Because it is inherently an individualized form of therapy, acupuncture remains notoriously difficult to study in the context of a “classic” randomized controlled trial.
Do not use that as a reason to dismiss it, though. It is not without reason that the practice continues to draw attention from the public and from researchers worldwide. This ancient, therapy remains a useful tool in the management of many physiological and psychological conditions.
Three recent articles highlight the successful use of acupuncture in very unique areas of practice.
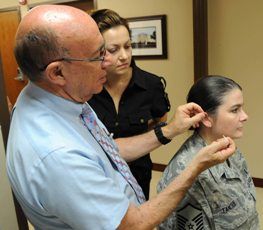 Richard Niemtzow, MD, and his colleagues describe the use of acupuncture as part of an integrative approach to assisting veterans struggling with PTDS, while Brenda Golianu MD, Jennie Seybold MD and Christina Almgren, PNP, found it helpful in weaning infants off of opioids and sedatives following surgical procedures.
Richard Niemtzow, MD, and his colleagues describe the use of acupuncture as part of an integrative approach to assisting veterans struggling with PTDS, while Brenda Golianu MD, Jennie Seybold MD and Christina Almgren, PNP, found it helpful in weaning infants off of opioids and sedatives following surgical procedures.
Dr. Golianu and her colleague, Kristin Sparrow MD, also looked at the effect of acupuncture on reducing physiological stress over time by tracking heart rate variance (HRV).
Although the concentrations for each of these studies are unrelated and the methods of treatment varied, all three showed strong positive results. None reported any adverse reactions –other than crying in two infants! This suggests that acupuncture can be useful adjunctive therapy for a wide assortment of medical concerns in people of all ages.
Reducing Stress, Raising HRV:
According to Sparrow and Golianu, Ancient Chinese Medicine practitioners recognized what we now know from quantitative analysis: that a machine-like regularity of heart rate is a sign of disease, age, and stress.
The two Stanford University researchers were interested in uncovering a possible connection between acupuncture and reduced physiological stress. They hypothesize that an increase in heart rate variance (HRV) during treatment (as well as cumulative long-term HRV improvements) would be a good marker for a reduction of physiological stress in response to acupuncture. They undertook a retrospective, uncontrolled observational study of ten patients being treated in a private acupuncture clinic for hypertension. The number and frequency of appointments varied a great deal between each client. In all cases, they gathered blood pressure readings prior to acupuncture, as well as HRV measurements recorded 20 minutes post-needling.
The results were primarily positive. The majority of patients saw a decrease in blood pressure as well as an increase in their heart rate variance –both positive health indicators (Sparrow K, Golianu B. Med Acupunct. 2014; 26(5): 286-294).
Only one patient did not see any improvement. The authors note that typically about 20% of all people do not respond to acupuncture therapy. While 20% may sound high, it is important to keep in mind that many commonly prescribed medications are also ineffective in large numbers of people. For example, in the case of statin drugs, the number needed to treat (NNT) ratio stands at 1 in 83 for prevention of death, and 1 in 125 for prevention of a stroke (http://www.thennt.com/nnt/statins-for-heart-disease-prevention-with-known-heart-disease/“>Newman D, et al. The NNT Group).
Drs. Sparrow and Golianu admit their study raised more questions than it answered.
For example, they wonder why there seemed to be cumulative changes over time, and whether this development reflects additional physiologic changes taking place.
They also admit that they are still uncertain about whether the observed HRV changes have sufficient clinical significance. That being said, the overall implications of this study suggest that acupuncture may be an effective method of reducing physiological stress. If that is the case, it makes sense to include acupuncture as part of any effort to improve mood, lower cardiovascular risk, increase immune system function, and reduce systemic inflammation.
Acupuncture “Cocktails” for PTSD:
Acupuncture definitely has a role to play in the care of people exposed to high- crisis events, such as natural disasters or battlefield trauma.
Col. Richard Niemtzow MD, PhD, MPH, a pioneer in the use of acupuncture in the military, and creator of Battlefield Acupuncture (BFA), notes that at Camp Leatherneck (a Marie Corps base in southern Afghanistan) health care practitioners are now using techniques such as his BFA, and Koffman’s https://www.researchgate.net/publication/264852234_Downrange_Acupuncture“>Acupuncture Cocktail to treat soldiers, particularly those injured by explosives.
Niemtzow explains that his acupuncture protocols are not intended to replace conventional medical care for war-related injuries, “but to assist in pain relief and in many cases, eliminate the need for pain medication.” His Battlefield Acupuncture system is designed for quick learning and easy deployment.
The “Koffman Cocktail,” developed by US Navy Capt. Robert Koffman, MD, is a hybrid of multiple auricular acupuncture techniques tailored for quick application to a wide range of common pain-related conditions.
“Everybody in the military experiences pain, lives with pain,” says Capt. Koffman, in a paper reviewing his approach.
Some of these same protocols have been used to effectively relieve pain and bring calm following natural disasters, such as hurricane Katrina and the Haiti earthquake.
In addition to pain reduction in the field, there are specific acupuncture protocols that can be used to help alleviate symptoms of PTSD, for example, the Helms’ Auricular Trauma Protocol developed by Joseph Helms, MD. Dr. Helms is one of the first medical doctors to take on the daunting task of “translating” acupuncture from its traditional Chinese cultural contacts into a conceptual framework accessible to conventionally-trained Western doctors.
Veterans struggling with PTSD may benefit greatly by getting connected with one of the many free acupuncture clinics offered at various times and locations throughout the US. This opportunity is generally available to both service members and their families.
For more information, one should look for the http://acuwithoutborders.org/veteransprogram.php“>Military Stress Recovery Project (MSRP) hosted by Acupuncturist Without Boarders. Their website provides a comprehensive list of locations.
Dr. Niemtzow has completed a yet-to-be published study comparing the fMRI scans of central nervous system activity in subjects without and with acupuncture needles. He says that the Battlefield Acupuncture treatment protocol produced significant attenuation of activity in the cingulate gyrus, thalamus, hypothalamus, and other areas. This correlates to a reduction of pain. Dr. Niemtzow also mentions another study using infrared spectroscopy that shows oxygen levels in the brain may be influenced by BFA.
Acupuncture in the NICU
Perhaps the most impressive acupuncture results are from a pilot study of 10 pediatric cases conducted by Brenda Golianu, MD, Jeannie Seybold, MD and Christina Almgren, PNP, of Stanford University Medical Center.
The objective was to determine if acupuncture would reduce pain med withdrawal symptoms and agitation in neonates and infants. The patients, aged 1 month – 15 months, were recovering from various surgical procedures, including a heart transplant in one, and a congenital diaphragmatic hernia repair in another. Most of these young patients were intubated and having difficulty with feeding.
The authors explain that infants have an increased sensitivity to pain and therefore often require high doses of pain 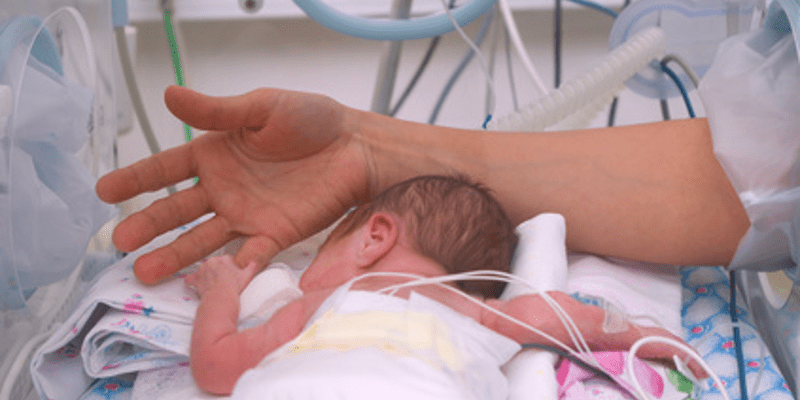 medications and sedatives following significant surgery. At the outset of this study each baby had been receiving between twofold and tenfold the recommended starting doses of opioids and benzodiazepines.
medications and sedatives following significant surgery. At the outset of this study each baby had been receiving between twofold and tenfold the recommended starting doses of opioids and benzodiazepines.
Dr. Golianu also notes that 80% of pediatric intensive care patients experience symptoms of withdrawal once the medication is stopped.
Acupuncture is used worldwide in detoxification clinics for adults, but there have been very few studies regarding its use in children. The Withdrawal Assessment Tool -1 (WAT-1) monitors agitation; muscle tone; yawning or sneezing; tremor; diaphoresis; repetitive movements; vomiting; fever; and watery stools as indicators of withdrawal. Scores fall between 0-11, with numbers greater than 3 requiring consideration for rescue dosing.
During this study each patient received auricular acupuncture daily for five days, with the exception of Case #2, who was discharged after 3 days of treatment. Needles were manually placed by either Dr. Golianu or Dr. Seybold, both of whom are acupuncture-certified pediatric anesthesiologists. After 15 minutes, needles were removed and acupressure beads were placed and maintained on treatment points for 24 hours.
The rate and degree of response varied slightly between patients. However, the authors found that within 24 hours of acupuncture treatment, 100% of the babies had experienced reductions in the amount of opioid medications needed to control agitation. They report an 89% reduction in the number of pain med doses given during the 48 hours of following acupuncture.
The most rapid improvement was seen in Case #2, a 5 month old who had undergone a heart transplant several weeks prior. The infant had been vomiting (approximately 5 times per 24 hours). The authors attributed the nausea to opioid withdrawal. Twenty-four hours following the initial acupuncture treatment, the baby had ceased vomiting and WAT-1 score had dropped from 4 to 0. They continued treatment for three days, after which this patient was discharged to go home.
The slowest rate of improvement was seen in Case #4, a 7-month-old (former 31-week premature) infant with a multitude of complex conditions, including Klippel-Feil syndrome and transposition of the great arteries. The child had undergone an arterial-switch procedure as well as a tracheostomy for mechanical ventilation and placement of a colostomy due to an imperforate anus.
Sixteen days after the colostomy, the baby continued to have severe breathing spasms, general agitation, and had poor feeding tolerance. In the 24 hours prior to acupuncture, this child required 8 additional as-needed sedative doses, including 2 muscle relaxants.
Follow the first treatment, only 5 as-needed doses were required, including 1 muscle relaxant. The infant’s WAT-1 score dropped from 7 to 3. As-needed doses continued to decline each day, and after 3 days of treatment no as-needed doses were required.
Golianu and Seybold note that all of the babies tolerated the acupuncture treatments well. In aggregate, the cohort experienced a steep reduction in as-needed medications, many were extubated, and feeding tolerance improved.
The authors hypothesize that children may require less needle stimulation than adults because their Qi may be more responsive to stimuli; therefore they may see more dramatic and rapid results.
Moving forward there is still much to learn about the body’s mechanistic response to acupuncture.
The difficulty in conducting controlled trials for such a personalized system of treatment means that we may need to develop new methods of research.
In the mean time, for patients who need additional support in managing physiological or psychological symptoms, acupuncture may well be a helpful addition to other therapies.
END







