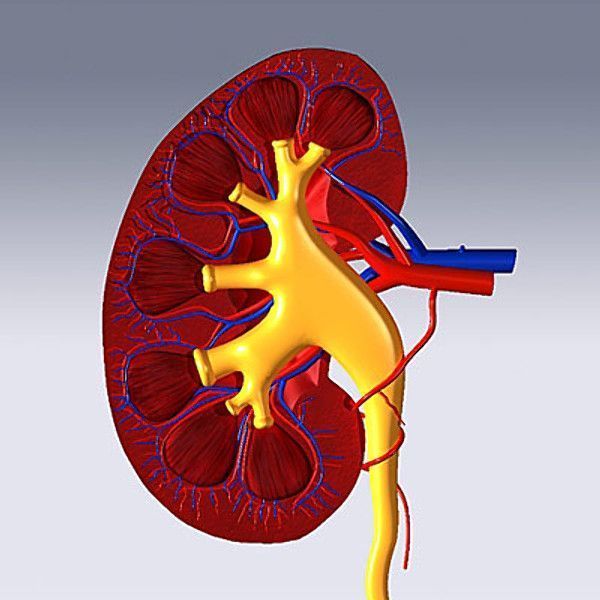 Consider this: the kidneys, at less than 1% of body weight, account for more than 20% of cardiac output. They require a significant blood supply in part due to their role in filtration and hormone production. These are vital organs. When something is amiss in the kidneys, it will show up in the vital signs.
Consider this: the kidneys, at less than 1% of body weight, account for more than 20% of cardiac output. They require a significant blood supply in part due to their role in filtration and hormone production. These are vital organs. When something is amiss in the kidneys, it will show up in the vital signs.
Decreased renal blood flow (RBF) can be one such problem.
When the glomerulus detects poor RBF, the glomerular granular cells release renin, leading to an elevation in blood pressure to ensure adequate perfusion of renal cells.
Early Detection Tips
Assessment of early kidney damage (i.e. renal insufficiency or stage 1 CKD) and mitigation of risk factors for kidney damage may prevent progression or development of high blood pressure.
Unfortunately, most patients are not diagnosed with any form of kidney disease until they are at a stage of significant dysfunction, usually stage III or beyond. This is not an ideal situation because at that point, we must be much more cautious in making dietary and supplement recommendations.
Part of the problem in diagnosing early-onset kidney disease is that even with a loss of up to 50% of renal cell function, GFR can be maintained within normal parameters; the dysfunction simply will not show up in the GFR measurements until a much later stage. This is part of the reason the diagnosis of stage 1 kidney disease is not based on GFR.
Though we lack precise diagnostic tests for early stage disease, there are some early indicators of poor renal function.
Consistent nocturia is often the only symptom of early kidney disease, though it is admittedly non-specific.
In addition, high-normal serum creatinine or creatinine that appears to be rising over time (in the absence of dehydration or other factors) and elevated cystatin C also indicate dysfunction at earlier stages. Serum cystatin C elevation antecedes microalbuminuria and also appears to be more accurate in indicating early stages of chronic kidney disease than serum creatinine. Urinary cystatin C is also being studied as a marker of renal ischemic injury.
Whether you see it as the chicken or the egg – the kidney affects and is affected by blood pressure changes. At any stage of high blood pressure, the kidneys will need support.
Starting Points for Kidney Support
Frequent NSAID use, alcohol abuse, smoking, and recreational drug use have all been proven to be directly nephrotoxic and to adversely affect blood pressure. Begin the process of mitigating and reversing kidney problems by discussing these risk factors with patients.
Once you rule out secondary hyperparathyroidism and other relevant differential diagnoses, it makes sense to focus on slow, measured weight loss if the patient is overweight. This has been proven to both improve serum creatinine and reduce blood pressure concurrently.
Part of this recommendation is moderate exercise. Aquatic exercise and daily walking have both been proven to improve GFR. Goal body fat should be less than 25% for men and 35% for women.
The second therapy I recommend is stress support. Stress and catecholamine injury have been directly correlated with high blood pressure and kidney damage. Stress is almost always a part of the equation in this patient population, and may manifest less obviously in patients who prefer not to discuss emotional stressors.
The ways of addressing stress are myriad, but one specific nutrient I recommend is Black Currant oil. That is because it is a very rich source of gamma linolenic acid, an essential omega-6 fatty acid that promotes healthy eicosanoid production. GLA is essential for optimal renal blood flow and can offset the effects of stress. The reason that NSAIDs, corticosteroids and stress (i.e. cortisol) are so damaging to the kidneys is in part because they block this pathway, which is vital for vasodilation.
The third therapeutic direction I strongly recommend is treating the gastrointestinal tract. This usually includes probiotic therapy, which can be in the form of fermented foods or probiotic supplementation. Research supports supplementation with lactobacillus species due their ability to decrease blood urea nitrogen by metabolizing nitrogenous compounds.
There are many more strategies to support healthy blood pressure levels and optimal kidney function but these are the approaches I’ve found to be generally safe and highly effective. In addition, they are foundational to any other therapy. No prescription–natural or otherwise–will go very far in patients who are not at a healthy weight, digesting properly, and finding ways to release stress.
END
Anne Williams, ND LAc practices at Rochat Holistic Health in New York City’s West Village. She specializes in women’s health and heart disease. Dr. Williams has no financial conflicts of interest to disclose.







